Human Physiology/The female reproductive system
Editing of this page by new or unregistered users is currently disabled due to vandalism. See the protection log for more details. If you cannot edit this page and you wish to make a change, you can request an edit, discuss changes on the discussion page, request unprotection, log in, or create an account. |
Homeostasis — Cells — Integumentary — Nervous — Senses — Muscular — Blood — Cardiovascular — Immune — Urinary — Respiratory — Gastrointestinal — Nutrition — Endocrine — Reproduction (male) — Reproduction (female) — Pregnancy — Genetics — Development — Answers
Introduction
All living things reproduce. This is something that sets the living apart from non-living. Even though the reproductive system is essential to keeping a species alive, it is not essential to keeping an individual alive. This chapter describes the different parts of the female reproductive system: the organs involved in the process of reproduction, hormones that regulate a woman's body, the menstrual cycle, ovulation and pregnancy, the female's role in genetic division, birth control, sexually transmitted diseases and other diseases and disorders.
Reproduction
Reproduction can be defined as the process by which an organism continues its species. In the human reproductive process, two kinds of sex cells ( gametes), are involved: the male gamete (sperm), and the female gamete (egg or ovum). These two gametes meet within the female's uterine tubes located one on each side of the upper pelvic cavity, and begin to create a new individual. The female needs a male to fertilize her egg; she then carries offspring through pregnancy and childbirth.
Similarities between male and female reproductive systems
The reproductive systems of the male and female have some basic similarities and some specialized differences. They are the same in that most of the reproductive organs of both sexes develop from similar embryonic tissue, meaning they are homologous. Both systems have gonads that produce (sperm and egg or ovum) and sex organs. And both systems experience maturation of their reproductive organs, which become functional during puberty as a result of the gonads secreting sex hormones.
In short, this is a known list of sex organs that evolve from the same tissues in a human life.
| Undifferentiated | Male | Female |
|---|---|---|
| Gonad | Testis | Ovary |
| Müllerian duct | Appendix testis | Fallopian tubes |
| Müllerian duct | Prostatic utricle | Uterus, proximal |
| Wolffian duct | Rete testis | Rete ovarii |
| Mesonephric tubules | Efferent ducts | Epoophoron |
| Wolffian duct | Epididymis | Gartner's duct |
| Wolffian duct | Vas deferens | |
| Wolffian duct | Seminal vesicle | |
| Wolffian duct | Prostate | Skene's glands |
| Urogenital sinus | Bladder, urethra | Bladder, urethra, distal |
| Urogenital sinus | Bulbourethral gland | Bartholin's gland |
| Genital swelling | Scrotum | Labia majora |
| Urogenital folds | Distal urethra | Labia minora |
| Genital tubercle | Penis | Clitoris |
| Prepuce | Clitoral hood | |
| Bulb of penis | Vestibular bulbs | |
| Glans penis | Clitoral glans | |
| Crus of penis | Clitoral crura |
Differences between male and female reproductive systems
The differences between the female and male reproductive systems are based on the functions of each individual's role in the reproduction cycle. A male who is healthy, and sexually mature, continuously produces sperm. The development of women's "eggs" are arrested during fetal development. This means she is born with a predetermined number of oocytes and cannot produce new ones.
At about 5 months gestation, the ovaries contain approximately six to seven million oogonia, which initiate meiosis. The oogonia produce primary oocytes that are arrested in prophase I of meiosis from the time of birth until puberty. After puberty, during each menstrual cycle, one or several oocytes resume meiosis and undergo their first meiotic division during ovulation. This results in the production of a secondary oocyte and one polar body. The meiotic division is arrested in metaphase II. Fertilization triggers completion of the second meiotic division and the result is one ovum and an additional polar body.
The ovaries of a newborn baby girl contain about one million oocytes. This number declines to 400,000 to 500,000 by the time puberty is reached. On average, 500-1000 oocytes are ovulated during a woman's reproductive lifetime.
When a young woman reaches puberty around age 10 to 13, a promary oocyte is discharged from one of the ovaries every 28 days. This continues until the woman reaches menopause, usually around the age of 50 years. Occytes are present at birth, and age as a woman ages.
- Female Reproductive System
- Produces eggs (ova)
- Secretes sex hormones
- Receives the male spermatazoa during
- Protects and nourishes the fertilized egg until it is fully developed
- Delivers fetus through birth canal
- Provides nourishment to the baby through milk secreted by mammary glands in the breast
External Genitals

Vulva
The external female genitalia is referred to as vulva. It consists of the labia majora and labia minora (while these names translate as "large" and "small" lips, often the "minora" can protrude outside the "majora"), mons pubis, clitoris, opening of the urethra (meatus), vaginal vestibule, vestibular bulbs, vestibular glands.
The term "vagina" is often improperly used as a generic term to refer to the vulva or female genitals, even though - strictly speaking - the vagina is a specific internal structure and the vulva is the exterior genitalia only. Calling the vulva the vagina is akin to calling the mouth the throat.
Mons Veneris
The mons veneris, Latin for "mound of Venus" (Roman Goddess of love) is the soft mound at the front of the vulva (fatty tissue covering the pubic bone). It is also referred to as the mons pubis. The mons veneris protects the pubic bone and vulva from the impact of sexual intercourse. After puberty, it is covered with pubic hair, usually in a triangular shape. Heredity can play a role in the amount of pubic hair an individual grows.
Labia Majora
The labia majora are the outer "lips" of the vulva. They are pads of loose connective and adipose tissue, as well as some smooth muscle. The labia majora wrap around the vulva from the mons pubis to the perineum. The labia majora generally hides, partially or entirely, the other parts of the vulva. There is also a longitudinal separation called the pudendal cleft. These labia are usually covered with pubic hair. The color of the outside skin of the labia majora is usually close to the overall color of the individual, although there may be some variation. The inside skin is usually pink to light brown. They contain numerous sweat and oil glands. It has been suggested that the scent from these oils are sexually arousing.
Labia Minora
Medial to the labia majora are the labia minora. The labia minora are the inner lips of the vulva. They are thin stretches of tissue within the labia majora that fold and protect the vagina, urethra, and clitoris. The appearance of labia minora can vary widely, from tiny lips that hide between the labia majora to large lips that protrude. There is no pubic hair on the labia minora, but there are sebaceous glands. The two smaller lips of the labia minora come together longitudinally to form the prepuce, a fold that covers part of the clitoris. The labia minora protect the vaginal and urethral openings. Both the inner and outer labia are quite sensitive to touch and pressure.
Clitoris

The clitoris, visible as the small white oval between the top of the labia minora and the clitoral hood, is a small body of spongy tissue that functions solely for sexual pleasure. Only the tip or glans of the clitoris shows externally, but the organ itself is elongated and branched into two forks, the crura, which extend downward along the rim of the vaginal opening toward the perineum. Thus the clitoris is much larger than most people think it is, about 4" long on average.
The clitoral glans or external tip of the clitoris is protected by the prepuce, or clitoral hood, a covering of tissue similar to the foreskin of the male penis. However, unlike the penis, the clitoris does not contain any part of the urethra.
During sexual excitement, the clitoris erects and extends, the hood retracts, making the clitoral glans more accessible. The size of the clitoris is variable between women. On some, the clitoral glans is very small; on others, it is large and the hood does not completely cover it.
Urethra
The opening to the urethra is just below the clitoris. Although it is not related to sex or reproduction, it is included in the vulva. The urethra is actually used for the passage of urine. The urethra is connected to the bladder. In females the urethra is 1.5 inches long, compared to males whose urethra is 8 inches long. Because the urethra is so close to the anus, women should always wipe themselves from front to back to avoid infecting the vagina and urethra with bacteria. This location issue is the reason for bladder infections being more common among females.
Hymen
The hymen is a thin fold of mucous membrane that separates the lumen of the vagina from the urethral sinus. Sometimes it may partially cover the vaginal orifice. The hymen is usually perforated during later fetal development.
Because of the belief that first vaginal penetration would usually tear this membrane and cause bleeding, its "intactness" has been considered a guarantor of virginity. However, the hymen is a poor indicator of whether a woman has actually engaged in sexual intercourse because a normal hymen does not completely block the vaginal opening. The normal hymen is never actually "intact" since there is always an opening in it. Furthermore, there is not always bleeding at first vaginal penetration. The blood that is sometimes, but not always, observed after first penetration can be due to tearing of the hymen, but it can also be from injury to nearby tissues.
A tear to the hymen, medically referred to as a "transection," can be seen in a small percentage of women or girls after first penetration. A transection is caused by penetrating trauma. Masturbation and tampon insertion can, but generally are not forceful enough to cause penetrating trauma to the hymen. Therefore, the appearance of the hymen is not a reliable indicator of virginity or chastity.
Perineum
The perineum is the short stretch of skin starting at the bottom of the vulva and extending to the anus. It is a diamond shaped area between the symphysis pubis and the coccyx. This area forms the floor of the pelvis and contains the external sex organs and the anal opening. It can be further divided into the urogenital triangle in front and the anal triangle in back.
The perineum in some women may tear during the birth of an infant and this is apparently natural. Some physicians however, may cut the perineum preemptively on the grounds that the "tearing" may be more harmful than a precise cut by a scalpel. If a physician decides the cut is necessary, they will perform it. The cut is called an episiotomy.
Internal Genitals
Vagina
The vagina is a muscular, hollow tube that extends from the vaginal opening to the cervix of the uterus. It is situated between the urinary bladder and the rectum. It is about three to five inches long in a grown woman. The muscular wall allows the vagina to expand and contract. The muscular walls are lined with mucous membranes, which keep it protected and moist. A thin sheet of tissue with one or more holes in it, called the hymen, partially covers the opening of the vagina. The vagina receives sperm during sexual intercourse from the penis. The sperm that survive the acidic condition of the vagina continue on through to the fallopian tubes where fertilization may occur.
The vagina is made up of three layers, an inner mucosal layer, a middle muscularis layer, and an outer fibrous layer. The inner layer is made of vaginal rugae that stretch and allow penetration to occur. These also help with stimulation of the penis. microscopically the vaginal rugae has glands that secrete an acidic mucus (pH of around 4.0.) that keeps bacterial growth down. The outer muscular layer is especially important with delivery of a fetus and placenta.
- Purposes of the Vagina
- Receives a male's erect penis and semen during sexual intercourse.
- Pathway through a woman's body for the baby to take during childbirth.
- Provides the route for the menstrual blood (menses) from the uterus, to leave the body.
- May hold forms of birth control, such as a diaphragm, FemCap, Nuva Ring, or female condom.
Pelvic inflammatory disease (PID) is a widespread infection that originates in the vagina and uterus and spreads to the uterine tubes, ovaries, and ultimately the pelvic peritoneum. This condition, which occurs in about 10% of women is usually caused by chlamydial or gonorrheal infection, other bacteria infecting the vagina may be involved as well. Signs and symptoms include tenderness of the lower abdomen, fever, and a vaginal discharge. Even a single episode of PID can cause infertility, due to scarring that blocks the uterine tubes. Therefore, patients are immediately given broad-spectrum antibiotics whenever PID is suspected.
Cervix
The cervix (from Latin "neck") is the lower, narrow portion of the uterus where it joins with the top end of the vagina. Where they join together forms an almost 90 degree curve. It is cylindrical or conical in shape and protrudes through the upper anterior vaginal wall. Approximately half its length is visible with appropriate medical equipment; the remainder lies above the vagina beyond view. It is occasionally called "cervix uteri", or "neck of the uterus".
During menstruation, the cervix stretches open slightly to allow the endometrium to be shed. This stretching is believed to be part of the cramping pain that many women experience. Evidence for this is given by the fact that some women's cramps subside or disappear after their first vaginal birth because the cervical opening has widened.
The portion projecting into the vagina is referred to as the portio vaginalis or ectocervix. On average, the ectocervix is three cm long and two and a half cm wide. It has a convex, elliptical surface and is divided into anterior and posterior lips. The ectocervix's opening is called the external os. The size and shape of the external os and the ectocervix varies widely with age, hormonal state, and whether the woman has had a vaginal birth. In women who have not had a vaginal birth the external os appears as a small, circular opening. In women who have had a vaginal birth, the ectocervix appears bulkier and the external os appears wider, more slit-like and gaping.
The passageway between the external os and the uterine cavity is referred to as the endocervical canal. It varies widely in length and width, along with the cervix overall. Flattened anterior to posterior, the endocervical canal measures seven to eight mm at its widest in reproductive-aged women. The endocervical canal terminates at the internal os which is the opening of the cervix inside the uterine cavity.
During childbirth, contractions of the uterus will dilate the cervix up to 10 cm in diameter to allow the child to pass through. During orgasm, the cervix convulses and the external os dilates.
Uterus
The uterus is shaped like an upside-down pear, with a thick lining and muscular walls. Located near the floor of the pelvic cavity, it is hollow to allow a blastocyte, or fertilized egg, to implant and grow. It also allows for the inner lining of the uterus to build up until a fertilized egg is implanted, or it is sloughed off during menses.
The uterus contains some of the strongest muscles in the female body. These muscles are able to expand and contract to accommodate a growing fetus and then help push the baby out during labor. These muscles also contract rhythmically during an orgasm in a wave like action. It is thought that this is to help push or guide the sperm up the uterus to the fallopian tubes where fertilization may be possible.
The uterus is only about three inches long and two inches wide, but during pregnancy it changes rapidly and dramatically. The top rim of the uterus is called the fundus and is a landmark for many doctors to track the progress of a pregnancy. The uterine cavity refers to the fundus of the uterus and the body of the uterus.
Helping support the uterus are ligaments that attach from the body of the uterus to the pelvic wall and abdominal wall. During pregnancy the ligaments prolapse due to the growing uterus, but retract after childbirth. In some cases after menopause, they may lose elasticity and uterine prolapse may occur. This can be fixed with surgery.
Some problems of the uterus include uterine fibroids, pelvic pain (including endometriosis, adenomyosis), pelvic relaxation (or prolapse), heavy or abnormal menstrual bleeding, and cancer. It is only after all alternative options have been considered that surgery is recommended in these cases. This surgery is called hysterectomy. Hysterectomy is the removal of the uterus, and may include the removal of one or both of the ovaries. Once performed it is irreversible. After a hysterectomy, many women begin a form of alternate hormone therapy due to the lack of ovaries and hormone production.
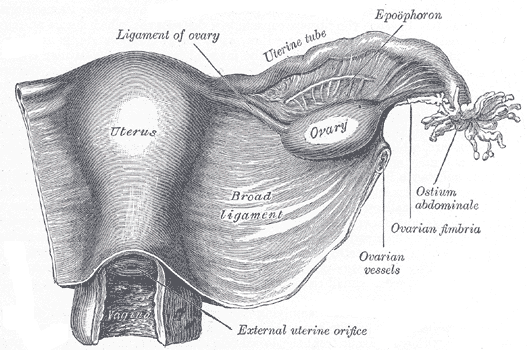
Fallopian Tubes
At the upper corners of the uterus are the fallopian tubes. There are two fallopian tubes, also called the uterine tubes or the oviducts. Each fallopian tube attaches to a side of the uterus and connects to an ovary. They are positioned between the ligaments that support the uterus. The fallopian tubes are about four inches long and about as wide as a piece of spaghetti. Within each tube is a tiny passageway no wider than a sewing needle. At the other end of each fallopian tube is a fringed area that looks like a funnel. This fringed area, called the infundibulum, lies close to the ovary, but is not attached. The ovaries alternately release an egg. When an ovary does ovulate, or release an egg, it is swept into the lumen of the fallopian tube by the fimbriae.
Once the egg is in the fallopian tube, tiny hairs in the tube's lining help push it down the narrow passageway toward the uterus. The oocyte, or developing egg cell, takes four to five days to travel down the length of the fallopian tube. If enough sperm are ejaculated during sexual intercourse and there is an oocyte in the fallopian tube, fertilization will occur. After fertilization occurs, the zygote, or fertilized egg, will continue down to the uterus and implant itself in the uterine wall where it will grow and develop.
If a zygote doesn't move down to the uterus and implants itself in the fallopian tube, it is called a ectopic or tubal pregnancy. If this occurs, the pregnancy will need to be terminated to prevent permanent damage to the fallopian tube, possible hemorrhage and possible death of the mother.
Mammary glands
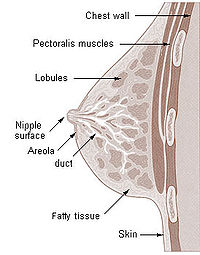
Mammary glands are the organs that produce milk for the sustenance of a baby. These exocrine glands are enlarged and modified sweat glands.
Structure
The basic components of the mammary gland are the alveoli (hollow cavities, a few millimetres large) lined with milk-secreting epithelial cells and surrounded by myoepithelial cells. These alveoli join up to form groups known as lobules, and each lobule has a lactiferous duct that drains into openings in the nipple. The myoepithelial cells can contract, similar to muscle cells, and thereby push the milk from the alveoli through the lactiferous ducts towards the nipple, where it collects in widenings (sinuses) of the ducts. A suckling baby essentially squeezes the milk out of these sinuses.
The development of mammary glands is controlled by hormones. The mammary glands exist in both sexes, but they are rudimentary until puberty when - in response to ovarian hormones - they begin to develop in the female. Estrogen promotes formation, while testosterone inhibits it.
At the time of birth, the baby has lactiferous ducts but no alveoli. Little branching occurs before puberty when ovarian estrogens stimulate branching differentiation of the ducts into spherical masses of cells that will become alveoli. True secretory alveoli only develop in pregnancy, where rising levels of estrogen and progesterone cause further branching and differentiation of the duct cells, together with an increase in adipose tissue and a richer blood flow.
Colostrum is secreted in late pregnancy and for the first few days after giving birth. True milk secretion (lactation) begins a few days later due to a reduction in circulating progesterone and the presence of the hormone prolactin. The suckling of the baby causes the release of the hormone oxytocin which stimulates contraction of the myoepithelial cells.
The cells of mammary glands can easily be induced to grow and multiply by hormones. If this growth runs out of control, cancer results. Almost all instances of breast cancer originate in the lobules or ducts of the mammary glands.
| STRUCTURE | LOCATION & DESCRIPTION | FUNCTION |
|---|---|---|
| Breasts | Upper chest one on each side containing alveolar cells (milk production), myoepithelial cells (contract to expel milk), and duct walls (help with extraction of milk). | Lactation milk/nutrition for newborn. |
| Cervix | The lower narrower portion of the uterus. | During childbirth, contractions of the uterus will dilate the cervix up to 10 cm in diameter to allow the child to pass through. During orgasm, the cervix convulses and the external os dilates |
| Clitoris | Small erectile organ directly in front of the vestibule. | Sexual excitation, engorged with blood. |
| Fallopian tubes | Extending upper part of the uterus on either side. | Egg transportation from ovary to uterus (fertilization usually takes place here). |
| Hymen | Thin membrane that partially covers the vagina in young females. | |
| Labia majora | Outer skin folds that surround the entrance to the vagina. | Lubrication during mating. |
| Labia minora | Inner skin folds that surround the entrance to the vagina. | Lubrication during mating. |
| Mons | Mound of skin and underlying fatty tissue, central in lower pelvic region | |
| Ovaries (female gonads) | Pelvic region on either side of the uterus. | Provides an environment for maturation of oocyte. Synthesizes and secretes sex hormones (estrogen and progesterone). |
| Perineum | Short stretch of skin starting at the bottom of the vulva and extending to the anus. | |
| Urethra | Pelvic cavity above bladder, tilted. | Passage of urine. |
| Uterus | Center of pelvic cavity. | To house and nourish developing human. |
| Vagina | Canal about 10-8 cm long going from the cervix to the outside of the body. | Receives penis during mating. Pathway through a womans body for the baby to take during childbirth. Provides the route for the menstrual blood (menses) from the uterus, to leave the body. May hold forms of birth control, such as an IUD, diaphragm, neva ring, or female condom |
| Vulva | Surround entrance to the reproductive tract.(encompasses all external genitalia) | |
| Endometrium | The innermost layer of uterine wall. | Contains glands that secrete fluids that bathe the utrine lining. |
| Myometrium | Smooth muscle in uterine wall. | Contracts to help expel the baby. |
The Female Reproductive Cycle
Towards the end of puberty, girls begin to release eggs as part of a monthly period called the female reproductive cycle, or menstrual cycle (menstrual referring to "monthly"). Approximately every 28 days, during ovulation, an ovary sends a tiny egg into one of the fallopian tubes. Unless the egg is fertilized by a sperm while in the fallopian in the two to three days following ovulation, the egg dries up and leaves the body about two weeks later through the vagina. This process is called menstruation. Blood and tissues from the inner lining of the uterus (the endometrium) combine to form the menstrual flow, which generally lasts from four to seven days. The first period is called menarche. During menstruation arteries that supply the lining of the uterus constrict and capillaries weaken. Blood spilling from the damaged vessels detaches layers of the lining, not all at once but in random patches. Endometrium mucus and blood descending from the uterus, through the liquid creates the menstruation flow.

The reproductive cycle can be divided into an ovarian cycle and a uterine cycle (compare ovarian histology and uterine histology in the diagram on the right). During the uterine cycle, the endometrial lining of the uterus builds up under the influence of increasing levels of estrogen (labeled as estradiol in the image). Follicles develop, and within a few days one matures into an ovum, or egg. The ovary then releases this egg, at the time of ovulation. After ovulation the uterine lining enters a secretory phase, or the ovarian cycle, in preparation for implantation, under the influence of progesterone. Progesterone is produced by the corpus luteum (the follicle after ovulation) and enriches the uterus with a thick lining of blood vessels and capillaries so that it can sustain the growing fetus. If fertilization and implantation occur, the embryo produces Human Chorionic Gonadotropin (HCG), which maintains the corpus luteum and causes it to continue producing progesterone until the placenta can take over production of progesterone. Hence, progesterone is "pro gestational" and maintains the uterine lining during all of pregnancy. If fertilization and implantation do not occur the corpus luteum degenerates into a corpus albicans, and progesterone levels fall. This fall in progesterone levels cause the endometrium lining to break down and sluff off through the vagina. This is called menstruation, which marks the low point for estrogen activity and is the starting point of a new cycle.
Common usage refers to menstruation and menses as a period. This bleeding serves as a sign that a woman has not become pregnant. However, this cannot be taken as certainty, as sometimes there is some bleeding in early pregnancy. During the reproductive years, failure to menstruate may provide the first indication to a woman that she may have become pregnant.
Menstruation forms a normal part of a natural cyclic process occurring in healthy women between puberty and the end of the reproductive years. The onset of menstruation, known as menarche, occurs at an average age of 12, but is normal anywhere between 8 and 16. Factors such as heredity, diet, and overall health can accelerate or delay the onset of menarche.
Signs of ovulation
The female body produces outward signs that can be easily recognized at the time of ovulation. The two main signs are thinning of the cervical mucus and a slight change in body temperature.
Thinning of the Cervical Mucus
After menstruation and right before ovulation, a woman will experience an increase of cervical mucus. At first, it will be thick and yellowish in color and will not be very plentiful. Leading up to ovulation, it will become thinner and clearer. On or around the day of ovulation, the cervical mucus will be very thin, clear and stretchy. It can be compared to the consistency of egg whites. This appearance is known as 'spinnbarkeit'.
Temperature Change
A woman can also tell the time of ovulation by taking her basal body temperature daily. This is a temperature taken with a very sensitive thermometer first thing in the morning before the woman gets out of bed. The temperature is then tracked to show changes. In the uterine cycle, a normal temperature will be around 97.0 – 98.0. The day of ovulation the temperature spikes down, usually into the 96.0 – 97.0 range and then the next morning it will spike up to normal of around 98.6 and stay in that range until menstruation begins.
Both of these methods are used for conception and contraception. They are more efficient in conception due to the fact that sperm can live for two to three days inside of the fallopian tubes. A woman could be off by a couple of days in her calculations and still become pregnant.
Menopause is the physiological cessation of menstrual cycles associated with advancing age. Menopause is sometimes referred to as "the change of life" or climacteric. Menopause occurs as the ovaries stop producing estrogen, causing the reproductive system to gradually shut down. As the body adapts to the changing levels of natural hormones, vasomotor symptoms such as hot flashes and palpitations, psychological symptoms such as increased depression, anxiety, irritability, mood swings and lack of concentration, and atrophic symptoms such as vaginal dryness and urgency of urination appear. Together with these symptoms, the woman may also have increasingly scanty and erratic menstrual periods.
Technically, menopause refers to the cessation of menses; the gradual process through which this occurs, which typically takes a year but may last as little as six months or more than five years, is known as climacteric. A natural or physiological menopause is that which occurs as a part of a woman's normal aging process. However, menopause can be surgically induced by such procedures as hysterectomy.
The average onset of menopause is 50.5 years, but some women enter menopause at a younger age, especially if they have suffered from cancer or another serious illness and undergone chemotherapy. Premature menopause is defined as menopause occurring before the age of 40, and occurs in 1% of women. Other causes of premature menopause include autoimmune disorders, thyroid disease, and diabetes mellitus.
Premature menopause is diagnosed by measuring the levels of follicle stimulating hormone (FSH) and luteinizing hormone (LH). The levels of these hormones will be higher if menopause has occurred. Rates of premature menopause have been found to be significantly higher in both fraternal and identical twins; approximately 5% of twins reach menopause before the age of 40. The reasons for this are not completely understood. Post-menopausal women are at increased risk of osteoporosis.
Perimenopause refers to the time preceding menopause, during which the production of hormones such as estrogen and progesterone diminish and become more irregular. During this period fertility diminishes. Menopause is arbitrarily defined as a minimum of twelve months without menstruation. Perimenopause can begin as early as age 35, although it usually begins much later. It can last for a few months or for several years. The duration of perimenopause cannot be predicted in advance.
Premenstrual Syndrome (PMS) It is common for women to experience some discomfort in the days leading up to their periods. PMS usually is at its worst the seven days before a period starts and can continue through the end of the period. PMS includes both physical and emotional symptoms: acne, bloating, fatigue, backaches, sore breasts, headaches, constipation, diarrhea, food cravings, depression, irritability, difficulty concentrating or handling stress.
Ovarian and Uterine Cycles in the Nonpregnant Woman

| Ovarian Cycle | Events | Uterine Cycle | Events |
|---|---|---|---|
| Follicular phase - Days 1-13 | FSH secretion begins. | Menstruation - Days 2-5 | Endometrium breaks down. |
| Follicle maturation occurs. | Proliferative phase - Days 6-13 | Endometrium rebuilds. | |
| Estrogen secretion is prominent. | |||
| Ovulation - Day 14* | LH spike occurs. | ||
| Luteal phase - Days 15-28 | LH secretion continues. | Secretory phase - Days 15-28 | Endometrial thickens, and glands are secretory. |
| Corpus luteum forms. | |||
| Progesterone secretion is prominent. |
(*)Assuming a 28 day cycle.
There are two phases of the ovarian cycle the follicular phase and the luteal phase. In the follicular phase about 10-25 follicles are taken from preantral or early antrial follicles to develop further. Seven days later the dominant follicle is selected to develop to full maturity. This is the pre-cursor for ovulation. Follicles themselves secrete FSH and estrogen, and these two hormones stimulate follicular growth and development. Ovulation marks the beginning of the luteal phase. This is started by the wall of the Graffian follicle to rupture and cause a flow of antral fluid that will carry the oocyte to the ovary's surface. The ruptured follicle is then turned into a gland (corpus luteum). Which secretes estrogens and progesterone. This is all triggered by and abrupt change in plasma LH levels. After ovulation the released oocyte enters the uterine tube, where it will be either fertilized or discarded.
The uterine cycle operates in sync with the ovarian cycle and is divided into three phases. The first phase in the menstrual phase. It is named the menstrual phase because in corresponds with the shedding the uterine lining or more commonly called menstruation. The corpus luteum degenerates causing plasma estrogen and progesterone levels to decrease and in turn causes menstruation. Blood vessels in the outer most layer of the endometrium constrict and decrease blood flow to the tissues killing these tissues. After the tissues die they start to separate from the underlying endometrial tissues. Eventually the dead tissue is shed. This shedding of the tissues ruptures blood vessels and causes bleeding. Now we have the proliferative phase. During this phase the uterus renews itself and prepares for pregnancy. The endometrial tissue that is left after menstruation begins to grow. The endometrial glands grow and enlarge causing more blood vessels. The cervical canal has glands that secrete a thin mucous that helps deposited sperm. Estrogen promotes uterine changes in this phase. The last phase is the secretory phase. This is where the endometrium is transformed to make it the best environment for implantation and subsequent housing and nourishment of the developing embryo. By doing this the endometrium will do things like have an enriched blood supply, begin to secrete fluids rich in glycogen, and even form a plug at the end of the cervical canal so that microorganisms can not enter. These changes in the uterus are caused by progesterone, due to the corpus luteum. At the end of the secretory phase the corpus luteum degenerates, and progesterone levels fall. This will trigger menstruation.
Sexual Reproduction
Sexual reproduction is a type of reproduction that results in increasing genetic diversity of the offspring. In sexual reproduction, genes from two individuals are combined in random ways with each new generation. Sex hormones released into the body by the endocrine system signal the body when it is time to start puberty. The female and male reproductive systems are the only systems so vastly different that each sex has their own different organs. All other systems have "unisex" organs.
Reproduction is characterized by two processes. The first, meiosis, involves the halving of the 46 of chromosomes. The second process, fertilization, leads the fusion of two gametes and the restoration of the original number of chromosomes: 23 chromosomes from the paternal side and 23 from the maternal side. During meiosis, the chromosomes of each pair usually cross over to achieve genetic recombination.
Sexual reproduction cannot happen without the sexual organs called gonads. Both sexes have gonads: in females, the gonads are the ovaries. The female gonads produce female gametes (eggs); the male gonads produce male gametes (sperm). After an egg is fertilized by the sperm, the fertilized egg is called the zygote.
The fertilization usually occurs in the oviducts, but can happen in the uterus itself. The zygote then implants itself in the wall of the uterus, where it begins the processes of embryogenesis and morphogenesis. The womens body carries out this process of reproduction for 40 weeks, until delivery of the fetus from the uterus through the vagina (birth canal). Even after birth, the female continues with the reproduction process by supplying the milk to nourish the infant.
Infertility
Infertility is the inability to naturally conceive a child or the inability to carry a pregnancy to term. There are many reasons why a couple may not be able to conceive without medical assistance. Infertility affects approximately 15% of couples. Roughly 40% of cases involve a male contribution or factor, 40% involve a female factor, and the remaining 20% involve both sexes. Healthy couples in their mid-20s having regular sex have a one-in-four chance of getting pregnant in any given month. This is called "Fecundity".
Primary vs. secondary
According to the American Society for Reproductive Medicine, infertility affects about 6.1 million people in the United States, equivalent to 10% of the reproductive age population. Female infertility accounts for one third of infertility cases, male infertility for another third, combined male and female infertility for another 15%, and the remainder of cases are "unexplained.
"Secondary infertility" is difficulty conceiving after already having conceived and carried a normal pregnancy. Apart from various medical conditions (e.g. hormonal), this may come as a result of age and stress felt to provide a sibling for their first child. Technically, secondary infertility is not present if there has been a change of partners.
Factors of Infertility
Factors relating to female infertility are:
- General factors
- Diabetes mellitus,thyroid disorders,adrenal disease
- Significant liver,kidney disease
- Psychological factors
- Hypothalamic-pituitary factors:
- Kallmann syndrome
- Hypothalamic dysfunction
- Hyperprolactinemia
- Hypopituitarism
- Ovarian factors
- Polycystic ovary syndrome
- Anovulation
- Diminished ovarian reserve
- Luteal dysfunction
- Premature menopause
- Gonadal dysgenesis (Turner syndrome)
- Ovarian neoplasm
- Tubal/peritoneal factors
- Endometriosis
- Pelvic adhesions
- Pelvic inflammatory disease(PID, usually due to chlamydia)
- Tubal occlusion
- Uterine factors
- Uterine malformations
- Uterine fibroids (leiomyoma)
- Asherman's Syndrome
- Cervical factors
- Cervical stenosis
- Antisperm antibodies
- Insufficient cervical mucus (for the travel and survival of sperm)
- Vaginal factors
- Vaginismus
- Vaginal obstruction
- Genetic factors
- Various intersexuality|intersexed conditions, such as androgen insensitivity syndrome
Combined Infertility
In some cases, both the man and woman may be infertile or sub-fertile, and the couple's infertility arises from the combination of these factors. In other cases, the cause is suspected to be immunological or genetic; it may be that each partner is independently fertile but the couple cannot conceive together without assistance.
Unexplained Infertility
In about 15% of cases of infertility, investigation will show no abnormalities. In these cases abnormalities are likely to be present but not detected by current methods. Possible problems could be that the egg is not released at the optimum time for fertilization, that it may not enter the fallopian tube, sperm may not be able to reach the egg, fertilization may fail to occur, transport of the zygote may be disturbed, or implantation fails. It is increasingly recognized that egg quality is of critical importance.
Diagnosis of Infertility
Diagnosis of infertility begins with a medical history and physical exam. The healthcare provider may order tests, including the following:
- an endometrial biopsy, which tests the lining of the uterus
- hormone testing, to measure levels of female hormones
- laparoscopy, which allows the provider to see the pelvic organs
- ovulation testing, which detects the release of an egg from the ovary
- Pap smear, to check for signs of infection
- pelvic exam, to look for abnormalities or infection
- a postcoital test, which is done after sex to check for problems with secretions
- special X-ray tests
Treatment
- Fertility medication which stimulates the ovaries to "ripen" and release eggs (e.g. Clomifene|clomifene citrate, which stimulates ovulation)
- Surgery to restore potency of obstructed fallopian tubes (tuboplasty)
- Donor insemination which involves the woman being artificially inseminated or artificially inseminated with donor sperm.
- In vitro fertilization (IVF) in which eggs are removed from the woman, fertilized and then placed in the woman's uterus, bypassing the fallopian tubes. Variations on IVF include:
- Use of donor eggs and/or sperm in IVF. This happens when a couple's eggs and/or sperm are unusable, or to avoid passing on a genetic disease.
- Intracytoplasmic sperm injection (ICSI) in which a single sperm is injected directly into an egg; the fertilized egg is then placed in the woman's uterus as in IVF.
- Zygote intrafallopian transfer(ZIFT) in which eggs are removed from the woman, fertilized and then placed in the woman's fallopian tubes rather than the uterus.
- Gamete intrafallopian transfer(GIFT) in which eggs are removed from the woman, and placed in one of the fallopian tubes, along with the man's sperm. This allows fertilization to take place inside the woman's body.
- Other assisted reproductive technology (ART):
- Assisted hatching
- Fertility preservation
- Freezing (cryopreservation) of sperm, eggs, & reproductive tissue
- Frozen embryo transfer (FET)
- Alternative and complimentary treatments
- Acupuncture Recent controlled trials published in Fertility and Sterility have shown acupuncture to increase the success rate of IVF by as much as 60%. Acupuncture was also reported to be effective in the treatment of female anovular infertility, World Health Organization, Acupuncture: Review and Analysis of Reports on Controlled Trials (2002).
- Diet and supplements
- Healthy lifestyle
Types of Birth Control
Birth control is a regimen of one or more actions, devices, or medications followed in order to deliberately prevent or reduce the likelihood of a woman becoming pregnant. Methods and intentions typically termed birth control may be considered a pivotal ingredient to family planning. Mechanisms which are intended to reduce the likelihood of the fertilization of an ovum by a sperm may more specifically be referred to as contraception. Contraception differs from abortion in that the former prevents fertilization, while the latter terminates an already established pregnancy. Methods of birth control (e.g. the pill, IUDs, implants, patches, injections, vaginal ring and some others) which may prevent the implantation of an embryo if fertilization occurs are medically considered to be contraception. It is advised to talk with a doctor before choosing a contraceptive. If you have genetics problems or blood conditions, such as factor V leiden, certain contraceptives can be deadly.
| Type | Procedure | Method | Effectiveness | Risks |
|---|---|---|---|---|
| Abstinence | Refrain from sexual intercourse | No sperm in vagina | 100% | None |
| Rhythm Method | Intercourse is avoided for about an 8-day span every month in middle of her cycle, from about five days before ovulation to three days after ovulation. | fertilization is only possible during 8-day span in middle of menstrual cycle | 70-80% | None |
| Withdrawal | The man withdraws his penis from the vagina at just the right moment before ejaculation. | sperm are unable to enter vagina if male penis is removed at the right time | 70-80% | None |
| Tubal Ligation (Vasectomy) | Oviducts are cut and tied | No eggs in oviduct | Almost 99% | About 75% Irreversible |
| Hormonal IUD (intrauterine device) | Flexible, plastic coil inserted by physician | Releases small amounts of estrogen. In most cases, stops egg from developing and being released, but can also operate by killing a fertilized egg by preventing its implantation | About 99% | May cause infections, uterine perforation |
| Oral Contraceptive | Hormone medication taken daily | Stops release of FSH and LH, but can also operate by killing a fertilized egg by preventing its implantation | More than 90% | Blood clots, especially in smokers |
| Contraceptive Implants | Tubes of progesterone implanted under the skin | Stops release of FSH and LH, but can also operate by killing a fertilized egg by preventing its implantation | More than 90% | None known |
| Contraceptive Injections | Injections of hormones | Stops release of FSH and LH, but can also operate by killing a fertilized egg by preventing its implantation | About 99% | Possible osteoporosis |
| Diaphragm | Latex cup inserted into vagina to cover cervix before intercourse | Blocks entrance of sperm into uterus | With spermicide, about 90% | Latex or spermicide allergy |
| Cervical Cap | Latex cup held by suction over cervix | Delivers spermicide near cervix | Almost 85% | UTI, latex or spermicide allergy |
| Female Condom | Polyurethane liner fitted inside vagina | Blocks entrance of sperm into uterus and prevents STD’s | Almost 85% | None |
| Male Condom | soft sheath, made of latex or animal membrane, encloses penis, trapping ejaculated sperm | Blocks entrance of sperm into vagina and prevents STD's | 90% | None |
| Jellies, Cream, Foams | Spermicidal products inserted before intercourse | Kills large number of sperm | About 75% | UTI, allergy to spermicides |
| Natural Family Planning | Keep record of ovulation using various methods | Avoid sexual intercourse near ovulation | About 70% | None known |
| Douche | Vagina cleansed after intercourse | Washes out sperm | Less than 70% | None known |
| Plan B Pill | Pill taken after intercourse | Prevents release of egg, fertilization of egg, but can also operate by killing a fertilized egg by preventing its implantation | About 89% | Same as oral contraceptive |
Sexually Transmitted Diseases
Sexually transmitted diseases (STDs) are diseases or infections likely to be transmitted by sexual contact: vaginal intercourse, oral sex, and/or anal sex. Many STDs are (more easily) transmitted through the mucous membranes of the penis, vulva, and (less often) the mouth. The visible membrane covering the head of the penis is a mucous membrane, though, for those who are circumcised it is usually dry and produces no mucus (similar to the lips of the mouth). Mucous membranes differ from skin in that they allow certain pathogens (viruses or bacteria) into the body (more easily).
The probability of transmitting infections through sex is far greater than by more casual means of transmission, such as non-sexual contact—touching, sharing cutlery, and shaking hands. Although mucous membranes exist in the mouth as well as in the genitals, many STDs are more likely to be transmitted through oral sex than through deep kissing. Many infections that are easily transmitted from the mouth to the genitals or from the genitals to the mouth, are much harder to transmit from one mouth to another. With HIV, genital fluids happen to contain a great deal more of the pathogen than saliva. Some infections labeled as STDs can be transmitted by direct skin contact. Herpes simplex and HPV are both examples. Depending on the STD, a person who has the disease but has no symptoms may or may not be able to spread the infection. For example, a person is much more likely to spread herpes infection when blisters are present than when they are absent. However, a person can spread HIV infection at any time, even if he/she has not developed symptoms of AIDS.
All sexual behaviors that involve contact with the bodily fluids of another person should be considered to hold some risk of transmission of sexually transmitted diseases. Most attention has focused on controlling HIV, which causes AIDS, but each STD presents a different situation.
As may be noted from the name, sexually transmitted diseases are transmitted from one person to another by certain sexual activities rather than being actually caused by those sexual activities. Bacteria, fungi, protozoa or viruses are still the causative agents. It is not possible to catch any sexually transmitted disease from a sexual activity with a person who is not carrying a disease; conversely, a person who has an STD received it from contact (sexual or otherwise) with someone who is infected.
Although the likelihood of transmitting diseases by sexual activities varies a great deal, in general, all sexual activities between two (or more) people should be considered as being a two-way route for the transmission of STDs (i.e. "giving" or "receiving" are both risky).
Prevention of Sexually Transmitted Diseases
Although healthcare professionals suggest that safer sex, such as the use of condoms, as the most reliable way of decreasing the risk of contracting sexually transmitted diseases during sexual activity, safer sex should by no means be considered an absolute safeguard. The transfer of and exposure to bodily fluids, such as blood transfusions and other blood products, sharing injection needles, needle-stick injuries (when medical staff are inadvertently jabbed or pricked with needles during medical procedures), sharing tattoo needles, and childbirth are all avenues of transmission. These means put certain groups, such as doctors, haemophiliacs and drug users, particularly at risk.
Human Papillomavirus (HPV)
There are over 100 types of this virus which is often asymptomatic. Nearly 3 out of 4 Americans between ages 15 and 49 have been infected. It can be contracted through one partner and remain dormant allowing it to be transmitted to another. Some types can cause cervical cancer.
Genital HPV infection is a sexually transmitted disease that is caused by human papillomavirus. Human papillomavirus is the name of a group of viruses that includes more than 100 different strains. More than 30 of these are sexually transmitted and they can infect the genital area of men and women. Approximately 20 million people are currently infected with HPV and at least 50% of sexually active men and women will acquire HPV at some point in their lives. By age 50 at least 80% of women will have acquired HPV and about 6.2 million Americans get a new HPV infection each year. Most people who have HPV don't know that they are infected. The virus lives in the skin or mucous membranes and usually causes no symptoms. Commonly some people get visible genital warts or have pre-cancerous changes in the cervix, vulva, anus, or penis. Very rarely, HPV results in anal or genital cancers. Genital warts usually appear soft, moist, pink, or flesh colored swellings. They can be raised, flat, single, or multiple, small or large and sometimes cauliflower shaped. Warts may not appear for weeks or months or not at all and the only way to diagnose them is by visible inspection. Most women are diagnosed with HPV on the basis of abnormal pap tests and there are no tests available for men. There is no cure for HPV. The surest way to eliminate risk for HPV is to refrain from any genital contact with another individual. For those who choose to be sexually active, a long term monogamous relationship with an uninfected partner is the strategy most likely to prevent future HPV infections.The next best way to help reduce risk is using a condom but the effectiveness is unknown.
What is the connection between HPV and cervical cancer? All types of HPV cause mild pap test abnormalities which do not have serious consequences. Approximately 10 of the 30 identified HPV types can lead to development of cervical cancer. Research as shown that for most women, 90% cervical HPV infection becomes undetectable within two years. Although only a small proportion of women have persistent infection, persistent infection with the high risk types of HPV is the main risk factor for cervical cancer.
A pap test can detect pre-cancerous and cancerous cells on the cervix. Regular pap testing and careful medical follow up, with treatment if necessary, can help ensure that pre-cancerous changes in the cervix caused by HPV infection do not develop into life-threatening cervical cancer. The pap test used in the U.S. cervical cancer screening programs is responsible for greatly reducing deaths from cervical cancer.
Diseases and Disorders of the Female Reproductive System
Women are commonly dealing with many different diseases and disorders that pertain to the reproductive system. Here are some of the most common:
- Vulvovaginitis (pronounced:vul-vo-vah-juh-ni-tus) is an inflammation of the vulva and vagina. It may be caused by irritating substances such as laundry soap, bubble baths or poor hygiene such as wiping from back to front. Symptoms include redness and itching in these areas and sometimes vaginal discharge. It can also be caused by an overgrowth of candida, a fungus normally present in the vagina.
- Nonmenstrual vaginal bleeding is most commonly due to the presence of a foreign body in the vagina. It may also be due to urethral prolapse, a condition in which the mucous membranes of the urethra protrude into the vagina and forms a tiny, donut shaped mass of tissue that bleeds easily. It can also be due to a straddle injury or vaginal trauma from sexual abuse.
- Ectopic Pregnancy occurs when a fertilized egg or zygote doesn't travel into the uterus, but instead grows rapidly in the fallopian tube. Women with this condition can develop severe abdominal pain and should see a doctor because surgery may be necessary.
- Ovarian tumors,although rare, can occur. Women with ovarian tumors may have abdominal pain and masses that can be felt in the abdomen. Surgery may be needed to remove the tumor.
- Ovarian cysts are noncancerous sacs filled with fluid or semi-solid material. Although they are common and generally harmless, they can become a problem if they grow very large. Large cysts may push on surrounding organs, causing abdominal pain. In most cases, cysts will pass or disappear on their own and treatment is not necessary. If the cysts are painful and occur frequently, a doctor may prescribe birth control pills to alter their growth and occurrences. Surgery is also an option if they need to be removed.
- Polycystic ovary syndrome is a hormone disorder in which too many hormones are produced by the ovaries. This condition causes the ovaries to become enlarged and develop many fluid filled sacs or cysts. It often first appears during the teen years. Depending on the type and the severity of the condition, it may be treated with drugs to regulate hormone balance and menstruation.
- Trichomonas vaginalis inflammatory condition of the vagina usually a bacterial infection also called vaginosis.
- Dysmenorrhea is painful periods.
- Menorrhagia is when a woman has very heavy periods with excess bleeding.
- Oligomenorrhea is when a woman misses or has infrequent periods, even though she has been menstruating for a while and is not pregnant.
- Amenorrhea is when a girl has not started her period by the time she is 16 years old or 3 years after puberty has started, has not developed signs of puberty by 14, or has had normal periods but has stopped menstruating for some reasons other than pregnancy.
- Toxic shock syndrome is caused by toxins released into the body during a type of bacterial infection that is more likely to develop if a tampon is left in too long. It can produce high fever, diarrhea, vomiting, and shock.
- Candidasis symptoms of yeast infections include itching, burning and discharge. Yeast organisms are always present in all people, but are usually prevented from "overgrowth" (uncontrolled multiplication resulting in symptoms) by naturally occurring microorganisms.
At least three quarters of all women will experience candidiasis at some point in their lives. The Candida albicans organism is found in the vaginas of almost all women and normally causes no problems. However, when it gets out of balance with the other "normal flora," such as lactobacilli (which can also be harmed by using douches), an overgrowth of yeast can result in noticeable symptoms. Pregnancy, the use of oral contraceptives, engaging in vaginal sex after anal sex in an unhygienic manner, and using lubricants containing glycerin have been found to be causally related to yeast infections. Diabetes mellitus and the use of antibiotics are also linked to an increased incidence of yeast infections. Candidiasis can be sexually transmitted between partners. Diet has been found to be the cause in some animals. Hormone Replacement Therapy and Infertility Treatment may be factors.
There are also cancer's of the female reproductive system, such as:
- Cervical cancer
- Ovarian cancer
- Uterine cancer
- Breast cancer
Endometriosis
Endometriosis is the most common gynecological diseases, affecting more than 5.5 million women in North America alone! The two most common symptoms are pain and infertility. In this disease a specialized type of tissue that normally lines the inside of the uterus,(the endometrium) becomes implanted outside the uterus, most commonly on the fallopian tubes, ovaries, or the tissue lining the pelvis. During the menstrual cycle, hormones signal the lining of the uterus to thicken to prepare for possible pregnancy. If a pregnancy doesn't occur, the hormone levels decrease, causing the thickened lining to shed.
When endometrial tissue is located in other parts it continues to act in it's normal way: It thickens, breaks down and bleeds each month as the hormone levels rise and fall. However, because there's nowhere for the blood from this mislocated tissue to exit the body, it becomes trapped and surrounding tissue becomes irritated. Trapped blood may lead to growth of cysts. Cysts in turn may form scar tissue and adhesions. This causes pain in the area of the misplaced tissue, usually the pelvis. Endometriosis can cause fertility problems. In fact, scars and adhesions on the ovaries or fallopian tubes can prevent pregnancy. Endometriosis can be mild, moderate or severe and tends to get worse over time without treatment. The most common symptoms are:
- Painful periods Pelvic pain and severe cramping, intense back pain and abdominal pain.
- Pain at other times Women may experience pelvic pain during ovulation, sharp deep pain in pelvis during intercourse, or pain during bowel movements or urination.
- Excessive bleeding Heavy periods or bleeding between periods.
- Infertility Approximately 30-40% of women
The cause of endometriosis remains mysterious. Scientists are studying the roles that hormones and the immune system play in this condition. One theory holds that menstrual blood containing endometrial cells flows back through the fallopian tubes, takes root and grows. Another hypothesis proposes that the bloodstream carries endometrial cells to other sites in the body. Still another theory speculates that a predisposition toward endometriosis may be carried in the genes of certain families.
Other researchers believe that certain cells present within the abdomen in some women retain their ability to specialize into endometrial cells. These same cells were responsible for the growth of the woman's reproductive organs when she was an embryo. It is believed that genetic or environmental influences in later life allow these cells to give rise to endometrial tissue outside the uterus.
Experts estimate that up to one in ten American women of childbearing age have endometriosis. There is some thinking that previous damage to cells that line the pelvis can lead to endometriosis. There are several ways to diagnose endometriosis:
- Pelvic exam
- Ultrasound
- Laparoscopy Usually used, most correct diagnosis
- Blood test
Endometriosis can be treated with:
- Pain medication
- Hormone therapy
- Oral contraceptives
- Gonadotropin-releasing hormone(Gn-Rh)agonists and antagonists
- Danazol(Danocrine)
- Medroxyprogesterone(Depo-Provera)
- Conservative surgery which removes endometrial growths.
- Hysterectomy
Check Your Understanding
- Answers for these questions can be found here
1. In homology, the ___________ in the female is equal to the penis in the male
- A) labia majora
- B) clitoral hood
- C) clitoris
- D) labia minora
- E) none of the above
2. This contains some of the strongest muscles in the human body
- A) uterus
- B) clitoris
- C) cervix
- D) labia majora
3. This protects the vaginal and urethral openings
- A) labia majora
- B) labia minora
- C) clitoris
- D) urethra
4. Sally has noticed that her cervical mucus has changed and now resembles egg whites- from this Sally could assume
- A) her period will begin soon
- B) nothing, this is a normal occurrence
- C) she has a yeast infection
- D) she is ovulating
5. Debbie recently went to the OBGYN and was diagnosed with PCOD (polycystic ovary syndrome) because of this she has
- A) nothing, its normal in women
- B) antisperm antibodies
- C) an overproduction of LH
- D) leaking of milk from her mammary glands
- E) problems becoming pregnant
6. Angie went to the doctor because she has had pain in her leg recently- this could be caused by
- A) ovulation pain
- B) her period that will be starting tomorrow
- C) premenstrual syndrome
- D) a blood clot resulting from her birth control pill
7. Sue recently started her period and has noticed that they are very heavy and painful, and that they are inconsistent in their timing. One explanation could be
- A) endometriosis
- B) ovarian cancer
- C) candidiasis
- D) toxic shock syndrome
- E) amenorrhea
8. Mary is getting married and is not ready to become a mother- she chooses this birth control because of its high effectiveness
- A) natural family planning
- B) a diaphragm
- C) contraceptive injections
- D) a spermicide foam
9. The release of LH in woman causes
- A) menstration
- B) ovulation
- C) increase of endometrial lining
- D) decrease of endometrial lining
- E) nothing LH only does something in the male reproductive system
10. When the ovaries stop producing estrogen, this occurs
- A) ovulation
- B) implantation
- C) premenstrual syndrome
- D) menopause
11. Infertility affects what percentage of couples?
- A) 5%
- B) 10%
- C) 15%
- D) 20%
12. What is the only 100% effective form of birth control?
- A) Tubal ligation
- B) IUD
- C) Natural family planning
- D) Abstinence
Glossary
Adhesions: Abnormal tissue that binds organs together
Alveoli: Basic components of the mammary glands; lined with milk-secreting epithelial cells
Birth Control: regimen of one or more actions, devices, or medications followed in order to deliberately prevent or reduce the likelihood of a woman becoming pregnant
Cervical Mucus: Mucus secreted by the cervix, near ovulation it helps to lower the acidity of the vagina
Cervix: Lower, narrow portion of the uterus where it joins with the top of the vagina
Clitoris: Small body of spongy tissue that functions solely for sexual pleasure
Chromosomes: Structures in the nucleus that contain the genes for genetic expression
Ectocervix: Portion of the cervix projecting into vagina
Endocervical Canal: Passageway between the external os and the uterine cavity
Endometrium: The inner lining of the uterus
Fallopian Tubes: Located at the upper end of the vagina, passage way for the egg from the ovary
Factor V Leiden: This is the name given to a variant of human factor V that causes a hypercoagulability disorder. In this disorder the Leiden variant of factor V, cannot be inactivated by activated protein C. Factor V Leiden is the most common hereditary hypercoagulability disorder amongst Eurasians. It is named after the city Leiden (The Netherlands), where it was first identified in 1994 by Prof R. Bertina et al.
Gamete: A haploid sex cell; either an egg cell or a sperm cell
Gene: That portion of the DNA of a chromosome containing the information needed to synthesize a particular protein molecule
Gonad: A reproductive organ, testis or ovary that produces gametes and sex hormones
Hormone: A chemical substance produced in an endocrine gland and secreted into the bloodstream that acts on target cells to produce a specific effect
Hymen: Thin fold of mucous membrane that separates the lumen of the vagina from the urethral sinus
Infertility: Inability to naturally conceive a child or the inability to carry a pregnancy to term
Labia Majora: Outer "lips" of the vulva, made of loose connective tissue and adipose tissue with some smooth muscle
Labia Minora: Inner lips of the vulva, folds and protects the vagina, urethra and clitoris
Mammary Glands: Organs that produce milk for the sustenance of a baby
Meiosis: A specialized type of cell division by which gametes, or haploid sex cells, are formed
Menarche: The first menstrual discharge; occurs normally between the ages of 9 and 17
Menopause: The period marked by the cessation of menstrual periods in the human female
Menstrual Cycle: The rhythmic female reproductive cycle characterized by physical changes in the uterine lining
Menstruation: The discharge of blood and tissue from the uterus at the end of menstrual cycle
Mittelschmerz: Pain near the lower abdomen site at the time of ovulation; German for ovulation pain
Mons Veneris: soft mound at the front of the vulva (fatty tissue covering the pubic bone)
Ovarian Cycle: Last phase of the reproductive cycle; if no implantation occurs, causes the breakdown of the endometrial lining and causes menstruation
Ovulation: The rupture of an ovarian follicle with the release of an ovum
Perineum: External region between the scrotum and the anus in a male or between the vulva and anus in a female
Premenstrual Syndrome (PMS): Time leading up to menstruation; includes both physical and emotional symptoms: acne, bloating, fatigue, backaches, sore breasts, headaches, constipation, diarrhea, food cravings, depression, irritability, difficulty concentrating or handling stress
Puberty: The period of development in which the reproductive organs become functional and the secondary sex characteristics are expressed
Reproduction: Process by which an organism continues its species
Sexually transmitted diseases (STDs): diseases or infections that have a significant probability of transmission between humans by means of sexual contact
Urethra: Located below the clitoris, used for the passage of urine
Uterine Cycle: First part of the reproductive cycle; the time when the endrometrial lining builds up and follicles develop
Uterus: Major reproductive organ, receives fertilized eggs which become implanted in the lining, the lining (endometrium) provides nourishment to developing fetus; contains some of the strongest muscles in the female body and is able to stretch during fetus development
Vagina: Muscular, hollow tube that extends from the vaginal opening to the cervix
Vulva: External female genitals, includes labia majora, labia minora, mons pubis, clitoris, meatus, vaginal vestibule, vestibule bulbs and vestibular glands
References
- Essentials of Anatomy and Physiology. Fourth Edition. Valerie C. Scanlon and Tina Sanders.
- Human Anatomy. Sixth Edition. Van De Graaff.
- Wikibook: Sexual Health
- http://www.fda.gov/cder/drug/infopage/planBQandAhtm
- http://www.goplanb.com/Forconsumers
- American Social Health Association;ashastd.org
- http://www.cdc.gov
- http://www.mayoclinic.com