Human Physiology/The Urinary System
Homeostasis — Cells — Integumentary — Nervous — Senses — Muscular — Blood — Cardiovascular — Immune — Urinary — Respiratory — Gastrointestinal — Nutrition — Endocrine — Reproduction (male) — Reproduction (female) — Pregnancy — Genetics — Development — Answers

Introduction
The Urinary System is a group of organs in the body concerned with filtering out excess fluid and other substances from the bloodstream. The substances are filtered out from the body in the form of urine. Urine is a liquid produced by the kidneys, collected in the bladder and excreted through the urethra. Urine is used to extract excess minerals or vitamins as well as blood corpuscles from the body. The Urinary organs include the kidneys, ureters, bladder, and urethra. The Urinary system works with the other systems of the body to help maintain homeostasis. The kidneys are the main organs of homeostasis because they maintain the acid base balance and the water salt balance of the blood.
Functions of the Urinary System
One of the major functions of the Urinary system is the process of excretion. Excretion is the process of eliminating, from an organism, waste products of metabolism and other materials that are of no use. The urinary system maintains an appropriate fluid volume by regulating the amount of water that is excreted in the urine. Other aspects of its function include regulating the concentrations of various electrolytes in the body fluids and maintaining normal pH of the blood. Several body organs carry out excretion, but the kidneys are the most important excretory organ. The primary function of the kidneys is to maintain a stable internal environment (homeostasis) for optimal cell and tissue metabolism. They do this by separating urea, mineral salts, toxins, and other waste products from the blood. They also do the job of conserving water, salts, and electrolytes. At least one kidney must function properly for life to be maintained. Six important roles of the kidneys are:
Regulation of plasma ionic composition. Ions such as sodium, potassium, calcium, magnesium, chloride, bicarbonate, and phosphates are regulated by the amount that the kidney excretes.
Regulation of plasma osmolarity. The kidneys regulate osmolarity because they have direct control over how many ions and how much water a person excretes.
Regulation of plasma volume. Your kidneys are so important they even have an effect on your blood pressure. The kidneys control plasma volume by controlling how much water a person excretes. The plasma volume has a direct effect on the total blood volume, which has a direct effect on your blood pressure. Salt(NaCl)will cause osmosis to happen; the diffusion of water into the blood.
Regulation of plasma hydrogen ion concentration (pH). The kidneys partner up with the lungs and they together control the pH. The kidneys have a major role because they control the amount of bicarbonate excreted or held onto. The kidneys help maintain the blood Ph mainly by excreting hydrogen ions and reabsorbing bicarbonate ions as needed.
Removal of metabolic waste products and foreign substances from the plasma. One of the most important things the kidneys excrete is nitrogenous waste. As the liver breaks down amino acids it also releases ammonia. The liver then quickly combines that ammonia with carbon dioxide, creating urea which is the primary nitrogenous end product of metabolism in humans. The liver turns the ammonia into urea because it is much less toxic. We can also excrete some ammonia, creatinine and uric acid. The creatinine comes from the metabolic breakdown of creatine phospate (a high-energy phosphate in muscles). Uric acid comes from the break down of nucleotides. Uric acid is insoluble and too much uric acid in the blood will build up and form crystals that can collect in the joints and cause gout.
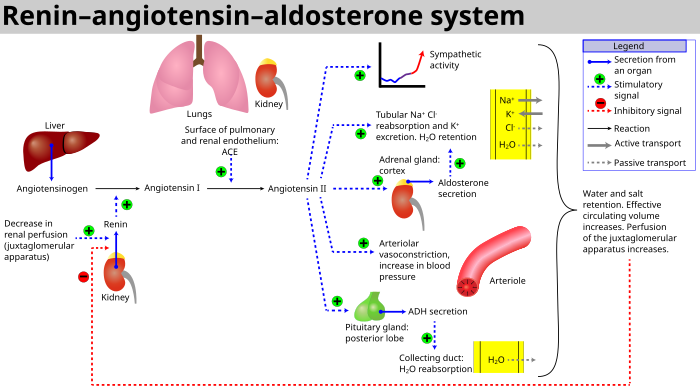
Secretion of Hormones The endocrine system has assistance from the kidney's when releasing hormones. Renin is released by the kidneys. Renin leads to the secretion of aldosterone which is released from the adrenal cortex. Aldosterone promotes the kidneys to reabsorb the sodium (Na+) ions. The kidneys also secrete erythropoietin when the blood doesn't have the capacity to carry oxygen. Erythropoietin stimulates red blood cell production. The Vitamin D from the skin is also activated with help from the kidneys. Calcium (Ca+) absorption from the digestive tract is promoted by vitamin D.
CC: Chapter Check: Name the role of the kidneys and how they work?
Organs in the Urinary System
Kidneys And Their Structure

The kidneys are a pair of bean shaped, brown organs about the size of your fist.It measures 10-12 cm long. They are covered by the renal capsule, which is a tough capsule of fibrous connective tissue. Adhering to the surface of each kidney is two layers of fat to help cushion them. There is a concaved side of the kidney that has a depression where a renal artery enters, and a renal vein and a ureter exit the kidney. The kidneys are located at the rear wall of the abdominal cavity just above the waistline, and are protected by the ribcage. They are considered retroperitoneal, which means they lie behind the peritoneum. There are three major regions of the kidney, renal cortex, renal medulla and the renal pelvis. The outer, granulated layer is the renal cortex. The cortex stretches down in between a radially striated inner layer. The inner radially striated layer is the renal medulla. This contains pyramid shaped tissue called the renal pyramids, separated by renal columns. The ureters are continuous with the renal pelvis and is the very center of the kidney.
Renal Vein
The renal veins are veins that drain the kidney. They connect the kidney to the inferior vena cava. Because the inferior vena cava is on the right half of the body, the left renal vein is generally the longer of the two. Unlike the right renal vein, the left renal vein often receives the left gonadal vein (left testicular vein in males, left ovarian vein in females). It frequently receives the left suprarenal vein as well.
Renal Artery
The renal arteries normally arise off the abdominal aorta and supply the kidneys with blood. The arterial supply of the kidneys are variable and there may be one or more renal arteries supplying each kidney. Due to the position of the aorta, the inferior vena cava and the kidneys in the body, the right renal artery is normally longer than the left renal artery. The right renal artery normally crosses posteriorly to the inferior vena cava. The renal arteries carry a large portion of the total blood flow to the kidneys. Up to a third of the total cardiac output can pass through the renal arteries to be filtered by the kidneys.
Ureters
The ureters are two tubes that drain urine from the kidneys to the bladder. Each ureter is a muscular tube about 10 inches (25 cm) long. Muscles in the walls of the ureters send the urine in small spurts into the bladder, (a collapsible sac found on the forward part of the cavity of the bony pelvis that allows temporary storage of urine). After the urine enters the bladder from the ureters, small folds in the bladder mucosa act like valves preventing backward flow of the urine. The outlet of the bladder is controlled by a sphincter muscle. A full bladder stimulates sensory nerves in the bladder wall that relax the sphincter and allow release of the urine. However, relaxation of the sphincter is also in part a learned response under voluntary control. The released urine enters the urethra.
Urinary Bladder
The urinary bladder is a hollow, muscular and distendible or elastic organ that sits on the pelvic floor (superior to the prostate in males). On its anterior border lies the pubic symphysis and, on its posterior border, the vagina (in females) and rectum (in males). The urinary bladder can hold approximately 17 to 18 ounces (500 to 530 ml) of urine, however the desire to micturate is usually experienced when it contains about 150 to 200 ml. When the bladder fills with urine (about half full), stretch receptors send nerve impulses to the spinal cord, which then sends a reflex nerve impulse back to the sphincter (muscular valve) at the neck of the bladder, causing it to relax and allow the flow of urine into the urethra. The Internal urethral sphincter is involuntary. The ureters enter the bladder diagonally from its dorsolateral floor in an area called the trigone. The trigone is a triangular shaped area on the postero-inferior wall of the bladder. The urethra exits at the lowest point of the triangle of the trigone. The urine in the bladder also helps regulate body temperature. A bladder when operating normally empties completely upon a complete discharge, otherwise it is a sign that its elasticity is compromised, when it becomes completely void of fluid, it may cause a chilling sensation due to the rapid change of body temperature.
Urethra

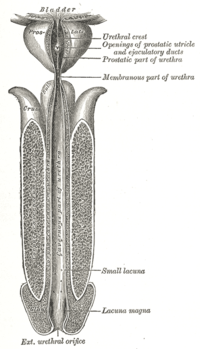
The urethra is a muscular tube that connects the bladder with the outside of the body. The function of the urethra is to remove urine from the body. It measures about 1.5 inches (3.8 cm) in a woman but up to 8 inches (20 cm) in a man. Because the urethra is so much shorter in a woman it makes it much easier for a woman to get harmful bacteria in her bladder this is commonly called a bladder infection or a UTI. The most common bacteria of a UTI is E-coli from the large intestines that have been excreted in fecal matter. Female urethra
In the human female, the urethra is about 1-2 inches long and opens in the vulva between the clitoris and the vaginal opening.
Men have a longer urethra than women. This means that women tend to be more susceptible to infections of the bladder (cystitis) and the urinary tract.
Male urethra
In the human male, the urethra is about 8 inches long and opens at the end of the head of the penis.
The length of a male's urethra, and the fact it contains a number of bends, makes catheterisation more difficult.
The urethral sphincter is a collective name for the muscles used to control the flow of urine from the urinary bladder. These muscles surround the urethra, so that when they contract, the urethra is closed.
- There are two distinct areas of muscle: the internal sphincter, at the bladder neck and
- the external, or distal, sphincter.
Human males have much stronger sphincter muscles than females, meaning that they can retain a large amount of urine for twice as long, as much as 800mL, i.e. "hold it".
Nephrons
A nephron is the basic structural and functional unit of the kidney. The name nephron comes from the Greek word (nephros) meaning kidney. Its chief function is to regulate water and soluble substances by filtering the blood, reabsorbing what is needed and excreting the rest as urine. Nephrons eliminate wastes from the body, regulate blood volume and pressure, control levels of electrolytes and metabolites, and regulate blood pH. Its functions are vital to life and are regulated by the endocrine system by hormones such as antidiuretic hormone, aldosterone, and parathyroid hormone.
Each nephron has its own supply of blood from two capillary regions from the renal artery. Each nephron is composed of an initial filtering component (the renal corpuscle) and a tubule specialized for reabsorption and secretion (the renal tubule). The renal corpuscle filters out large solutes from the blood, delivering water and small solutes to the renal tubule for modification.
Glomerulus
The glomerulus is a capillary tuft that receives its blood supply from an afferent arteriole of the renal circulation. The glomerular blood pressure provides the driving force for fluid and solutes to be filtered out of the blood and into the space made by Bowman's capsule. The remainder of the blood not filtered into the glomerulus passes into the narrower efferent arteriole. It then moves into the vasa recta, which are collecting capillaries intertwined with the convoluted tubules through the interstitial space, where the reabsorbed substances will also enter. This then combines with efferent venules from other nephrons into the renal vein, and rejoins with the main bloodstream.
Afferent/Efferent Arterioles
The afferent arteriole supplies blood to the glomerulus. A group of specialized cells known as juxtaglomerular cells are located around the afferent arteriole where it enters the renal corpuscle. The efferent arteriole drains the glomerulus. Between the two arterioles lies specialized cells called the macula densa. The juxtaglomerular cells and the macula densa collectively form the juxtaglomerular apparatus. It is in the juxtaglomerular apparatus cells that the enzyme renin is formed and stored. Renin is released in response to decreased blood pressure in the afferent arterioles, decreased sodium chloride in the distal convoluted tubule and sympathetic nerve stimulation of receptors (beta-adrenic) on the juxtaglomerular cells. Renin is needed to form Angiotensin I and Angiotensin II which stimulate the secretion of aldosterone by the adrenal cortex.
Glomerular Capsule or Bowman's Capsule
Bowman's capsule (also called the glomerular capsule) surrounds the glomerulus and is composed of visceral (simple squamous epithelial cells) (inner) and parietal (simple squamous epithelial cells) (outer) layers. The visceral layer lies just beneath the thickened glomerular basement membrane and is made of podocytes which send foot processes over the length of the glomerulus. Foot processes interdigitate with one another forming filtration slits that, in contrast to those in the glomeruluar endothelium, are spanned by diaphragms. The size of the filtration slits restricts the passage of large molecules (e.g., albumin) and cells (e.g., red blood cells and platelets). In addition, foot processes have a negatively-charged coat (glycocalyx) that limits the filtration of negatively-charged molecules, such as albumin. This action is called electrostatic repulsion.
The parietal layer of Bowman's capsule is lined by a single layer of squamous epithelium. Between the visceral and parietal layers is Bowman's space, into which the filtrate enters after passing through the podocytes' filtration slits. It is here that smooth muscle cells and macrophages lie between the capillaries and provide support for them. Unlike the visceral layer, the parietal layer does not function in filtration. Rather, the filtration barrier is formed by three components: the diaphragms of the filtration slits, the thick glomerular basement membrane, and the glycocalyx secreted by podocytes. 99% of glomerular filtrate will ultimately be reabsorbed.
The process of filtration of the blood in the Bowman's capsule is ultrafiltration (or glomerular filtration), and the normal rate of filtration is 125 ml/min, equivalent to ten times the blood volume daily. Measuring the glomerular filtration rate (GFR) is a diagnostic test of kidney function. A decreased GFR may be a sign of renal failure. Conditions that can affect GFR include: arterial pressure, afferent arteriole constriction, efferent arteriole constriction, plasma protein concentration and colloid osmotic pressure.
Any proteins that are roughly 30 kilodaltons or under can pass freely through the membrane. Although, there is some extra hindrance for negatively charged molecules due to the negative charge of the basement membrane and the podocytes. Any small molecules such as water, glucose, salt (NaCl), amino acids, and urea pass freely into Bowman's space, but cells, platelets and large proteins do not. As a result, the filtrate leaving the Bowman's capsule is very similar to blood plasma in composition as it passes into the proximal convoluted tubule. Together, the glomerulus and Bowman's capsule are called the renal corpuscle.
Proximal Convoluted Tubule (PCT)
The proximal tubule can be anatomically divided into two segments: the proximal convoluted tubule and the proximal straight tubule. The proximal convoluted tubule can be divided further into S1 and S2 segments based on the histological appearance of it's cells. Following this naming convention, the proximal straight tubule is commonly called the S3 segment. The proximal convoluted tubule has one layer of cuboidal cells in the lumen. This is the only place in the nephron that contains cuboidal cells. These cells are covered with millions of microvilli. The microvilli serve to increase surface area for reabsorption.
Fluid in the filtrate entering the proximal convoluted tubule is reabsorbed into the peritubular capillaries, including approximately two-thirds of the filtered salt and water and all filtered organic solutes (primarily glucose and amino acids). This is driven by sodium transport from the lumen into the blood by the Na+/K+ ATPase in the basolateral membrane of the epithelial cells. Much of the mass movement of water and solutes occurs in between the cells through the tight junctions, which in this case are not selective.
The solutes are absorbed isotonically, in that the osmotic potential of the fluid leaving the proximal tubule is the same as that of the initial glomerular filtrate. However, glucose, amino acids, inorganic phosphate, and some other solutes are reabsorbed via secondary active transport through cotransport channels driven by the sodium gradient out of the nephron.
Loop of the Nephron or Loop of Henle
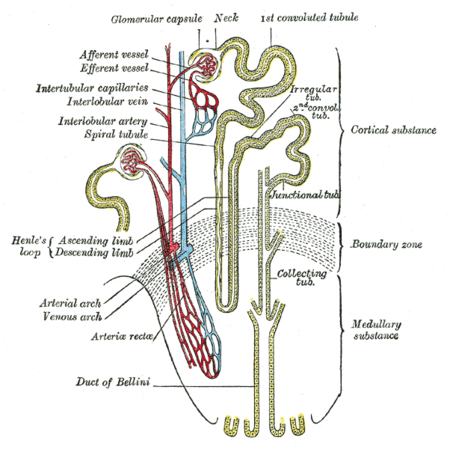
The loop of Henle (sometimes known as the nephron loop) is a U-shaped tube that consists of a descending limb and ascending limb. It begins in the cortex, receiving filtrate from the proximal convoluted tubule, extends into the medulla, and then returns to the cortex to empty into the distal convoluted tubule. Its primary role is to concentrate the salt in the interstitium, the tissue surrounding the loop.
- Descending limb
- Its descending limb is permeable to water but completely impermeable to salt, and thus only indirectly contributes to the concentration of the interstitium. As the filtrate descends deeper into the hypertonic interstitium of the renal medulla, water flows freely out of the descending limb by osmosis until the tonicity of the filtrate and interstitium equilibrate. Longer descending limbs allow more time for water to flow out of the filtrate, so longer limbs make the filtrate more hypertonic than shorter limbs.
- Ascending limb
- Unlike the descending limb, the ascending limb of Henle's loop is impermeable to water, a critical feature of the countercurrent exchange mechanism employed by the loop. The ascending limb actively pumps sodium out of the filtrate, generating the hypertonic interstitium that drives countercurrent exchange. In passing through the ascending limb, the filtrate grows hypotonic since it has lost much of its sodium content. This hypotonic filtrate is passed to the distal convoluted tubule in the renal cortex.
Distal Convoluted Tubule (DCT)
The distal convoluted tubule is similar to the proximal convoluted tubule in structure and function. Cells lining the tubule have numerous mitochondria, enabling active transport to take place by the energy supplied by ATP. Much of the ion transport taking place in the distal convoluted tubule is regulated by the endocrine system. In the presence of parathyroid hormone, the distal convoluted tubule reabsorbs more calcium and excretes more phosphate. When aldosterone is present, more sodium is reabsorbed and more potassium excreted. Atrial natriuretic peptide causes the distal convoluted tubule to excrete more sodium. In addition, the tubule also secretes hydrogen and ammonium to regulate pH. After traveling the length of the distal convoluted tubule, only 3% of water remains, and the remaining salt content is negligible. 97.9% of the water in the glomerular filtrate enters the convoluted tubules and collecting ducts by osmosis.
Collecting ducts
Each distal convoluted tubule delivers its filtrate to a system of collecting ducts, the first segment of which is the connecting tubule. The collecting duct system begins in the renal cortex and extends deep into the medulla. As the urine travels down the collecting duct system, it passes by the medullary interstitium which has a high sodium concentration as a result of the loop of Henle's countercurrent multiplier system. Though the collecting duct is normally impermeable to water, it becomes permeable in the presence of antidiuretic hormone (ADH). As much as three-fourths of the water from urine can be reabsorbed as it leaves the collecting duct by osmosis. Thus the levels of ADH determine whether urine will be concentrated or dilute. Dehydration results in an increase in ADH, while water sufficiency results in low ADH allowing for diluted urine. Lower portions of the collecting duct are also permeable to urea, allowing some of it to enter the medulla of the kidney, thus maintaining its high ion concentration (which is very important for the nephron).
Urine leaves the medullary collecting ducts through the renal papilla, emptying into the renal calyces, the renal pelvis, and finally into the bladder via the ureter. Because it has a different embryonic origin than the rest of the nephron (the collecting duct is from endoderm whereas the nephron is from mesoderm), the collecting duct is usually not considered a part of the nephron proper.
Renal Hormones
1. Vitamin D- Becomes metabolically active in the kidney. Patients with renal disease have symptoms of disturbed calcium and phosphate balance.
2. Erythropoietin- Released by the kidneys in response to decreased tissue oxygen levels (hypoxia).
3. Natriuretic Hormone- Released from cardiocyte granules located in the right atria of the heart in response to increased atrial stretch. It inhibits ADH secretions which can contribute to the loss of sodium and water.
Formation of Urine
Urine is formed in three steps: Filtration, Reabsorption, and Secretion.
Filtration
Blood enters the afferent arteriole and flows into the glomerulus. Blood in the glomerulus has both filterable blood components and non-filterable blood components. Filterable blood components move toward the inside of the glomerulus while non-filterable blood components bypass the filtration process by exiting through the efferent arteriole. Filterable Blood components will then take a plasma like form called glomerular filtrate. A few of the filterable blood components are water, nitrogenous waste, nutrients and salts (ions). Nonfilterable blood components include formed elements such as blood cells and platelets along with plasma proteins. The glomerular filtrate is not the same consistency as urine, as much of it is reabsorbed into the blood as the filtrate passes through the tubules of the nephron.
Reabsorption
Within the peritubular capillary network, molecules and ions are reabsorbed back into the blood. Sodium Chloride reabsorbed into the system increases the osmolarity of blood in comparison to the glomerular filtrate. This reabsorption process allows water (H2O) to pass from the glomerular filtrate back into the circulatory system.
Glucose and various amino acids also are reabsorbed into the circulatory system. These nutrients have carrier molecules that claim the glomerular molecule and release it back into the circulatory system. If all of the carrier molecules are used up, excess glucose or amino acids are set free into the urine. A complication of diabetes is the inability of the body to reabsorb glucose. If too much glucose appears in the glomerular filtrate it increases the osmolarity of the filtrate, causing water to be released into the urine rather than reabsorbed by the circulatory system. Frequent urination and unexplained thirst are warning signs of diabetes, due to water not being reabsorbed.
Glomerular filtrate has now been separated into two forms: Reabsorbed Filtrate and Non-reabsorbed Filtrate. Non-reabsorbed filtrate is now known as tubular fluid as it passes through the collecting duct to be processed into urine.
Secretion
Some substances are removed from blood through the peritubular capillary network into the distal convoluted tubule or collecting duct. These substances are Hydrogen ions, creatinine, and drugs. Urine is a collection of substances that have not been reabsorbed during glomerular filtration or tubular reabsorbtion.
Maintaining Water-Salt Balance
It is the job of the kidneys to maintain the water-salt balance of the blood. They also maintain blood volume as well as blood pressure. Simple examples of ways that this balance can be changed include ingestion of water, dehydration, blood loss and salt ingestion.
Reabsorption of water
Direct control of water excretion in the kidneys is exercised by the anti-diuretic hormone (ADH), released by the posterior lobe of the pituitary gland. ADH causes the insertion of water channels into the membranes of cells lining the collecting ducts, allowing water reabsorption to occur. Without ADH, little water is reabsorbed in the collecting ducts and dilute urine is excreted. There are several factors that influence the secretion of ADH. The first of these happen when the blood plasma gets too concentrated. When this occurs, special receptors in the hypothalamus release ADH. When blood pressure falls, stretch receptors in the aorta and carotid arteries stimulate ADH secretion to increase volume of the blood.
Reabsorption of Salt
The Kidneys also regulate the salt balance in the blood by controlling the excretion and the reabsorption of various ions. As noted above, ADH plays a role in increasing water reabsorption in the kidneys, thus helping to dilute bodily fluids. The kidneys also have a regulated mechanism for reabsorbing sodium in the distal nephron. This mechanism is controlled by aldosterone, a steroid hormone produced by the adrenal cortex. Aldosterone promotes the excretion of potassium ions and the reabsorption of sodium ions. The release of Aldosterone is initiated by the kidneys. The juxtaglomerular apparatus is a renal structure consisting of the macula densa, mesangial cells, and juxtaglomerular cells. Juxtaglomerular cells (JG cells, also known as granular cells) are the site of renin secretion. Renin is an enzyme that converts angiotensinogen (a large plasma protein produced by the liver) into Angiotensin I and eventually into Angiotensin II which stimulates the adrenal cortex to produce aldosterone. The reabsorption of sodium ions is followed by the reapsorption of water. This causes blood pressure as well as blood volume to increase.
Atrial natriuretic hormone (ANH) is released by the atria of the heart when cardiac cells are stretched due to increased blood volume. ANH inhibits the secretion of renin by the juxtaglomerular apparatus and the secretion of the aldosterone by the adrenal cortex. This promotes the excretion of sodium. When sodium is excreted so is water. This causes blood pressure and volume to decrease.
Hypernatremia
An increase in plasma sodium levels above normal is hypernatremia. Sodium is the primary solute in the extracellular fluid. Sodium levels have a major role in osmolarity regulation. For excitable cells the electrochemical gradient for sodium across the plasma membrane is critical for life. Water retention and an increased blood pressure usually are signs of hypernatremia. If the plasma sodium levels are below normal it is called hyponatremia. Signs of this are low plasma volume and hypotension.
Diuretics
A diuretic (colloquially called a water pill) is any drug that elevates the rate of bodily urine excretion (diuresis). Diuretics also decrease the extracellular fluid (ECF) volume, and are primarily used to produce a negative extracellular fluid balance. Caffeine, cranberry juice and alcohol are all weak diuretics. In medicine, diuretics are used to treat heart failure, liver cirrhosis, hypertension and certain kidney diseases. Diuretics alleviate the symptoms of these diseases by causing sodium and water loss through the urine. As urine is produced by the kidney, sodium and water – which cause edema related to the disease – move into the blood to replace the volume lost as urine, thereby reducing the pathological edema. Some diuretics, such as acetazolamide, help to make the urine more alkaline and are helpful in increasing excretion of substances such as aspirin in cases of overdose or poisoning. The antihypertensive actions of some diuretics (thiazides and loop diuretics in particular) are independent of their diuretic effect. That is, the reduction in blood pressure is not due to decreased blood volume resulting from increased urine production, but occurs through other mechanisms and at lower doses than that required to produce diuresis. Indapamide was specifically designed with this is mind, and has a larger therapeutic window for hypertension (without pronounced diuresis) than most other diuretics. Chemically, diuretics are a diverse group of compounds that either stimulate or inhibit various hormones that naturally occur in the body to regulate urine production by the kidneys. Alcohol produces diuresis through modulation of the vasopressin system.
Diseases of the Kidney
Diabetic nephropathy (nephropatia diabetica), also known as Kimmelstiel-Wilson syndrome and intercapillary glomerulonephritis, is a progressive kidney disease caused by angiopathy of capillaries in the kidney glomeruli. It is characterized by nodular glomerulosclerosis. It is due to longstanding diabetes mellitus, and is a prime cause for dialysis in many Western countries.

In medicine, hematuria (or "haematuria") is the presence of blood in the urine. It is a sign of a large number of diseases of the kidneys and the urinary tract, ranging from trivial to lethal.
Kidney stones, also known as nephrolithiases, urolithiases or renal calculi, are solid accretions (crystals) of dissolved minerals in urine found inside the kidneys or ureters. They vary in size from as small as a grain of sand to as large as a golf ball. Kidney stones typically leave the body in the urine stream; if they grow relatively large before passing (on the order of millimeters), obstruction of a ureter and distention with urine can cause severe pain most commonly felt in the flank, lower abdomen and groin. Kidney stones are unrelated to gallstones.
Case Study I was 34 weeks pregnant when I noticed blood in my urine. I immediately went to my OBGYN where I was told that I had a bladder infection and given an antibiotic. The next morning I experienced the most intense pain. I was rushed to the ER where I was told that I had kidney stones. The doctors explained that there was nothing they could do as long as I was pregnant. The next 3 weeks of my life were filled with intense pain and multiple painkillers. After I delivered my baby, CAT scans were done and I was informed that I had 6 kidney stones. It took three more weeks for me to pass all of the stones the largest measuring 5 mm. The stones were tested and I was informed that my body had been building up calcium due to my pregnancy and this was the cause of the kidney stones. I continued to have kidney pain for 6 months after passing the stones. I now live my life on a low calcium diet and the hope that my body will not develop more kidney stones.
Pyelonephritis When an infection of the renal pelvis and calices, called pyelitis, spreads to involve the rest of the kidney as well, the result is pyelonephritis. It usually results from the spread of fecal bacterium Escherichia coli from the anal region superiorly through the urinary tract. In severe cases, the kidney swells and scars, abscesses form, and the renal pelvis fills with pus. Left untreated, the infected kidney may be severely damaged, but administration of antibiotics usually achieve a total cure.
glomerulonephritis Inflammation of the glomerular can be caused by immunologic abnormalities, drugs or toxins, vascular disorders, and systemic diseases. Glomerulonephritis can be acute, chronic or progressive. Two major changes in the urine are distinctive of glomerulonephritis: hematuria and proteinuria with albumin as the major protein. There is also a decrease in urine as there is a decrease in GFR (glomerular filtration rate). Renal failure is associated with oliguria (less than 400 ml of urine output per day).
Renal Failure Uremia is a syndrome of renal failure and includes elevated blood urea and creatinine levels. Acute renal failure can be reversed if diagnosed early. Acute renal failure can be caused by severe hypotension or severe glomerular disease. Diagnostic tests include BUN and plasma creatinine level tests. It is considered to be chronic renal failure if the decline of renal function to less than 25%.
Diabetes Insipidus
This is caused by the deficiency of or decrease of ADH. The person with (DI) has the inability to concentrate their urine in water restriction, in turn they will void up 3 to 20 liters/day. There are two forms of (DI), neurogenic, and nephrogenic. In nephrogenic (DI) the kidneys do not respond to ADH. Usually the nephrogenic (DI) is characterized by the impairment of the urine concentrating capability of the kidney along with concentration of water. The cause may be a genetic trait, electrolyte disorder, or side effect of drugs such as lithium. In the neurogenic (DI), it is usually caused by head injury near the hypophysisal tract.
Urinary tract infections (UTI's)
The second most common type of bacterial infections seen by health care providers is UTI's. Out of all the bacterias that colonize and cause urinary tract infections the big gun is Escherichia coli. In the hospital indwelling catheters and straight catheterizing predispose the opportunity for urinary tract infections. In females there are three stages in life that predispose urinary tract infections, that is menarche, manipulation between intercourse, and menopause. However, a small percentage of men and children will get urinary tract infections. In men it is usually due to the prostate gland growth which usually occurs in older age men. In children it can occur 3% to 5% in girls and 1% in boys, uncircumcised boys it is more common than circumcised ones to have a urinary tract infection, in girls it may be the result of onset of toilet training, some predispositions for getting urinary tract infection include family history and urinary tract anomalies. In neonates urinary tract infections is most common when bacteremia is present.
Dialysis and Kidney Transplant

Generally, humans can live normally with just one kidney. Only when the amount of functioning kidney tissue is greatly diminished will renal failure develop. If renal function is impaired, various forms of medications are used, while others are contraindicated. Provided that treatment is begun early, it may be possible to reverse chronic kidney failure due to diabetes or high blood pressure. If creatinine clearance (a measure of renal function) has fallen very low ("end-stage renal failure"), or if the renal dysfunction leads to severe symptoms, dialysis is commenced. Dialysis is a medical procedure, performed in various different forms, where the blood is filtered outside of the body.
Kidney transplantation is the only cure for end stage renal failure; dialysis, is a supportive treatment; a form of "buying time" to bridge the inevitable wait for a suitable organ.
The first successful kidney transplant was announced on March 4, 1954 at Peter Bent Brigham Hospital in Boston. The surgery was performed by Dr. Joseph E. Murray, who was awarded the Nobel Prize in Medicine in 1990 for this feat.
There are two types of kidney transplants: living donor transplant and a cadaveric (dead donor) transplant. When a kidney from a living donor, usually a blood relative, is transplanted into the patient's body, the donor's blood group and tissue type must be judged compatible with the patient's, and extensive medical tests are done to determine the health of the donor. Before a cadaveric donor's organs can be transplanted, a series of medical tests have to be done to determine if the organs are healthy. Also, in some countries, the family of the donor must give its consent for the organ donation. In both cases, the recipient of the new organ needs to take drugs to suppress their immune system to help prevent their body from rejecting the new kidney.
Review Questions
- Answers for these questions can be found here
1. While reading a blood test I notice a high level of creatinine, I could assume from this that
- A) There is a possibility of a UTI
- B) There is a possibility of diabetes
- C) There is a possibility of kidney failure
- D) There is nothing wrong, this is normal
2. Direct control of water excretion in the kidneys is controlled by
- A) Anti-diuretic hormone
- B) The medulla oblongata
- C) Blood plasma
- D) Sodium amounts in the blood
3. Nephrons
- A) Eliminate wastes from the body
- B) Regulate blood volume and pressure
- C) Control levels of electrolytes and metabolites
- D) Regulate blood pH
- E) All of the above
4. If I am dehydrated, my body will increase
- A) ATP
- B) ADP
- C) Diluted urine
- D) ADH
5. Which part of the nephron removes water, ions and nutrients from the blood?
- A ) vasa recta
- B ) loop of henle
- C ) proximal convoluted tubule
- D ) peritubular capillaries
- E ) glomerulus
6. Kidneys have a direct effect on which of the following
- A ) Blood pressure
- B ) How much water a person excretes
- C ) Total blood volume
- D ) pH
- E ) all of the above
7. Why do substances in the glomerulus enter the Bowman's capsule?
- A ) the magnetic charge of the Bowman's capsule attracts the substances
- B ) the substances are actively transported into the Bowman's capsule
- C ) blood pressure of the glomerulus is so great that most substances in blood move into capsule
- D ) little green men force it in with their ray guns
8. What happens in tubular excretion?
- A ) urine bonds are formed between the wastes
- B ) wastes are diffused from the tubule
- C ) wastes move into the distal convoluted tubule from the blood
- D ) blood pressure forces wastes away from the kidney
9. The countercurrent exchange system includes_________and_________.
- A ) glomerulus and macula densa
- B ) proximal convoluted tubule and distal convoluted tubule
- C ) loop of Henle and collecting tubule
- D ) afferent arteriole and efferent arteriole
- E ) ureters and bladder
10. The function of the loop of the nephron in the process of urine formation is:
- A ) reabsorption of water
- B ) production of filtrate
- C ) reabsorption of solutes
- D ) secretion of solutes
11. Name the six important roles of the kidneys.
Glossary
Antidiuretic: lessening or decreasing of urine production or an agent that decreases the release of urine.
Catheterisation: a catheter is a tube that can be inserted into a body cavity, duct or vessel. Catheters thereby allow drainage or injection of fluids or access by surgical instruments. The process of inserting a catheter is catheterisation. In most uses a catheter is a thin, flexible tube: a "soft" catheter; in some uses, it is a larger, solid tube: a "hard" catheter.
Dehydration: condition resulting from excessive loss of body fluid.
Diabetes: a general term for a disease characterized by the beginning stages and onset of renal failure. It is derived from the Greek word diabaínein, that literally means "passing through," or "siphon", a reference to one of diabetes' major symptoms—excessive urine production.
Diuresis: secretion and passage of large amounts of urine.
Diuretic: increasing of urine production, or an agent that increases the production of urine.
Erythropoietin: hormone that stimulates stem cells in the bone marrow to produce red blood cells
Fibrous Capsule: the kidney's loose connective tissue
Glomerulus: capillary tuft that receives its blood supply from an afferent arteriole of the renal circulation.
Gluconeogenesis: the cycle of producing a glucose form fat or protein; preformed by the kidney in times of long fasting, initially gluconeogenesis is preformed by the liver
Juxtaglomerular (JG) cells: Renin-secreting cells that are in contact with the macula densa and the afferent arterioles of the renal nephron.
Juxtaglomerular apparatus (JGA): A site of juxtaglomerular cells connecting with the macula densa where renin is secreted and sensor for control of secretion of golmerular filtration rate.
Loop of Henle/ Nephron Loop: u-shaped tube that consists of a descending limb and ascending limb; primary role is to concentrate the salt in the interstitium, the tissue surrounding the loop
Medullary Pyramids or Renal Pyramids: the cone shaped masses in the kidney
Micturition: another name for excretions
Nephron: basic structural and functional unit of the kidney; chief function is to regulate water and soluble substances by filtering the blood, reabsorbing what is needed and excreting the rest as urine
Podocytes: filtration membrane, in the visceral layer of the bowman's capsule
Renal Calculi: kidney stones, solid crystals of dissolved minerals in urine found inside the kidneys
Renal Cortex: outer portion of the kidney
Renal Lobe: each pyramid together with the associated overlying cortex
Renal Pelvis: a central space, or cavity that transmits urine to the urinary bladder via the ureter
Renin: hormone released by the Juxtaglomerular (JG) cells of the kidneys when blood pressure falls
TURP: transurethral resection of the prostate. During TURP, an instrument is inserted up the urethra to remove the section of the prostate that is blocking urine flow. This is most commonly caused by benign prostatic hyperplasia (BPH). A TURP usually requires hospitalization and is done using a general or spinal anesthetic. It is now the most common surgery used to remove part of an enlarged prostate.
Urethra: a muscular tube that connects the bladder with the outside of the body
Ureters: two tubes that drain urine from the kidneys to the bladder
Urine: liquid produced by the kidneys, collected in the bladder and excreted through the urethra
Urinary Bladder: a hollow, muscular and distensible or elastic organ that sits on the pelvic floor
Urinary System: a group of organs in the body concerned with filtering out excess fluid and other substances from the bloodstream
References
- Graaff, Van De (2002). "Human Anatomy, Sixth Edition". New York: McGraw-Hill.
- Mader, Sylvia S. (2004). Human Biology. New York: McGraw-Hill.
- Smith, Peter (1998). Internet reference, The Role of the Kidney. Department of Clinical Dental Sciences,The University of Liverpool.
- McCance, Katherine L., Heuther, Sue E. (1994). "Pathophysiology: The Biological Basis for Disease In Adults and Children, Second Edition". Mosby-Year Book, Inc.