Human Physiology/Integumentary System
Homeostasis — Cells — Integumentary — Nervous — Senses — Muscular — Blood — Cardiovascular — Immune — Urinary — Respiratory — Gastrointestinal — Nutrition — Endocrine — Reproduction (male) — Reproduction (female) — Pregnancy — Genetics — Development — Answers
Introduction
[edit | edit source]The integumentary system consists of the skin, hair, nails, the subcutaneous tissue below the skin,and assorted glands.The most obvious function of the integumentary system is the protection that the skin gives to underlying tissues. The skin not only keeps most harmful substances out, but also prevents the loss of fluids.
A major function of the subcutaneous tissue is to connect the skin to underlying tissues such as muscles. Hair on the scalp provides insulation from cold for the head. The hair of eyelashes and eyebrows helps keep dust and perspiration out of the eyes, and the hair in our nostrils helps keep dust out of the nasal cavities. Any other hair on our bodies no longer serves a function, but is an evolutionary remnant. Nails protect the tips of fingers and toes from mechanical injury. Fingernails give the fingers greater ability to pick up small objects.
There are four types of glands in the integumentary system: Sudoriferous glands, Sebaceous glands, Ceruminous glands, and Mammary glands. Sudoriferous glands are sweat producing glands. These are important to help maintain body temperature. Sebaceous glands are oil producing glands which help inhibit bacteria, keep us waterproof and prevent our hair and skin from drying out. Ceruminous glands produce earwax which keeps the outer surface of the eardrum pliable and prevents drying. Mammary glands produce milk.
Skin
[edit | edit source]In zoology and dermatology, skin is an organ of the integumentary system made up of a layer of tissues that guard underlying muscles and organs. As the interface with the surroundings, it plays the most important role in protecting against pathogens. Its other main functions are insulation and temperature regulation, sensation and vitamin D and B synthesis. Skin is considered one of the most important parts of the body.
Skin has pigmentation, melanin, provided by melanocytes, which absorbs some of the potentially dangerous radiation in sunlight. It also contains DNA repair enzymes which reverse UV damage, and people who lack the genes for these enzymes suffer high rates of skin cancer. One form predominantly produced by UV light, malignant melanoma, is particularly invasive, causing it to spread quickly, and can often be deadly. Human skin pigmentation varies among populations in a striking manner. This has sometimes led to the classification of people(s) on the basis of skin color.
Damaged skin will try to heal by forming scar tissue, often giving rise to discoloration and depigmentation of the skin.
The skin is often known as "the largest organ in the human body". This applies to exterior surface, as it covers the body, appearing to have the largest surface area of all the organs. Moreover, it applies to weight, as it weighs more than any single internal organ, accounting for about 15 percent of body weight. For the average adult human, the skin has a surface area of between 1.5-2.0 square meters, most of it is between 2-3 mm thick. The average square inch of skin holds 650 sweat glands, 20 blood vessels, 60,000 melanocytes, and more than a thousand nerve endings.
The use of natural or synthetic cosmetics to treat the appearance of the face and condition of the skin (such as pore control and black head cleansing) is common among many cultures.
Layers
[edit | edit source]The skin has two major layers which are made of different tissues and have very different functions.

Skin is composed of the epidermis and the dermis. Below these layers lies the hypodermis or subcutaneous adipose layer, which is not usually classified as a layer of skin.
The outermost epidermis consists of stratified squamous keratinizing epithelium with an underlying basement membrane. It contains no blood vessels, and is nourished by diffusion from the dermis. The main type of cells which make up the epidermis are keratinocytes, with melanocytes and Langerhans cells also present. The epidermis can be further subdivided into the following strata (beginning with the outermost layer): corneum, lucidum, granulosum, spinosum, basale. Cells are formed through mitosis at the innermost layers. They move up the strata changing shape and composition as they differentiate, inducing expression of new types of keratin genes. They eventually reach the corneum and become sloughed off (desquamation). This process is called keratinization and takes place within about 30 days. This layer of skin is responsible for keeping water in the body and keeping other harmful chemicals and pathogens out.
Blood capillaries are found beneath the dermis, and are linked to an arteriole and a venule. Arterial shunt vessels may bypass the network in ears, the nose and fingertips.
The dermis lies below the epidermis and contains a number of structures including blood vessels, nerves, hair follicles, smooth muscle, glands and lymphatic tissue. It consists of loose connective tissue otherwise called areolar connective tissue—collagen, elastin and reticular fibers are present. Erector muscles, attached between the hair papilla and epidermis, can contract, resulting in the hair fiber pulled upright and consequentially goose bumps. The main cell types are fibroblasts, adipocytes (fat storage) and macrophages. Sebaceous glands are exocrine glands which produce a mixture of lipids and waxy substances known as sebum. Sebum serves many functions, including lubrication, water-proofing, softening, and also provides antimicrobial properties. Sweat glands open up via a duct onto the skin by a pore.
The dermis is made of an irregular type of fibrous connective tissue consisting of collagen and elastin fibers. It can be split into the papillary and reticular layers. The papillary layer is outermost and extends into the epidermis to supply it with vessels. It is composed of loosely arranged fibers. Papillary ridges make up the lines of the hands giving us fingerprints. The reticular layer is more dense and is continuous with the hypodermis. It contains the bulk of the structures (such as sweat glands). The reticular layer is composed of irregularly arranged fibers and resists stretching.
The hypodermis is not part of the skin, and lies below the dermis. Its purpose is to attach the skin to underlying bone and muscle as well as supplying it with blood vessels and nerves. It consists of loose connective tissue and elastin. The main cell types are fibroblasts, macrophages and adipocytes (the hypodermis contains 95% of body fat). Fat serves as padding and insulation for the body.
The patch drug delivery system. The transdermal patch is an increasingly popular drug delivery system. These patches are designed so that the drug molecules diffuse through the epidermis to the blood vessels in the dermis layer. A typical patch works well for small lipid-soluble molecules (for example, estrogen, nitroglycerin, and nicotine) that can make their way between epidermal cells.
Functions
[edit | edit source]- Protection: Skin gives an anatomical barrier between the internal and external environment in bodily defense; Langerhans cells in the skin are part of the immune system
- Sensation: Skin contains a variety of nerve endings that react to heat, cold, touch, pressure, vibration, and tissue injury; see somatosensory system and touch.
- Heat regulation: The skin contains a blood supply far greater than its requirements which allows precise control of energy loss by radiation, convection and conduction. Dilated blood vessels increase perfusion and heat loss while constricted vessels greatly reduce cutaneous blood flow and conserve heat. Erector pili muscles are significant in animals.
Tumors
[edit | edit source]- Benign tumors of the skin: Squamous cell papilloma
- Skin cancer
- Acne
- Keratosis pilaris
- Fungal infections such as athlete's foot
- microbial infections
- calcinosis cutis
- ulcer
Hair
[edit | edit source]Types of hair
[edit | edit source]Humans have three different types of hair:
- Lanugo, the fine, unpigmented hair that covers nearly the entire body of a fetus, although most has been replaced with vellus by the time of the baby's birth
- Vellus hair, the short, downy, "peach fuzz" body hair (also unpigmented) that grows in most places on the human body. While it occurs in both sexes, and makes up much of the hair in children, men have a much smaller percentage (around 10%) vellus whereas 2/3 of a female's hair is vellus.
- Terminal hair, the fully developed hair, which is generally longer, coarser, thicker, and darker than vellus hair, and often is found in regions such as the axillary, male beard, and pubic.
Pathological impacts on hair
[edit | edit source]Drugs used in cancer chemotherapy frequently cause a temporary loss of hair, noticeable on the head and eyebrows, because they kill all rapidly dividing cells, not just the cancerous ones. Other diseases and traumas can cause temporary or permanent loss of hair, either generally or in patches.
The hair shafts may also store certain poisons for years, even decades, after death. In the case of Col. Lafayette Baker, who died July 3, 1868, use of an atomic absorption spectrophotometer showed the man was killed by white arsenic. The prime suspect was Wallace Pollock, Baker's brother-in-law. According to Dr. Ray A. Neff, Pollack had laced Baker's beer with it over a period of months, and a century or so later minute traces of arsenic showed up in the dead man's hair. Mrs. Baker's diary seems to confirm that it was indeed arsenic, as she writes of how she found some vials of it inside her brother's suit coat one day.
Nails
[edit | edit source]
Parts of the fingernail
[edit | edit source]
The fingernail is an important structure made of keratin. The fingernail generally serve two purposes. It serves as a protective plate and enhances sensation of the fingertip. The protection function of the fingernail is commonly known, but the sensation function is equally important. The fingertip has many nerve endings in it allowing us to receive volumes of information about objects we touch. The nail acts as a counterforce to the fingertip providing even more sensory input when an object is touched.
Nail Structure
[edit | edit source]The structure we know of as the nail is divided into six specific parts - the root, nail bed, nail plate, eponychium (cuticle), perionychium, and hyponychium.
Root The root of the fingernail is also known as the germinal matrix. This portion of the nail is actually beneath the skin behind the fingernail and extends several millimeters into the finger. The fingernail root produces most of the volume of the nail and the nail bed. This portion of the nail does not have any melanocytes, or melanin producing cells. The edge of the germinal matrix is seen as a white, crescent shaped structure called the lunula.
Nail Bed The nail bed is part of the nail matrix called the sterile matrix. It extends from the edge of the germinal matrix, or lunula, to the hyponychium. The nail bed contains the blood vessels, nerves, and melanocytes, or melanin-producing cells. As the nail is produced by the root, it streams down along the nail bed, which adds material to the undersurface of the nail making it thicker. It is important for normal nail growth that the nail bed be smooth. If it is not, the nail may split or develop grooves that can be cosmetically unappealing.
Nail Plate The nail plate is the actual fingernail, made of translucent keratin. The pink appearance of the nail comes from the blood vessels underneath the nail. The underneath surface of the nail plate has grooves along the length of the nail that help anchor it to the nail bed.
eponychium The cuticle of the fingernail is also called the eponychium. The cuticle is situated between the skin of the finger and the nail plate fusing these structures together and providing a waterproof barrier.
Perionychium The perionychium is the skin that overlies the nail plate on its sides. It is also known as the paronychial edge. The perionychium is the site of hangnails, ingrown nails, and an infection of the skin called paronychia.
Hyponychium The hyponychium is the area between the nail plate and the fingertip. It is the junction between the free edge of the nail and the skin of the fingertip, also providing a waterproof barrier.

Nail Diseases
[edit | edit source]Nail diseases are in a separate category from diseases of the skin. Although nails are a skin appendage, they have their own signs and symptoms which may relate to other medical conditions. Nail conditions that show signs of infection or inflammation require medical assistance and cannot be treated at a beauty parlor. Deformity or disease of the nails may be referred to as onychosis.
There are many disease that can occur with the fingernails and toenails. The most common of these diseases are ingrown nails and fungal infections.
Ingrown Nails
[edit | edit source]Onychocryptosis, commonly known as "ingrown nails" (unguis incarnatus), can affect either the fingers or the toes. In this condition, the nail cuts into one or both sides of the nail bed, resulting in inflammation and possibly infection. The relative rarity of this condition in the fingers suggests that pressure from the ground or shoe against the toe is a prime factor. The movements involved in walking or other physical disturbances can contribute to the problem. Mild onychocryptosis, particularly in the absence of infection, can be treated by trimming and rounding the nail. More advanced cases, which usually include infection, are treated by surgically excising the ingrowing portion of the nail down to its bony origin and cauterizing the matrix, or 'root', to prevent recurrence. This surgery is called matricectomy. The best results are achieved by cauterizing the matrix with phenol. Another method, which is much less effective, is excision of the matrix, sometimes called a 'cold steel procedure'
Nail Fungus
[edit | edit source]An infection of nail fungus (onychomycosis) occurs when fungi infect one or more of your nails. Onychomycosis generally begins as a white or yellow spot under the tip of the fingernail or toenail. As the nail fungus spreads deeper into the nail, it may cause the nail to discolor, thicken and develop crumbling edges — an unsightly and potentially painful problem.
Infections of nail fungus account for about half of all nail disorders. These infections usually develop on nails continually exposed to warm, moist environments, such as sweaty shoes or shower floors. Nail fungus isn't the same as athlete's foot, which primarily affects the skin of the feet, but at times the two may coexist and can be caused by the same type of fungus. Topical steroid misuse is one of the most common cause now a days.
An infection with nail fungus may be difficult to treat, and infections may recur. But medications are available to help clear up nail fungus permanently.
Clinical Application
[edit | edit source]Nail inspection can give a great deal of information about the internal working of the body as well, and like tongue or iris inspection, has a long history of diagnostic use in cantraditional medical practices such as Chinese medicine.
Pliability:
Brittleness is associated with iron deficiency, thyroid problems, impaired kidney function, circulation problems[2], and biotin deficiency[3] Splitting and fraying are associated with psoriasis, folic acid, protein and/or Vitamin C deficiency. Unusual thickness is associated with circulation problems. Thinning nails and itchy skin are associated with lichen planus[4].
Shape and texture:
Clubbing, or nails that curve down around the fingertips with nail beds that bulge is associated with oxygen deprivation and lung, heart, or liver disease. Spooning, or nails that grow upwards is associated with iron or B12 deficiency. Flatness can indicate a B12 vitamin deficiency[5] or Raynaud's disease[6] Pitting of the nails is associated with Psoriasis. Horizontal ridges indicate stress, and Beau's lines are associated with many serious conditions. Vertical ridges are associated with arthritis[7]. Vertical grooves are associated with kidney disorders, aging, and iron deficiency[8]. Beading is associated with rheumatoid arthritis[9]. Nails that resemble hammered brass are associated with (or portend) hair loss[10]. Short small beds are associated with heart disease[11].
Coloration of the nail bed:
Mee's lines are associated with arsenic or thallium poisoning, and renal failure. White lines across the nail are associated with heart disease, liver disease, or a history of a recent high fever[12]. Opaque white nails with a dark band at the fingertip are associated with cancer, cirrhosis, congestive heart failure, diabetes and aging[13]. Paleness or whitening is associated with liver or kidney disease and anemia[14]. Yellowing of the nail bed is associated with chronic bronchitis, lymphatic problems, diabetes, and liver disorders. Brown or copper nail beds are associated with arsenic or copper poisoning, and local fungal infection. Grey nail beds are associated with arthritis, edema, malnutrition, post-operative effects, glaucoma and cardio-pulmonary disease[15]. redness is associated with heart conditions. dark nails are associated with B12 deficiency. Stains of the nail plate (not the nail bed) are associated with nail polish[16], smoking, and henna use.
Markings:
Pink and white nails are associated with kidney disease[17]. Parallel white lines in the nails are associated with hypoalbuminemia. red skin at the base of the nail is associated with connective tissue disorders[18]. blue lunulae are associated with silver poisoning or lung disorder[19]. blue nail beds are (much like blue skin) associated with poor oxygenation of the blood (asthma, emphysema, etc)[20]. small white patches are associated with zinc or calcium deficiency or malabsorption, parasites, or local injury[21]. receded lunulae (fewer than 8) are associated with poor circulation[22], shallow breathing habits or thyroid dysfunction[23]. large lunulae (more than 25% of the thumb nail) is associated with high blood pressure.
Glands
[edit | edit source]Sudoriferous(Sweat Glands)
[edit | edit source]
In humans, there are two kinds of sweat glands which differ greatly in both the composition of the sweat and its purpose: Also "click" here"How our body Sweats" to see a short movie on sweat glands.
Eccrine (a.k.a. merocrine)
[edit | edit source]Eccrine sweat glands are exocrine glands distributed over the entire body surface but are particularly abundant on the palms of hands, soles of feet, and on the forehead. These produce sweat that is composed chiefly of water (99%) with various salts. The primary function is body temperature regulation.
Eccrine sweat glands are coiled tubular glands derived leading directly to the most superficial layer of the epidermis (outer layer of skin) but extending into the inner layer of the skin (dermis layer). They are distributed over almost the entire surface of the body in humans and many other species but are lacking in some marine and fur-bearing species. The sweat glands are controlled by sympathetic cholinergic nerves which are controlled by a center in the hypothalamus. The hypothalamus senses core temperature directly, and also has input from temperature receptors in the skin and modifies the sweat output, along with other thermoregulatory processes.
Human eccrine sweat is composed chiefly of water with various salts and organic compounds in solution. It contains minute amounts of fatty materials, urea, and other wastes. The concentration of sodium varies from 35–65 mmol/l and is lower in people acclimatized to a hot environment. The sweat of other species generally differs in composition.
Apocrine
[edit | edit source]Apocrine sweat glands only develop during early- to mid-puberty (approximately age 15) and release more than normal amounts of sweat for approximately a month and subsequently regulate and release normal amounts of sweat after a certain period of time. Apocrine sweat glands produce sweat that contains fatty materials. These glands are mainly present in the armpits and around the genital area and their activity is the main cause of sweat odor, due to the bacteria that break down the organic compounds in the sweat from these glands. Emotional stress increases the production of sweat from the apocrine glands, or more precisely: the sweat already present in the tubule is squeezed out. Apocrine sweat glands essentially serve as scent glands.
In some areas of the body, these sweat glands are modified to produce wholly different secretions, including the cerumen ("wax") of the outer ear. Other glands, such as Mammary glands, are greatly enlarged and modified to produce milk.
Sebaceous Glands
[edit | edit source]
The sebaceous glands are glands found in the skin of mammals. They secrete an oily substance called sebum (Latin, meaning fat or tallow) that is made of fat (lipids) and the debris of dead fat-producing cells. These glands exist in humans throughout the skin except in the palms of the hands and soles of the feet. Sebum acts to protect and waterproof hair and skin, and keep them from becoming dry, brittle, and cracked. It can also inhibit the growth of microorganisms on skin.
Sebaceous glands can usually be found in hair-covered areas where they are connected to hair follicles to deposit sebum on the hairs, and bring it to the skin surface along the hair shaft. The structure consisting of hair, hair follicle and sebaceous gland is also known as pilosebaceous unit. Sebaceous glands are also found in non haired areas of lips, eyelids, penis, labia minora and nipples; here the sebum reaches the surface through ducts. In the glands, sebum is produced within specialized cells and is released as these cells burst; sebaceous glands are thus classified as holocrine glands.
Sebum is odorless, but its bacterial breakdown can produce odors. Sebum is the cause of some people experiencing "oily" hair if it is not washed for several days. Earwax is partly sebum, as is mucopurulent discharge, the dry substance accumulating in the corners of the eye after sleeping.

The composition of sebum varies from species to species; in humans, the lipid content consists of about 25% wax monoesters, 41% triglycerides, 16% free fatty acids, and 12% squalene.
The activity of the sebaceous glands increases during puberty because of heightened levels of androgens.
Sebaceous glands are involved in skin problems such as acne and keratosis pilaris. A blocked sebaceous gland can result in a sebaceous cyst. The prescription drug isotretinoin significantly reduces the amount of sebum produced by the sebaceous glands, and is used to treat acne. The extreme use (up to 10 times doctor prescribed amounts) of anabolic steroids by bodybuilders to prevent weight loss tend to stimulate the sebaceous glands which can cause acne.
The sebaceous glands of a human fetus in utero secrete a substance called Vernix caseosa, a "waxy" or "cheesy" white substance coating the skin of newborns.
The preputial glands of mice and rats are large modified sebaceous glands that produce pheromones.
Ceruminous glands
[edit | edit source]
Earwax, also known by the medical term cerumen, is a yellowish, waxy substance secreted in the ear canal of humans and many other mammals. It plays a vital role in the human ear canal, assisting in cleaning and lubrication, and also provides some protection from bacteria, fungus, and insects. A comprehensive review of the physiology and pathophysiology of cerumen can be found in Roeser and Ballachanda. Excess or impacted cerumen can press against the eardrum and/or occlude the external auditory canal and impair hearing.
Production, composition, and different types
[edit | edit source]Cerumen is produced in the outer third of the cartilaginous portion of the human ear canal. It is a mixture of viscous secretions from sebaceous glands and less-viscous ones from modified apocrine sweat glands.
Two distinct genetically determined types of earwax are distinguished -- the wet-type which is dominant, and the dry type which is recessive. Asians and Native Americans are more likely to have the dry type of cerumen (grey and flaky), whereas Caucasians and Africans are more likely to have the wet type (honey-brown to dark-brown and moist). Cerumen type has been used by anthropologists to track human migratory patterns, such as those of the Inuit.
The difference in cerumen type has been tracked to a single base change (an single nucleotide polymorphism) in a gene known as "ATP-binding cassette C11 gene". In addition to affecting cerumen type, this mutation also reduces sweat production. The researchers conjecture that the reduction in sweat was beneficial to the ancestors of East Asians and Native Americans who are thought to have lived in cold climates.
Function
[edit | edit source]
Cleaning. Cleaning of the ear canal occurs as a result of the "conveyor belt" process of epithelial migration, aided by jaw movement. Cells formed in the center of the tympanic membrane migrate outwards from the umbo (at a rate equivalent to that of fingernail growth) to the walls of the ear canal, and accelerate towards the entrance of the ear canal. The cerumen in the canal is also carried outwards, taking with it any dirt, dust, and particulate matter that may have gathered in the canal. Jaw movement assists this process by dislodging debris attached to the walls of the ear canal, increasing the likelihood of its extrusion.
Lubrication. Lubrication prevents desiccation and itching of the skin within the ear canal (known as asteatosis). The lubricative properties arise from the high lipid content of the sebum produced by the sebaceous glands. In wet-type cerumen at least, these lipids include cholesterol, squalene, and many long-chain fatty acids and alcohols.
Antibacterial and antifungal roles. While studies conducted up until the 1960s found little evidence supporting an antibacterial role for cerumen, more recent studies have found that cerumen provides some bactericidal protection against some strains of bacteria. Cerumen has been found to be effective in reducing the viability of a wide range of bacteria (sometimes by up to 99%), including Haemophilus influenzae, Staphylococcus aureus, and many variants of Escherichia coli. The growth of two fungi commonly present in otomycosis was also significantly inhibited by human cerumen. These antimicrobial properties are due principally to the presence of saturated fatty acids, lysozyme and, especially, to the relatively low pH of cerumen (typically around 6.1 in normal individuals).
Mammary Glands
[edit | edit source]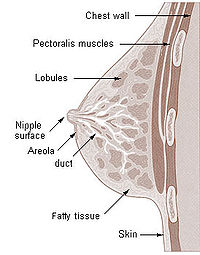
Mammary glands are the organs that, in the female mammal, produce milk for the sustenance of the young. These exocrine glands are enlarged and modified sweat glands and are the characteristic of mammals which gave the class its name.
Structure
[edit | edit source]The basic components of the mammary gland are the alveoli (hollow cavities, a few millimetres large) lined with milk-secreting epithelial cells and surrounded by myoepithelial cells. These alveoli join up to form groups known as lobules, and each lobule has a lactiferous duct that drains into openings in the nipple. The myoepithelial cells can contract, similar to muscle cells, and thereby push the milk from the alveoli through the lactiferous ducts towards the nipple, where it collects in widenings (sinuses) of the ducts. A suckling baby essentially squeezes the milk out of these sinuses.

1 - Fat
2 - Lactiferous duct/lobule
3 - Lobule
4 - Connective tissue
5 - Sinus of lactiferous duct
6 - Lactiferous duct
One distinguishes between a simple mammary gland, which consists of all the milk-secreting tissue leading to a single lactiferous duct, and a complex mammary gland, which consists of all the simple mammary glands serving one nipple.
Humans normally have two complex mammary glands, one in each breast, and each complex mammary gland consists of 10-20 simple glands. (The presence of more than two nipples is known as polythelia and the presence of more than two complex mammary glands as polymastia.)
Also, "click" this;"Breast tissue", to this a movie visual of the breast.
Development and hormonal control
[edit | edit source]The development of mammary glands is controlled by hormones. The mammary glands exist in both sexes, but they are rudimentary until puberty when in response to ovarian hormones, they begin to develop in the female. Click this [1]to see what breast tissue does in a female during menstruation. Estrogen promotes formation, while testosterone inhibits it.
At the time of birth, the baby has lactiferous ducts but no alveoli. Little branching occurs before puberty when ovarian estrogens stimulate branching differentiation of the ducts into spherical masses of cells that will become alveoli. True secretory alveoli only develop in pregnancy, where rising levels of estrogen and progesterone cause further branching and differentiation of the duct cells, together with an increase in adipose tissue and a richer blood flow.
Colostrum is secreted in late pregnancy and for the first few days after giving birth. True milk secretion (lactation) begins a few days later due to a reduction in circulating progesterone and the presence of the hormone prolactin. The suckling of the baby causes the release of the hormone oxytocin which stimulates contraction of the myoepithelial cells.
Breast cancer
[edit | edit source]As described above, the cells of mammary glands can easily be induced to grow and multiply by hormones. If this growth runs out of control, cancer results. Almost all instances of breast cancer originate in the lobules or ducts of the mammary glands.
Types of breast cancer
- DCIS: Ductal Carcinoma in Situ
- LCIS: Lobular Carcinoma in Situ
- Invasive ductal carcinoma
- Invasive lobular carcinoma
- Inflammatory breast cancer
- Paget's disease

Homeostasis
[edit | edit source]As a whole, the integumentary system plays a big part in maintaining homeostasis. The integumentary system is the outermost organ system of the body and many of its functions are related to this location. The skin protects the body against pathogens and chemicals, minimizes loss or entry of water, and blocks the harmful effects of sunlight. Sensory receptors in the skin provide information about the external environment, helping the skin regulate body temperature in response to environmental changes and helping the body react to pain and other tactile stimuli. The large surface area of the skin makes it ideal for temperature regulation. The rate of heat loss can be regulated by the amount of blood flowing through the blood vessels in the dermis close to the surface of the skin. When the body temperature rises, as for example during exercise, sympathetic tone is reduced and this brings about dilation of the blood vessels supplying the skin. The increase in skin blood flow allows heat to be lost more rapidly so that body temperature does not rise above the normal homeostatic range. The rate of heat loss can also be boosted by the production of sweat, which takes up additional heat as it evaporates. Conversely, if heat production is less than required, the dermal vessels constrict, sweating stops, and heat is conserved by the body.
Glossary
[edit | edit source]- Areolar
- Areolar connective tissue is a pliable, mesh-like tissue with a fluid matrix and functions to cushion and protect body organs. It acts as a packaging tissue holding the internal organs together and in correct placement.
- Basal lamina
- Basal lamina (often erroneously called basement membrane) is a layer on which epithelium sits. This layer is composed of an electron-dense layer (lamina densa) between two electron-lucid layers (lamina lucida), and is approximately 40-50 nm thick (with exceptions such as the 100-200 nm glomerular basement membrane).
- Dermis
- The dermis is the layer of skin beneath the epidermis that consists of connective tissue and cushions the body from stress and strain. The dermis is tightly connected to the epidermis by a basement membrane.
- Epidermis
- The epidermis is the outermost layer of the skin. It forms the waterproof, protective wrap over the body's surface and is made up of stratified squamous epithelium with an underlying basal lamina.
- Fibroblasts
- A fibroblast is a cell that makes the structural fibers and ground substance of connective tissue.
- Hair follicle
- A hair follicle is part of the skin that grows hair by packing old cells together.
- Hypodermis
- The hypodermis (also called the hypoderm), is the lowermost layer of the integumentary system in vertebrates. It is derived from the mesoderm, but unlike the dermis, it is not derived from the dermatome region of the mesoderm.
- Impetigo
- This is a superficial skin infection most common among children age 2–6 years. People who play close contact sports such as rugby, American football and wrestling are also susceptible, regardless of age. The name derives from the Latin impetere ("assail"). It is also known as school sores.
- Melanocytes
- These are cells located in the bottom layer of the skin's epidermis and in the middle layer of the eye, the uvea. Through a process called melanogenesis, these cells produce melanin, a pigment in the skin, eyes, and hair.
- Melanoma
- A melanoma is a malignant tumor that originates in melanocytes. It is a highly malignant form of skin cancer, and, though rare, is responsible for the majority of skin cancer-related deaths.
- Onychosis
- Deformity or disease of the nails
- Papillary
- The papillary layer is outermost and extends into the epidermis to supply it with vessels. It is composed of loosely arranged fibres. Papillary ridges make up the lines of the hands.
- Recticular Layer
- The reticular layer is more dense and is continuous with the hypodermis. It contains the bulk of the structures (such as sweat glands). The reticular layer is composed of irregularly arranged fibres and resists stretching.
- For more fun pictures of other skin diseases and skin problems "click" to this cool website
- "Dermatology Image Database". Note: From this link then click "Clinical Skin Diseases Images".
Review Questions
[edit | edit source]- Answers for these questions can be found here
1. Name all of the parts of the integumentary system.
2. Name the cells that produce melanin and describe its function.
3. Name and describe the importance of the cutaneous senses.
4. Explain how sweating helps maintain normal body temperature.
5. Explain where on the body hair has important functions and describe these functions.
6. What is a melanoma?
A) The outermost layer of skin
B) A type of nail disease
C) A malignant tumor that originates in melanocytes
D) The lower most layer of skin
References
[edit | edit source]- Brannon, Heather (2006). "Nail Anatomy" About, Inc., A part of The New York Times Company.
- Cobb, Judith. Fingernails, Jewels or Tools? Nature's Field - Nail diagnosis
- Graaff, Van De (2002). Human Anatomy, Sixth Edition. New York: McGraw-Hill.
- Mader, Sylvia S. (2004). Human Biology. New York: McGraw-Hill.
- Sorrentino, Sheila A. (2004). Mosby's textbook for Nursing Assistants, 6th Edition. St. Louis, Missouri: Mosby.