Basic Physics of Digital Radiography/The Image Receptor

Technological aspects of digital radiography image receptors are described in this chapter. These receptors are generally used for radiography and some can also be used for fluoroscopy. As a result, in addition to single-shot radiography, other exposure modes can also be used with the technology described. The use of continuous X-ray exposures in fluoroscopy generally refers to the use of low XRT currents (i.e. 0.5 to 5 mA) - see Figure 4.1. The resultant images have a low image quality but are sufficient for applications such as patient positioning or monitoring catheter placement. Its use is also commonly called Screening, a reference to the days when a sheet of glass coated with a fluorescent material was used for such imaging. By contrast, the term fluorography generally refers to the use of relatively intense (e.g. 50 to 1000 mA), pulsed exposures. Pulses are typically of short duration and can be applied at a rate of, for example, 1 to 8 per second. The resultant images have a relatively high image quality and can therefore be used for diagnostic purposes.
Computed Radiography
[edit | edit source]We have previously described the process of photostimulable luminescence which is exploited in Computed Radiography, where the absorption of radiation causes electrons to become trapped at intermediate energy levels. Phosphors having this property are therefore referred to as Storage Phosphors.
A latent X-ray image can be recorded using a plate coated with crystals of barium fluorohalide compounds which contain trace amounts of europium. The general form of these compounds is BaFlX:Eu, where X can be Cl, Br or I or a mixture thereof. Radiographic information is recorded by elevating electrons to traps in the energy gap and the number of filled traps is proportional to the amount of radiant energy absorbed. When stimulated by visible radiation of wavelength around 600 to 680 nm (i.e. red light), the crystals luminesce as the electrons return to their ground state in the range 300-500 nm (blue).
Laser Readout
[edit | edit source]
- The plate can be scanned in a raster pattern with a finely focused laser beam, e.g. He/Ne, and a scanning mirror - see Figure 4.2. The laser light stimulates the release of electrons from the traps giving rise to the emission of light which is collected by a light guide and fed to a photodetector, e.g. a photomultiplier tube. The signals generated by the photodetector as the plate is being scanned are amplified and digitized by an analogue-to-digital converter (ADC).
- The image is in essence built up point by point and line by line to give a digital image resolution of up to 4k x 4k pixels. Pixel size is typically 0.1 μm. The imaging cycle is completed by flooding the plate with a high intensity sodium discharge lamp that erases any remnants of the latent image and essentially prepares the plate for reuse - see Figure 4.3.
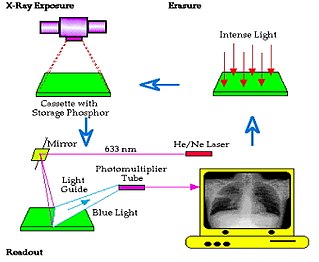
- The spatial resolution of computed radiography is influenced by factors such as the phosphor plate thickness, the readout time and the diameter of the laser beam, which is typically about 100 μm. Note that divergence through scattering of the laser light in the body of the phosphor layer will broaden the stimulated area to beyond this diameter.
- Note that the nature of the CR imaging process limits its application to single-shot radiographic imaging. In clinical practice, the process is generally part of a workflow where patient radiographs are recorded as traditionally in film/screen radiography, but with images now generated with a latent image read-out device and automatically sent to a quality control workstation for image evaluation, annotation and transfer to a PACS for reporting.
Imaging Plate
[edit | edit source]
- The CR imaging plate is very similar to intensifying screens in its structure. It consists of tiny phosphor grains of about 5 μm embedded in an organic binder which is coated onto a substrate material. The plate is turbid and as a result scatters light (both excitation laser and stimulated light) strongly and isotropically - see Figure 4.4. Thus, the light diffusion limits the useful thickness of the phosphor layer. An improvement in X-ray absorption efficiency can indeed be obtained by increasing the thickness of the phosphor layer. However,
- lateral diffusion of light in the phosphor layer will increase in proportion to the layer thickness, impairing spatial resolution; and
- sensitivity will not increase all that much when the layer exceeds a certain thickness, because most of the light stimulated deep in the layer will not reach the surface for detection.
- This sensitivity limitation can be overcome by making the substrate of the imaging plate from a transparent material and to detect the photo-stimulated luminescence from both the front and the back sides of the plate[1]. This requires two light-collection systems, but only one laser beam. The improved sensitivity results since only ~30% of the photostimulated light is collected using the conventional single laser approach. In addition, sensitivity improvements have been achieved using a structured phosphor, e.g. CsBr:Eu - see the discussion below - as the imaging plate[2].
A fundamental limitation of CR is the time required to read the latent image. Since the decay time of the phosphor luminescence is ~0.7 μs typically, the readout of a 3,000x3,000 pixel image can take over half a minute to complete. An improvement can be obtained by line scanning, where a full line of pixels is stimulated and read out simultaneously instead of single pixels, as described above. This line-scanning approach requires a linear array of laser light sources, e.g. laser diodes, as well as a linear array of photodetectors as wide as the imaging plate, and gives rise to readout times of less than 10 seconds. Furthermore, the linear scanning mechanism can be built into the image receptor cassette[3].
Note that clinical radiography with CR plates has been found to generate a range of unique artefacts, which are the subject of a pictorial review in Cesar et al. (2001)[4].
Direct Radiography
[edit | edit source]
Considerable research has been conducted in recent years into the development of flat panel image receptors for digital radiography. This research has extended from the development of active-matrix liquid-crystal flat panel displays (AMLCD) for application in, for example, laptop computers. The underlying technology of AMLCDs is a large area integrated circuit called an active matrix array which consists of many millions of identical semiconductor elements deposited on a substrate material. An intensifying screen or a photoconductor coupled to such an active matrix array forms the basis of flat panel X-ray image receptors. These detectors have been applied for both radiography and fluoroscopy.
Such a receptor is illustrated in Figure 4.5, where the active matrix array and associated electronic circuitry is mounted in a cassette. Array sizes of up to 43 cm x 43 cm are available with more than 9 million pixels (pixel size ~140 μm). Operation of the array is controlled by a digital image processor (see the next chapter), which also stores and displays the resultant images.
A simplified description of the operation is illustrated in Figure 4.6. Each pixel of the array has a switch (typically made from a thin film transistor) which is connected to switching control circuitry in a manner which allows all switches in a row of the array to be operated simultaneously. The output from each pixel is connected in columns with individual pre-amplifiers. All switches are kept in the off position during the X-ray exposure. Following the exposure, the switches in the first row are turned on and the signal from each pixel is amplified by the pre- amplifiers, digitized using an ADC and stored in the image memory of the digital image processor. These switches are then turned off and the switches in the second row are turned on to acquire signals from the second row of pixels. This process is repeated for the whole array so that an image is acquired in a sequential, line-by-line manner. When the receptor is used for fluoroscopy the array is scanned continuously[5]

Research developments have advanced on two fronts as illustrated in Figure 4.7.
Indirect Receptors
[edit | edit source]- Indirect receptors are based on coupling an intensifying screen to the active matrix array. Phosphors such as Gd2O2S:Tb and CsI:Tl have been used, and the light produced following X-ray interaction is detected by an array of pixels consisting of photodetectors - see panel (a) in the figure. Each photodetector generates an electric charge that is proportional to the amount of light striking it, and this charge is stored until it is read-out by the switching control circuitry. The detection process is referred to as indirect since the detected X-rays are first converted to the light, which is subsequently converted to electric charge.
- CsI:Tl has distinct advantages as an intensifying screen because it has favourable K-absorption edges at 33 keV (I) and 36 keV (Cs) and its crystals can be grown in a dense, needle-like (5-10 μm in diameter) structure in a thin layer up to 600 μm thick[6] Fluorescent light generated by X-ray absorption can therefore be guided fiber-optically to the photodetector array without much lateral dispersion. CsI:Tl as a result is a so-called Structured Phosphor, as opposed to the dispersed powder phosphor obtained using Gd2O2S:Tb and similar screens. The packing density of scintillation sites in CsI:Tl is also quite high as a result of its crystalline structure, whereas a powder screen consists of only about 60% phosphor and 40% binder. This results in an absorption efficiency for structured phosphors to be about four times higher than that of a powder screen with similar spatial resolution capabilities.
- CsI:Tl fluoresces in the green region of the visible spectrum, where the light absorption efficiency of a-Si is relatively high.
- Indirect receptors have also found application in Computed Tomography. In MDCT, for instance, arrays of up to 916 columns by 64 rows of detector elements made from a phosphorescent material are coupled to an a-Si array of photodiodes. Ultra-Fast Ceramic (UFC) detectors which are manufactured as doped gadolinium oxysulfide crystals feature a relatively fast response, high detection efficiency and broad dynamic range. In addition, collimator blades can be mounted directly on the detector array for scatter reduction purposes.
 |
 |
Direct Receptors
[edit | edit source]- Direct receptors are based on coupling a photoconductor to the active matrix array. Photoconductors such as amorphous selenium (a-Se) have been used, and the electric charge produced following X-ray interaction is detected by an array of pixels each consisting of an electrode and a capacitor - see panel (b). This charge is stored in each capacitor until it is read-out by the electronic switching circuitry. The photoconductor requires a voltage of the order of 5,000 V to be applied, using a surface electrode, so that the charge produced can be attracted to the pixel electrodes.
- It should be noted that the photoconductive properties of amorphous selenium (a-Se) have been known for many years and have been widely applied in photocopiers, fax machines and laser printers. The direct imaging technique has evolved from xeroradiography, which was a popular medical imaging technique many years ago.
- Selenium is not as efficient as cesium iodide as an X-ray absorption material because of its lower atomic number (Z=34). Its K-absorption edge is at 13 keV and its attenuation falls off rapidly with increasing energy. It can be expected on this basis that rather thick layers of a-Se are required to absorb X-ray photons with equal efficiency to CsI at higher X-ray energies. Other potential materials such as lead oxide (PbO), lead iodide (PbI2) and mercuric iodide (HgI2) exist which have better absorption efficiencies than selenium for a given layer thickness and may find application in the future[7].
Important design features of flat panel image receptors include the pixel size and the fill factor. Pixel size affects spatial resolution and sizes of the order of about 100-200 μm are typical. The fill factor is the percentage of a pixel area which is sensitive to the image signal - be it electric charge or light photons. It can never be 100%, given the need to accommodate conductors (~10 μm wide) which input switching signals and which output image signals, as well as the thin film transistor in each pixel. Typical fill factors are in the range 50-80%.
Flat-panel detectors generally use active matrices of hydrogenated amorphous silicon (a-Si:H+) as readout arrays. This is the technology developed for laptop displays which makes it possible to manufacture large-area X-ray imagers with high radiation tolerance. The amorphous silicon layer is formed on a glass substrate, for instance, by plasma-enhanced deposition of silane (SiH4) gas. The disordered structure of the amorphous layer has the advantage that X-ray detection can occur without radiation damage to the material. The material can therefore be repeatedly exposed with comparatively intense X-ray beams. The active matrix array is manufactured from the a-Si layer by photolithography and chemical etching techniques, as widely used in integrated circuit manufacture.
However, a-Si is limited by the minimum size of the structures that can be built into this material. Another possibility is a readout array based on complementary metal-oxide semiconductor (CMOS) technology. CMOS is made using crystalline silicon wafers instead of amorphous silicon and is highly developed in the semiconductor industry. CMOS imagers provide a high fill-factor and very fast readouts. In addition, it is possible to integrate on-chip electronics (e.g. amplifiers) for each pixel, which can improve performance significantly and may someday provide X-ray energy discrimination capabilities. Their use in DR however has been limited because of significant electronic noise.
A variant on the design of indirect detectors is to mount the photodiode/TFT array on the anterior side of the intensifying screen - so called Irradiation Side Sampling (ISS)[8]. The benefit here is an improved detection geometry between the scintillation sites in the screen and the photodiodes which reduces light attenuation and blurring effects.
An interesting hybrid design can be obtained using features of both the indirect and direct image receptors. Here a structured phosphor is coupled to a thin a-Se layer and has a potential advantage when electron amplification is controlled using programmable applied voltages.
Reduction of electronic noise generated by TFTs and associated circuitry can be achieved using optical readout of direct detectors. Here two layers of a-Se are used separated by an electron-trapping layer (ETL). One layer is used to generate electrons when X-rays are absorbed which are trapped by the ETL, and the second thinner layer is used to read this charge when it is illuminated by a line-scanning array of light-emitting diodes[9].
XII-Video Systems
[edit | edit source]
The basic elements of an X-ray Image Intensifier (XII) and video system are shown in the Figure 4.8. X-rays emerging from the patient are converted to an optical image in the XII, which is viewed by a video camera and displayed using a computer system. These systems are widely used for fluoroscopy and fluorography during barium-studies, angiography and interventional radiology. Their historical development is reviewed in Balter (2019)[10].
Many systems also feature a mechanism for placing a CR or DR cassette at the XII input so that radiographic images can be recorded. This device is sometimes referred to as a Cassette Changer and may allow a number of images to be recorded onto one image receptor. Units incorporating cassette changers are sometimes referred to as Radiography/Fluoroscopy (R/F) systems - see Figure 4.9.
X-Ray Image Intensifier
[edit | edit source]
- Figure 4.10 illustrates the essential features of an X-ray image intensifier. After the X-ray beam emerges from the patient, it enters the XII tube to be absorbed by the input phosphor and thus create light photons. These photons strike a photocathode and cause it to emit electrons. The electrons are accelerated towards the output phosphor by a high electric field produced between the anode and photocathode. Focusing is accomplished by the focusing lenses. The electrons hit the output phosphor and cause large numbers of light photons to be produced which carry the fluoroscopic image. By this complex means (see Figure 4.11), the XII converts an X-ray image to an electro-optically intensified light image.
- Image intensification also results because the output phosphor is so much smaller than the input phosphor. Output phosphors are typically about 2 cm in diameter while input phosphors may vary in diameter from about 15 to 40 cm, depending on the clinical application. Intensification through image minification can therefore range from factors of about 56 to 400. Additional intensification is achieved by the electron acceleration inside the tube, i.e. the Flux Gain. The overall brightness gain achieved (i.e. the minification times the flux gain) can be over 5,000[11].
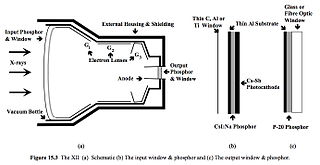
Fig. 4.10: The X-ray image intensifier (a), with close-ups of the phosphor/photocathode sandwich (b) and the output phosphor (c).
- The input window is usually made of a thin layer of titanium, carbon fiber or aluminium so as to minimize X-ray absorption. The input phosphor is usually cesium iodide activated with sodium (CsI:Na). The input phosphor and photocathode must be in intimate contact with each other in order to preserve the latent image fidelity - see panel (b). Electrons are produced in direct proportion to the brightness of the input phosphor and are accelerated through a potential of 25-35 kV before striking the output phosphor. This accelerating anode is located in the neck of the evacuated tube.
- The electrostatic focusing lenses (G1, G2 and G3) are at a positive potential with respect to the cathode. The photocathode is actually curved (unlike that shown in Figure 4.10) to equalize the path lengths of all electrons so as to minimize image distortion.

- The output phosphor is generally made from a phosphor called P20. This phosphor emits green light which matches well with the sensitivity of video cameras. A very thin layer of aluminium is plated onto this output phosphor to prevent light from being reflected back through the tube and activating the photocathode - see panel (c). This layer also serves as an earth to remove spent electrons from the tube.
- The glass envelope is encased in a lead lined canister which provides a degree of radiation protection from stray X-rays. Protection from external magnetic fields is also incorporated. Many XII designs also incorporate a fixed radiographic grid at the input.
- Variable field sizes can be achieved by altering the voltage on the electrostatic lens G3 illustrated in Figure 4.10. An increase in this voltage can be used to decrease the area of the input phosphor that can be imaged on the output phosphor but it also decreases the Minification Gain. An increase in radiation exposure (i.e. mA) is generally needed to compensate. Such variable field sizes can be useful when fine control is required in interventional radiology, for example. However, it should be appreciated that the consequent change in patient exposure is inversely related to the square of the field size when images of equivalent brightness are needed.
- It should be appreciated that even with substantial brightness gains the image on the output phosphor remains very dull and direct viewing is not practicable. This is one reason why a video camera is generally used to view the XII output. Furthermore, it should be appreciated that XII images suffer from effects such as pincushion distortion and vignetting.
Video Camera
[edit | edit source]- The video camera views the XII output through optical coupling consisting a simple system of lenses and an aperture. The aperture can be used to control the amount of light striking the camera. Alternatively, the video camera and XII can be coupled fiber-optically.
- There are two general types of video camera used for fluoroscopy. The traditional device is called a photoconductive camera or Pick-Up Tube (PUT) and is illustrated in the following figure, and the more recent semiconductor or CCD camera. Both cameras generate images in the form of a video signal, but in substantially different ways. The operation of these cameras is described below.
- Photoconductive Video Camera
- The PUT camera uses a photosensor which is called the target. The output image of the XII is focused onto a target assembly (see Figure 4.12) which is made from a three layer sandwich. The first layer is a glass face plate which serves only to maintain the vacuum whilst transmitting the incident light. Next comes the signal plate, which consists of a thin transparent film of electrically-conductive graphite. A potential of approximately 40 volts is applied to this layer. The third member of the sandwich is the target which is a thin film of photoconductive material.

- An important part of the camera is the vacuum tube typically measuring up to 15 cm in length by up to 3 cm in diameter. It can be surrounded by coils for focusing and deflecting the electron beam. Alternatively, deflection electrodes called deflectrons can be shaped on the inside walls of the vacuum tube.
- At the opposite end of the tube is the cathode. Through indirect heating, electrons are boiled from the cathode surface and accelerated by up to 900 volts towards the anode. The anode extends across the end of the tube as a fine wire mesh which allows most of the electron beam to pass through it. Once they pass through they decelerate to hit the signal plate. The electron beam is focused to a tiny point using the focusing coils which extend almost the full length of the tube. The focused electron beam can be deflected both vertically and horizontally by the application of suitable voltages to the deflectrons.
- Video camera targets are generally scanned in a raster pattern which is similar to that used in broadcast TV. Here an interlaced raster scan is used to scan 625 horizontal lines of the target at a rate of 25 images (called frames) each second, for instance, to generate the perception of continuous imaging.
- Light falling on the photoconductive target changes its conductivity in proportion to the light intensity and these changes are read by the scanning electron beam. The electric current generated is conveyed via the transparent conductive film to an external circuit where a video voltage can be developed.
- The choice of photoconductive target has an important impact on the performance of the video camera. A general-purpose target material used in the vidicon camera is antimony trisulphide (Sb2S3), while other materials such as lead oxide (PbO), as in the Plumbicon, and cadmium selenide (CdSe), as in the Chalnicon, can be used for more specialised applications.
- Semiconductor Video Camera

- These cameras are typically based on charged coupled device (CCD) technology and consist of a semiconductor chip that is sensitive to light. The chip contains many thousands of electronic sensors (e.g. photodiodes) each of which reacts to light and generates a signal that varies depending on the amount of light each receives. CCDs have been developed primarily for the domestic video camera market and the result is a compact, lightweight camera with improved performance relative to photoconductive cameras. Array sizes of up to 2,028 x 2,028 and greater are possible.
- The device differs critically from the PUT camera in that a scanning electron beam in an evacuated environment is not required. The signal is read from each sensor element at the appropriate rate by purely electronic means using what are called electronic shift registers - see Figure 4.13. Sensor signals are first transferred into the vertical shift registers and then shifted one line at a time to a horizontal shift register to be read out to form a video signal. The analogy to a bucket brigade has often been used to describe this process.
- Note that CCD cameras have also found application in the direct viewing of intensifying screens in radiographic applications[12].

- The camera control unit provides the link between the camera and the display monitor. It houses an oscillator circuit that controls the electron beam deflections of a PUT camera, for instance, or the interline transfer in CCD cameras and synchronises the recorded image with that displayed on a video monitor or stored in a computer memory. Synchronization is generally achieved using sync pulses inserted during the blanking interval of each video line and frame - see Figure 4.14. The main amplifier in the control unit adjusts the gain of the video amplifier so that the video signal range, usually 0 to 1 V, can be fully utilised. This function is called Automatic Gain Control (AGC).
- Note that the video image is generally rectangular in shape. The ratio of the width of the image to its height is called the Aspect Ratio and is typically 4:3. This is not ideally suited to medical imaging where the video camera is viewing the circular image produced by an XII.
Automatic Brightness Control
[edit | edit source]- The range of body part thicknesses and composition encountered in fluoroscopic imaging is quite large. In a barium upper GI study, for example, moving from screening the neck to screening the stomach will substantially increase X-ray attenuation along the way and result in darker images unless the exposure factors and/or the gain of the video camera are adjusted to compensate. Adjustment of the exposure factors is generally referred to as Automatic Brightness Control (ABC), while camera-based adjustment is provided by the AGC, as described above. ABC is used to keep the brightness of the displayed image at a constant level during examinations. It involves the adjustment of the kV and mA automatically depending on the part of the anatomy being examined. This can be achieved using a small photosensor at the XII output, for instance, which monitors the central portion of intensified images and feeds a signal back to the generator to adjust the kV, the mA (or both) accordingly.
- ABC systems are generally designed to operate between minimum (e.g. 70 kV) and maximum (e.g. 120 kV) kilovoltages. The minimum kV can be used at the start of an exposure sequence, for instance, to prevent low energy X-rays exposing the patient unnecessary, and is then increased automatically so that a pre-determined image brightness level is reached. The tube current (mA) can also be adjusted automatically during this process. Such mA adjustment within the kV range of the ABC is limited by the power rating of the XRT. When the power limit is reached, in fluoroscopy of the lateral abdomen or at steep-angled cardiac projections, for instance, further adjustment of exposure factors is no longer possible and the AGC circuitry can come into play to maintain image brightness. However, images with increased electronic noise generally result.
- The actual kV and mA settings used by ABC systems dictate the contrast displayed in fluoroscopic images as well as the dose to the patient. A High Dose ABC mode can be used which lowers the kV and boosts the mA so that image contrast can be improved at the same image brightness, while a Low Dose mode increases the kV and lowers the mA to effect a similar outcome. A third intermediate mode can also be selected on many systems. The heat capacity of the XRT imposes the power limit, which is controlled by the product, (kV x mA), the ABC system automatically applies. This is dictated by the thickness and composition of the anatomy being screened. When this product reaches the power limit, in the case of a very large patient, for example, the ABC generally maintains constant kV and mA settings. Hence the need for additional control provided by the camera's AGC. In addition, the AGC control of image brightness happens almost instantaneously whereas the HV circuitry can take about a second or so to respond to any ABC detected illuminance changes. The AGC is therefore also of use during this adaptation period so as to maintain a constant brightness in displayed images.
Radiation Dose Management
[edit | edit source]An indicator of the radiation exposure required to generate a CR or DR image is provided on many systems. This indicator can be called the Sensitivity Index (SI), the Log Median (LgM), the Exposure Index (EI) or similar parameter and can be used to gauge the adequacy of an exposure. Note that these parameters are generally referenced to exposures generated under specific conditions, e.g. X-ray energy, beam filtration etc., and therefore can be regarded only as a crude indicator of patient dose.
Dose-Area Product (DAP) - see the discussion below - records can be used to review exposure trends over time in the clinical environment[13]. One of the aims here is to reduce the phenomenon of Exposure Creep, where exposures slowly increase over time in the pursuit of images of excellent quality, for example. Another aim here can be to review exposure measurements relative to Diagnostic Reference Levels (DRLs).
Retake analysis can also be combined with such exposure reviews so that, for instance, a team of X-ray personnel can work collectively to improve performance. Reasons for retake radiographs can be catalogued into radiographic exposure errors, including those resulting from patient movement, when too long an exposure is used, for example, and radiographic positioning errors[14].
Skin Injury
[edit | edit source]- There has been considerable interest in recent years in reducing fluoroscopic doses following numerous reports of epilation and skin injuries to patients from prolonged interventional procedures[15]. Regulatory agencies throughout the world have responded to ICRP deliberations[16] and have issued recommendations to the effect that the person responsible for the apparatus:
- Needs to establish standard operating procedures and clinical protocols.
- Should know typical radiation dose rates for the specific fluoroscopic system.
- Must assess the impact of each procedure's protocol on the potential for radiation injury to patients.
- Must modify the protocol to limit the dose.
- Should enlist a qualified health physicist to provide assistance in developing and optimising dose minimisation techniques.
- Should give consideration to rotating the tube and the image intensifier through 180° during prolonged neuroradiological procedures.
- Should give consideration to carrying out those cardiology procedures where multiple stenting is necessary over a period of weeks to fractionate the radiation dose.
- Should give due consideration when purchasing new equipment to features offered by the manufacturer that may aid in reducing the patient dose.
- Skin injury has been found to be sensitive to factors such as previous high dose exposure, medication, connective tissue disease and diabetes mellitus. A review of hair and skin effects is given in Balter et al. (2010)[17]. Single-site skin doses in interventional radiology above 2 Gy, for example, have been found to cause erythema and epilation and higher doses to cause permanent skin damage.
- Mechanisms of patient dose reduction which have been developed include:
- Pulsed Fluoroscopy: this is a feature which uses short pulses of radiation of variable duration and frequency (Fig. 3.1). Such pulsing can be generated by switching the mA in the HV generator or by controlling the electron beam of the XRT, as in the Grid-Controlled XRT. Following each exposure pulse, the image is stored in image memory and displayed continuously until the next pulse to give a contiguous visual effect. Significant dose rate reductions are achievable using this approach, although dose reductions are not directly proportional to the decreased pulse rate due to built in adjustments to maintain diagnostic quality. Also, stroboscopic artifact may result when imaging fast moving objects such as the heart.
- Additional Filtration: the addition of a thin Cu filter (0.1 - 0.3 mm) at the output of the X-ray tube can generate substantial dose reductions without a detrimental impact on image quality. A refinement to this approach is the Region of Interest (ROI) filter which provides little filtration to the central region of the field of view and substantial filtration in peripheral regions - the rationale being that high image quality is required in the centre of the field and noisier image data of lower contrast is tolerable outside of this region for providing general anatomical information only. This latter mechanism has also been referred to as the X-ray fovea.
- Collimation: Since the use of conventional rectangular collimators used with XII-based fluoroscopy systems (which generate circular images) results in unused exposure, some modern systems use circular collimators. These typically have the capability of automatically responding to changes in source-to-image distance and in the electronic zoom selection used in the XII. A complex collimator assembly, based on adjustable multileaf absorbers, results and can include robotic control. Another feature in this regard is referred to as radiation-free collimator positioning and involves storing an image in computer memory, stopping the exposure and adjusting the collimator controls so that the computer generates a graphics display of the collimated region.
- Digital Image Storage: the fact that images are stored in computer memory (see the following chapter) allows the possibility of using features such as Last-Image-Hold (LIH), where the most recently acquired image is displayed continuously without irradiating the patient, Reference Imaging, where a previously acquired image is displayed on a second video monitor for comparison purposes, Image Browsing, where multiple images acquired previously can be displayed, and Fluoroscopic Loop, where an imaging sequence can be continuously replayed for closer inspection.
- Automatic Brightness Control (ABC) can be used in conjunction with exposure pulse control and additional filtration to generate what is called Automatic Dose Rate Control (ADRC)[18]. Here, different filters can be selected automatically for insertion into the X-ray beam depending on the particular exposure factors encountered when screening commences. For example, some ADRC systems can generate the selection of:
- a kilovoltage which remains constant during the imaging sequence,
- an mA pulse height and width which maintains image brightness, and
- the automatic insertion of Cu filters of different thicknesses,
- depending of the thickness and composition of the body part being examined. Such systems can be used with four selectable copper filters, for instance, of thickness 0.2, 0.3, 0.6 and 0.9 mm depending on patient thickness. Since absorbed doses are greater for larger patient thicknesses, because higher exposure factors are required to acquire images of adequate brightness, a filter thickness is chosen that hardens the X-ray beam appropriately and reduces patient dose. This is referred to as Spectral Filtering. The ADRC system can cause the HV generator to select a constant kV, depending on the Cu filter thickness, and vary the mA pulse height depending on the anatomy. For example, it may select 60 kV with a 0.9 mm Cu filter for a thin body part, such as the foot, and 80 kV with a 0.3 Cu filter for a body part greater than 20 cm thick, with the mA adjusted for each exposure by the generation of pulses of the necessary intensity.
- Most fluoroscopy systems also feature an audible alert which sounds after a 'beam-on' time of five minutes. The accumulated exposure time is generally displayed in real-time on the image display, along with the kV and mA - and dose rate readings when a Dose-Area Product meter (see below) is installed.
Staff Dose
[edit | edit source]- Three sources of exposure arise for staff when operating radiography and fluoroscopy equipment: the primary beam used to expose the patient, leakage radiation from the XRT and scattered radiation from the patient. Lead aprons can be worn and distance exploited to minimise the impact of leakage and scattered radiation in instances where staff are required to remain in an X-ray room or operating theatre during exposures. Note however that lead aprons only attenuate X-rays by ~90-95%, depending on their lead equivalence. These aprons are generally made from lead-impregnated vinyl, are equivalent to 0.25-0.5 mm of lead and weigh about 5 kg. Lighter aprons with similar attenuation can be made from composites, such as tungsten and tin, and may be of value to staff during long interventional procedures. Aprons of 0.5 mm lead equivalence should be used by staff who remain in close proximity to the patient during exposures. The safer style is the wrap-around apron, in comparison to backless designs. From a practical perspective, lead aprons should always be stored vertically on racks since folding them can introduce cracks which reduce their effectiveness. In addition, they should be radiographed at least annually to check for any such signs of wear and tear.
- In addition, the number of staff in the immediate vicinity of the patient can be kept to a minimum and warnings given when an exposure is impending. Ideally, staff should be behind a shielded operator's console area during an exposure. The design of X-ray rooms is such that, in general, adequate shielding and distance ensures that doses to any person in the room, behind the console or, indeed, external to the room can be optimised.
- In some interventional cases, the interventionist may find it necessary to have their hands in the primary beam for parts of the procedure. Such repeated exposure over a number of years may potentially lead eventually to radiation dermatitis of the hands. Dose optimisation in such circumstances can be achieved by arranging the imaging system so that the hands are kept on the beam exit side of the patient. For example, if the XRT is positioned under the patient then the hands manipulating the catheter should be on top of the patient.

- It should also be noted that the use of over-couch XRTs in fluoroscopy can lead to significantly greater staff doses than systems which use under-couch XRTs - see Figure 4.15. Increased radiation scattered from the patient and the lack of shielding provided by the structure of the patient table are the cause. An increased incidence of lens injuries has been found, for instance, in radiologists who have used over-couch systems without protective screens[19]. Note, however, that this over-couch argument may not always be valid when inverted C-arms are used to assist with hand surgery[20].
- The elevated dose rates to the trunk and head of the staff member can be noted in panel (a) of the figure. Radiation dose to the legs of interventionists can also be significant even with the use of under-couch XRTs - and with C-arm systems[21][22].

- The use of C-arm and similar arrangements in cardiac catheterisation laboratories, operating theatres and angiography suites can introduce additional hazards - see Figure 4.16. These arise because of the ergonomics associated with the use of lead shielding devices - which are intended for the minimisation of scatter and leakage at the interventionist's position. It is therefore quite possible for their thyroid and eye lens, for instance, to receive substantial doses. Thyroid shields and lead spectacles can be worn and adjustable lead glass shields used for dose optimisation purposes in these circumstances[23][24]. Shielding equivalent to 0.25 mm of lead is generally required with glasses also having side protection. In addition, interventionists can wear a second dosemeter at the level of their neck to monitor the dose to their thyroid and eyes. Note that radiation-associated posterior lens changes have been observed in the eyes of cardiac Cath Lab staff - both medical and clinical, most not wearing lead glasses - with an incidence significantly greater than an unexposed control group[25] and that a study of cataract incidence has been launched for a large sample of interventional cardiologists[26].
- The location of the interventionist during the procedure has a large influence on their hand dose[27]. A ring dosemeter on the finger proximal to the XRT can be used to monitor such doses. Lead gloves are not generally worn for ergonomic reasons and also because the additional attenuation generated when shielded hands are in the beam will increase the automatically controlled exposure factors. Note that particular additional optimisation techniques can be required in specialities such as urology[28] and endovascular surgery[29].
- Targeted education for all users of specialised X-ray apparatus has been identified as a key optimisation strategy[30] and has been implemented successfully in, for example, computed tomography[31].
Patient Dose
[edit | edit source]- Good imaging geometry should be used to optimise patient protection in radiography, fluoroscopy and fluorography. In most situations the image receptor should therefore be moved to the maximum distance from the XRT and the patient placed as close to the image receptor as possible. In other words, the patient should ideally be moved to the image receptor and not the other way around. Some fluoroscopy systems can do this automatically so as to maintain a narrow air gap between the patient and image receptor before exposures.
- Effective doses to patients from fluoroscopy procedures are considerably higher, as might be expected, than in General Radiography - see the table below. The higher doses result from both fluoroscopy-screening exposures and multiple fluorography exposures. Notice that strongly attenuating parts of the body which contain a number of radio-sensitivite organs, such as the abdomen, generate the larger doses in the table.
| Procedure | Effective Dose (mSv) |
|---|---|
| Cerebral Arteriography | 2.5
|
| Nephrostomy | 5.5
|
| Barium Meal | 8.2
|
| Renal Arteriorography | 10.3
|
| Barium Enema | 11.7
|
| Biliary Stent Placement | 12.5
|
| Enteroclysis | 14.0
|
- More recent and extensive data is provided in Mettler et al. (2008)[34]. Note that specific patient shielding can be of benefit to patient dose in different types of X-ray examinations, e.g. thyroid protection in cerebral angiography[35].
- It can be noted from the table that all doses are higher than that of the average annual background dose (2.4 mSv). From this perspective, the dose from a Cerebral Arteriogram is equivalent to about 1 year of background exposure - its so-called Background Equivalent Radiation Time (BERT). Note however that considerable variations can exist in patient dosimetric survey data, by a factor of 10 or more, due to patient anatomical differences and the quality of the imaging technology, for example. Note also that variations by a factor of over 100 occur in background exposure in different parts of the world. It is apparent that the BERT is therefore only a very approximate indicator of relative dose.
- The higher doses in the above table, and higher still in extended interventional procedures, have prompted the use of dosimetry equipment to routinely monitor parameters such as the Dose-Area Product (DAP) and the Peak Skin Dose. DAP (also called the Kerma-Area Product) is a measure of the total energy exiting an XRT and is generally measured (in Gy cm2) at a location in the beam close to the collimators. The parameter has the advantage that it is independent of source-to-skin distance, as was described previously, and can be used to estimate stochastic risk from a procedure. The Peak Skin Dose is a useful indicator of the likelihood of deterministic effects. Such measurements can be also be used to establish a dose scale to assist interventional staff in radiation dose management[36].
| Modality | Examination | Average Effective Dose (mSv) |
|---|---|---|
| General radiography | Extremities | 0.001 |
| Knee | 0.005 | |
| Shoulder | 0.01 | |
| Chest (PA) | 0.02 | |
| Chest (PA + Lateral) | 0.1 | |
| Skull | 0.1 | |
| Cervical Spine | 0.2 | |
| Mammography | 0.04 | |
| Pelvis | 0.6 | |
| Abdomen | 0.7 | |
| Hip | 0.7 | |
| Thoracis Spine | 1 | |
| Lumbar Spine | 1.5 | |
| Intravenous Urography | 3 | |
| DEXA | without CT | 0.001 |
| with CT | 0.04 | |
| Fluoroscopy | ERCP | 4 |
| Small Bowel series | 5 | |
| Upper GI series | 6 | |
| Ba Enema | 8 | |
| Computed Tomography | Head | 2 |
| Neck | 3 | |
| Calcium Scoring | 3 | |
| Pelvis | 6 | |
| Spine | 6 | |
| Chest | 7 | |
| Abdomen | 8 | |
| Virtual Colonoscopy | 10 | |
| CTPA | 15 | |
| Three-Phase Liver | 15 | |
| Coronary Angiography | 16 | |
| Interventional Radiography | Head/Neck Angiography | 5 |
| Thoracic Angiograpghy | 5 | |
| Coronary Angiography | 7 | |
| Abdominal Angiography | 12 | |
| CTPA, Stent or RF Ablation | 15 | |
| Pelvic Vein Embolization | 60 | |
| TIPS Placement | 70 | |
| Dental Radiography | Intra-oral Radiography | 0.005 |
| Panoramic Radiography | 0.01 | |
| Dental CT | 0.2 |
A visual interpretation of this data is shown below:
- Implementation of dose monitoring is critical for dose optimization in digital radiography. Staff guidelines as previously developed for film/screen radiography, should include appropriate collimation, source-to-image distance (SID), focal spot size and patient positioning. This information can also enable effective doses to be subsequently estimated, in situations where DAP meters, for instance, are not available. The use of image quality indicators for different examinations is an additional step in assisting clinical management of the balance between dose and image quality[37].
- Results of a comprehensive catalogue of dose surveys from 1980-2007 are summarised in Figure 4.17. It can be seen that effective dose in General Radiography vary by a factor of >1,000, in the range 0.001 to 3 mSv, depending on the area of anatomy irradiated. Radiography/fluoroscopy procedures, as used for barium studies, can be seen to generate higher doses (4-8 mSv) as do CT studies (2-16 mSv). Interventional radiology is seen to generate still higher doses (5-70 mSv). CT and interventional exposures can therefore be considered at relatively high dose examinations and therefore require greater attention from a dose management perspective. However, it should be appreciated that these values contain large uncertainties, which can range by factors of 5-10 or more. Furthermore, the average figures are themselves age- and sex-averaged and are also subject to a variation of ±40% when referred to an individual patient, depending on variables which include the patient's weight, orientation, X-ray exposure factors and imaging technology used. It is therefore apparent that they should be considered as indicative values only which should never be used as a substitute for the dose to an individual patient from a particular examination. Their use here is solely to provide a comparison for dose management purposes.
- On a final point, note that patient dosimetry in general radiography, fluoroscopy, mammography and computed tomography is reviewed in Huda et al. (2008)[38].
References
[edit | edit source]- ↑ Neitzel U, 2005. Status and prospects of digital detector technology for CR and DR. Radiat Prot Dosimetry, 114:32-8.
- ↑ Cowen AR, Davies AG & Kengyelics SM, 2007. Advances in computed radiography systems and their physical imaging characteristics. Clin Radiol, 62:1132-41.
- ↑ Schaefer-Prokop CM, De Boo DW, Uffmann M & Prokop M, 2009. DR and CR: Recent advances in technology. Eur J Radiol, 72:194-201.
- ↑ Cesar LJ, Schueler BA, Zink FE, Daly TR, Taubel JP & Jorgenson LL, 2001. Artefacts found in computed radiography. Br J Radiol, 74:195-202.
- ↑ Cowen AR, Davies AG & Sivananthan MU, 2008. The design and imaging characteristics of dynamic, solid-state, flat-panel x-ray image detectors for digital fluoroscopy and fluorography. Clin Radiol, 63:1073-85.
- ↑ Cowen AR, Kengyelics SM & Davies AG, 2008. Solid-state, flat-panel, digital radiography detectors and their physical imaging characteristics. Clin Radiol, 63:487-98.
- ↑ Spahn M, 2005. Flat detectors and their clinical applications. Eur Radiol, 15:1934-47.
- ↑ Sato K, Nariyuki F, Kuwabara T, Fukui S, Okada Y, Nabeta T, Hosoi Y, Enomoto J, Sasao M & Seguchi Y, 2010. Development of CALNEO, an indirect-conversion digital radiography system with high-conversion efficiency. Fujifilm R&D, 55:10-3
- ↑ Rivetti S, Lanconelli N, Bertolini M, Borasi G, Golinelli P, Acchiappati D & Gallo E, 2009. Physical and psychophysical characterization of a novel clinical system for digital mammography. Med Phys, 36:5139-48
- ↑ Balter S, 2019. Fluoroscopic technology from 1895 to 2019 drivers: Physics and physiology. Medical Physics International, 7:111-40.
- ↑ Seibert JA, 2006. Flat-panel detectors: How much better are they? Pediatr Radiol, 36 Suppl 2:173-81.
- ↑ Yaffe MJ & Rowlands JA, 1997. X-ray detectors for digital radiography. Phys Med Biol, 42:1-39.
- ↑ Schuncke A & Neitzel U, 2005. Retrospective patient dose analysis of a digital radiography system in routine clinical use. Radiat Prot Dosimetry, 114:131-4.
- ↑ Prieto C, Vano E, Ten JI, Fernandez JM, Iñiguez AI, Arevalo N, Litcheva A, Crespo E, Floriano A & Martinez D, 2009. Image retake analysis in digital radiography using DICOM header information. J Digit Imaging, 22:393-9.
- ↑ Shope TS, 1996. Radiation-induced skin injuries from fluoroscopy. Radiographics, 16:1195-9.
- ↑ Valentin J, 2000. Avoidance of radiation injuries from medical interventional procedures. Ann ICRP, 30:7-67.
- ↑ Balter S, Hopewell JW, Miller DL, Wagner LK & Zelefsky MJ, 2010. Fluoroscopically guided interventional procedures: A review of radiation effects on patients' skin and hair. Radiology, 254:326-41.
- ↑ Lin PJ, 2007. The operation logic of automatic dose control of fluoroscopy system in conjunction with spectral shaping filters. Med Phys, 34:3169-72.
- ↑ Vañó E, González L, Beneytez F & Moreno F, 1998. Lens injuries induced by occupational exposure in non-optimized interventional radiology laboratories. Br J Radiol, 71:728-33.
- ↑ Tremains MR, Georgiadis GM & Dennis MJ, 2001. Radiation exposure with use of the inverted-c-arm technique in upper-extremity surgery. J Bone Joint Surg Am, 83-A:674-8.
- ↑ Whitby M & Martin CJ, 2003. Radiation doses to the legs of radiologists performing interventional procedures: Are they a cause for concern? Br J Radiol, 76:321-7.
- ↑ Shortt CP, Al-Hashimi H, Malone L & Lee MJ, 2007. Staff radiation doses to the lower extremities in interventional radiology. Cardiovasc Intervent Radiol, 30:1206-9.
- ↑ Shortt CP, Fanning NF, Malone L, Thornton J, Brennan P & Lee MJ, 2007. Thyroid dose during neurointerventional procedures: Does lead shielding reduce the dose? Cardiovasc Intervent Radiol, 30:922-7.
- ↑ Thornton RH, Dauer LT, Altamirano JP, Alvarado KJ, St Germain J & Solomon SB, 2010. Comparing strategies for operator eye protection in the interventional radiology suite. J Vasc Interv Radiol, 21:1703-7.
- ↑ Vano E, Kleiman NJ, Duran A, Rehani MM, Echeverri D & Cabrera M, 2010. Radiation cataract risk in interventional cardiology personnel. Radiat Res, 174:490-5.
- ↑ Jacob S, Michel M, Spaulding C, Boveda S, Bar O, Brézin AP, Streho M, Maccia C, Scanff P, Laurier D & Bernier MO, 2010. Occupational cataracts and lens opacities in interventional cardiology (O'CLOC study): Are X-Rays involved? Radiation-induced cataracts and lens opacities. BMC Public Health, 10:537.
- ↑ Martin CJ, 2009. A review of radiology staff doses and dose monitoring requirements. Radiat Prot Dosimetry, 136:140-57.
- ↑ Hellawell GO, Mutch SJ, Thevendran G, Wells E & Morgan RJ, 2005. Radiation exposure and the urologist: What are the risks? J Urol, 174:948-52.
- ↑ Walsh SR, Cousins C, Tang TY, Gaunt ME & Boyle JR, 2010. Ionizing radiation in endovascular interventions. J Endovasc Ther, 15:680-7.
- ↑ Le Heron J, Padovani R, Smith I & Czarwinski R, 2010. Radiation protection of medical staff. Eur J Radiol. 2010 Oct;76(1):20-3.
- ↑ Wallace AB, Goergen SK, Schick D, Soblusky T & Jolley D, 2010. Multidetector CT dose: Clinical practice improvement strategies from a successful optimization program. J Am Coll Radiol, 7:614-24.
- ↑ Ruiz-Cruces R, Perez-Martinez M, Martin-Palanca, Flores A, Cristófol J, Martínez-Morillo M & Díez de los Ríos A, 1997. Patient dose in radiologically guided interventional vascular procedures: Conventional versus digital systems. Radiology, 205:385-93.
- ↑ Ruiz-Cruces R, Ruiz F, Pérez-Martínez M, López J, Tort Ausina I & de los Ríos AD, 2000. Patient dose from barium procedures. Br J Radiol, 73:752-61.
- ↑ a b Mettler FA Jr, Huda W, Yoshizumi TT & Mahesh M, 2008. Effective doses in radiology and diagnostic nuclear medicine: A catalog. Radiology, 248:254-63.
- ↑ Shortt CP, Malone L, Thornton J, Brennan P & Lee MJ, 2008. Radiation protection to the eye and thyroid during diagnostic cerebral angiography: A phantom study. J Med Imaging Radiat Oncol, 52:365-9.
- ↑ Davies AG, Cowen AR, Kengyelics SM, Moore J, Pepper C, Cowan C & Sivanathan MU, 2006. X-ray dose reduction in fluoroscopically guided electro-physiology procedures. Pacing Clin Electrophysiol, 29:262-71.
- ↑ Uffmann M & Schaefer-Prokop C, 2009. Digital radiography: The balance between image quality and required radiation dose. Eur J Radiol, 72:202-8.
- ↑ Huda W, Nickoloff EL & Boone JM, 2008. Overview of patient dosimetry in diagnostic radiology in the USA for the past 50 years. Med Phys, 35:5713-28.

