Structural Biochemistry/Tylenol
Overview
Tylenol, also known as acetaminophen, is a popular pain reliever. This drug is famous for relieving headaches as well as reducing fever. Tylenol is not considered an NSAID, anti-inflammatory. It does not do much in halting inflammation.
Precautions
Be careful if your joints are aching from intense exercise. Tylenol would probably not be a good choice, compared to aspirin or Aleve. This is because the aching of joints is due to inflammation.
Discovery of Tylenol
[edit | edit source]The main ingredient in Tylenol which is acetaminophen was actually first discovered in Europe before aspirin even became a consumer product. However, it was never studied closely for its possible pharmaceutical uses until Robert L. McNeil of McNeil Laboratories. After an informal conversation with Raymond Conklin, who was vice president of the Institute for the Study of Analgesic and Sedative Drugs, at an American Pharmaceutical Manufacturers Association meeting, this compound N-acetyl P-aminophenol was brought to Neil’s attention and his work began. One of the reasons for the great success of acetaminophen when compared to aspirin is the lack of stomach aches that arise from acetaminophen. The FDA approved the drug in June of 1955 and it was introduced as Elixer Tylenol.
Absorption
Oral acetaminophen is rapidly and almost completely absorbed from the GI primarily in the small intestine. This absorption process occurs by passive transport. The relative bioavailability ranges from 85% to 98%.
Distribution
Acetaminophen appears to be distributed throughout most body fluids except fat. The volume distribution of acetaminophen is 0.95 L/kg. A small fraction of acetaminophen is bound to plasma proteins and binding is only slightly increased in plasma concentrations associated with overdose. Sulfate and glucuronide metabolites do not bind to plasma proteins even at relatively high concentrations.
Metabolism
Acetaminophen is primarily metabolized in the liver and involves three principal separate pathways 1. conjugation with glucuronide 2. conjugation with sulfate 3.oxidation via the cytochrome
Excretion
Acetaminophen is eliminated from the body primarily by formation of glucuronide and sulfate conjugates.
Mechanism of Tylenol Tylenol, acetaminophen, belongs to a class of painkillers known as non-opioid analgesics. Non-opioid analgesics work by inhibiting an enzyme known as cyclooxygenase (COX). COX is a catalyst for the conversion of a fatty acid contained in cell walls, arachidonic acid, to a substance known as prostaglandins. Prostaglandins produce pain, inflammation and fever. It causes pain and inflammation after cell injury at the site of the injury in the peripheral nervous system. They elevate body temperature by affecting the hypothalamus. By blocking COX and the subsequent production of prostaglandins in the central and peripheral nervous systems, Tylenol reduces both fever and inflammation. Tylenol differs from the other non-opioids in that it does not block COX in the peripheral nervous system that great. It appears to reduce pain primarily in the central nervous system by more than one mechanism, possibly in part by inhibiting a form of COX known as COX-3. Therefore, it is considered to be a weak analgesic and does not possess anti-inflammatory properties.
Similarity of Structure Tylenol and Aspirin
The first similarity between the two molecule is their benzene skeleton. Both these molecules have reactive oxygen and reactive hydrogens attach to the benzene ring that contribute to their molecule acidity. Aspirin has a carboxylic acid while Tylenol contains a phenol. The acidity of both molecules contributes to similar physiological activities, relieving pain.
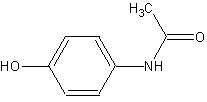
-Tylenol- Top Image

-Aspirin - Bottom Image
Side Effects
[edit | edit source]Some people might present allergic reactions after taking tylenol. It is recommended to see a physician if the person presents one or more of the following symptoms:
- hives
- difficulty breathing
- swelling of the face, lips, tongue or throat
- nausea
- upset stomach
- itching
- loss of appetite
- dark urine
- clay-colored stools
- jaundice (yellow skin or eyes)
Incompatibility with other drugs
[edit | edit source]Tylenol could react violently if taken with some other medications. Medications that could possibly react with tylenol to produce severe side effects are:
- Antibiotics
- birth control pills/hormone replacement medication
- blood pressure medication
- cancer medication
- cholesterol lowering medication
- arthritis medication (including gold injections)
- HIV/AIDS medication
- psychiatric disorder medication
- seizure medications
Acetaminophen induces liver necrosis Although acetaminophen is safe for therapeutic doses, higher dosage can contribute to liver necrosis. Acetaminophen poisoning accounts for almost half of all cases of acute liver failure in the US and the UK. This results from the following steps: 1. Acetaminophen is metabolically activated by cytochrome 450 into a reactive specie which depletes glutathione, an antioxidant that prevents damages to important cellular components caused by reactive oxygen species such as free radicals and peroxides. 2. Loss of glutathione with an increased formation of reactive oxygen and nitrogen species in liver cells undergoes necrotic changes; 3. Due to increased oxidative stress, mitochondrial permeability changes. 4. Mitochondrial permeability changes from the additional oxidative stress which leads to loss of mitochondrial membrane potential, and the loss of the ability of the mitochondria to synthesize ATP. 5. Loss of ATP will not enable the liver cell to function anymore leading to necrosis. There are inflammatory mediators such as certain cytokines and chemokines that can modify the toxicity. Some have been shown to alter oxidative stress. In addition, existing data support the involvement of cytokines, chemokines, and growth factors in the initiation of regenerative processes of the liver. As a result, pay careful attention to how much acetaminophen one is taking and never exceed the maximum daily dose (4,000 mg or eight Tylenol extra strength pills in a 24-hour period). If one needs more pain relief, consult with one’s doctor about incorporating other pain relief strategies or by switching to a different type of painkiller. Acetaminophen is also available in a variety of medications, from over-the-counter cough and cold medicines to prescription strength painkillers. Confirm the ingredients of all drugs to make sure the maximum dosage is not exceeded as over dosage will induce liver necrosis. If one has liver disease or drink alcohol heavily, avoid acetaminophen completely! If one regularly takes the drug, watch for signs of liver damage, which include dark urine, pale stools, right-upper abdominal pain, and a yellowish tinge in the whites of the eyes.
Addition Dangers of Tylenol Diphenhydramine, an ingredient in Tylenol PM, is an antihistamine that also has sedative properties to help patients fall asleep. However, if people take too much diphenhydramine due to excessive use of Tylenol PM or by taking diphenhydramine in addition to the amount found in Tylenol PM, overdose can occur. This overdose can cause confusion, dry mouth, fatigue, muscle weakness, dizziness and chest congestion. In high doses, diphenhydramine can cause hallucinations and seizures.
COX-2and Acetaminophen
From a structural standpoint, it is hard to see how acetaminophen would inhibit the COX site of COX because it lacks a carboxylic acid moiety for interaction with arginine 120. Early work provided a mechanistic approach to see why acetaminophen would have part of the therapeutic activities possessed by NSAIDs but lack anti-inflammatory and anticoagulatory activity. Acetaminophen exerts its effect on a subtype of COX located in the brain. The finding of 2 forms of COX validated the notion of COX subtypes, but further investigation of COX-2 failed to find it to be significantly inhibited by acetaminophen.
Reference
[edit | edit source]http://www.drugs.com/tylenol.html [1] [2] [3] [4] [5] [6] [7]
"Robert L. McNeil, Jr." Homepage of the Chemical Heritage Foundation. N.p., n.d. Web. 21 Nov. 2012. <http://www.chemheritage.org/discover/online-resources/chemistry-in-history/themes/pharmaceuticals/relieving-symptoms/mcneil.aspx>.
- ↑ http://www.chemistryexplained.com/A-Ar/Acetaminophen.html
- ↑ http://www.ncbi.nlm.nih.gov/pubmed/20020268
- ↑ http://tuftsjournal.tufts.edu/2008/04/professor/01/
- ↑ http://dmd.aspetjournals.org/content/31/12/1499.full
- ↑ http://www.tylenolprofessional.com/pharmacology.html
- ↑ http://cid.oxfordjournals.org/content/31/Supplement_5/S211.full
- ↑ http://news.consumerreports.org/health/2011/11/repeatedly-taking-too-much-tylenol-can-be-dangerous.html