Structural Biochemistry/Protein function/Regulation
Protein regulation is essential for biological balance. Too much or too little of any proteinreactivity can cause severe biological damage.
Specific Diseases
[edit | edit source]Alzheimer's Disease
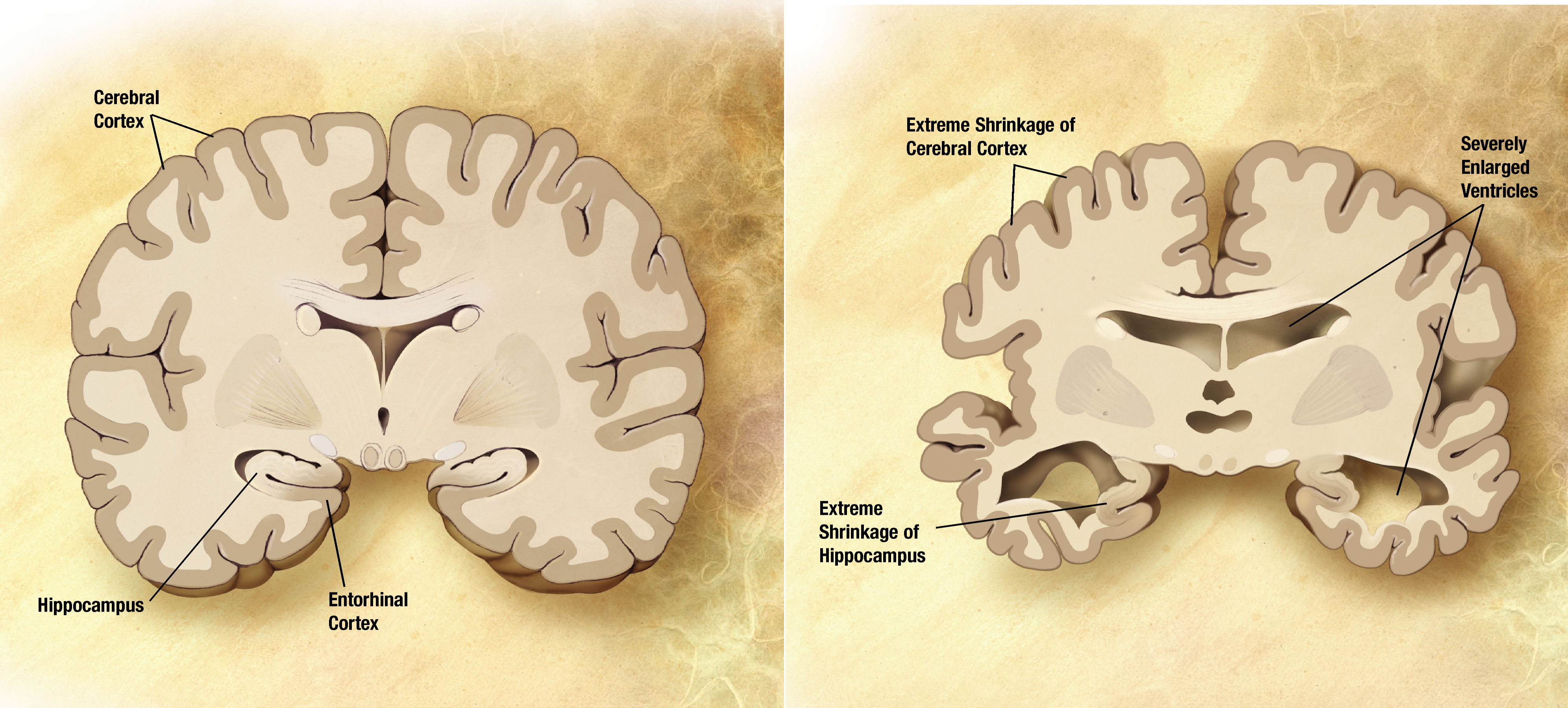
[edit | edit source]Alzheimer's patients have "plaques" in their brains, which are essentially large chunks of a certain protein believed to contribute to neuronal death. It is also a dementia that gets worse over time. There is no cure for Alzheimer's disease. As you can see in the picture, someone who has Alzheimer's has extreme loss in the different functions of the brain.
Alzheimer's patients have this protein's regulation pathway disturbed, causing it to be overly expressed. Protein regulation is also referred to as Enzyme Regulation. Furthermore, the study of these protein regulation pathways have lead to much growth in the creation of medicinal and pharmaceutical products.
Hunter Syndrome
[edit | edit source]Hunter syndrome is a genetic disease in which mucopolysaccharides do not degrade accurately. As a result, mucopolysaccharides will accumulate inside the body. The main cause of this accumulation is the absence of iduronate sulfatase enzyme. Some of the signs for recognition of the syndrome are big heads and different facial characteristics. The syndrome can be found out with urine test. However, this test is not trusted. The study of fibroblasts that extract from body’s skin is more effective. The gene that contributes to the cause of Hunter syndrome is residing on the X-recessive chromosome. Since males only have one X chromosome, the chance that males inherit this syndrome is higher than that of females.
The problem with Hunter syndrome is how the body is unable to break down mucopolysaccharides, which make up proteoglycan that is part of the extracellular matrix. As a consequence, the adding up of mucopolysaccharides becomes an obstacle for other cells in the body to carry out their jobs. This incident may lead to significant effects that can harm the body. For instance, some early side effects of Hunter syndrome can be the normal sickness such as cold and runny nose.
Hunter syndrome results in a certain effects upon the body. Thus, people who inherit the syndrome tend to have common characteristics. The more extreme consequences of Hunter syndrome include mental retardation, heart problem, joint stiffness, etc. Bone marrow replacement was proven to help expanding the life span of Hunter syndrome patients. Unfortunately, it does not solve the problem of mental retardation. Elaprase, a lysosomal enzyme iduronate sulfatase that can be made by recombinant DNA technique, has demonstrated to be an effective cure for Hunter syndrome through the replace of enzyme. Nevertheless, elaprase is indeed very expensive.
Hurler Syndrome
[edit | edit source]Hurler Syndrome is an inherited disease and is caused by a recessive mutation (both parents would need to have passed down the trait). Historically, it was thought to be caused by the excessive synthesis of 2 mucopolysaccharides: dermatan sulfate and heparan sulfate. Some scientists believed the excessive synthesis of the 2 molecules to be caused by a faulty regulation pathway. Elizabeth Neufeld tested this hypothesis and found it to be false; she found the cause of the disorder to be the inadequate degradation of the 2 sugars. While normal cells leveled off production after a certain point, cells affected by the mutation continued production past normal levels.
Correction of this disease is easily possible in vitro (and works to an extent in vivo.) The addition of healthy cells in the same culture as mutated cells in vitro caused normal levels of dermatan sulfate and heparan sulfate to be created. The normal cells excrete a corrective factor/enzyme in the medium which is taken up by the mutated cells. This enzyme is crucial in the degradation of the 2 mucopolysaccharides; furthermore, very little of it is necessary to fully correct the mutated cells. There are many problems with using α-L-Iduronidase as treatment in vivo; the main issue being that various tissues respond at various degrees to the medication. Most importantly, the central nervous system does not uptake any of the intravenously injected enzyme because of the blood-brain barrier. On top of this issue, a significant number of people with this disease have neurological diseases that need to uptake this enzyme somehow.
α-L-Iduronidase was found to be the key enzyme in restoring proper degradation of dermatan sulfate and heparan sulfate. It was found though that α-L-Iduronidase from some cells was not corrective. Research showed that the carbohydrate mannose 6-phosphate was responsible for proper uptake of the enzyme; a mutation in the structure of it caused the α-L-Iduronidase product to not be taken up properly by cells affected by Hurler Syndrome.
Sanfilippo Syndrome
[edit | edit source]Sanfilippo Syndrome is within a set of neurodegenerative diseases called tauopathies (the most common of which is Alzheimer's Disease). Although there are 4 subtypes of Sanfilippo Syndrome, they are all characterized by reduced degradation of heparan sulfate (see Hurler Syndrome section) due to reduced levels of a lysosomal enzyme.
It was found in a mouse model (MPS IIIB) that there were significantly increased levels of the protein lysozyme; increased levels of this disease were found to cause the creation of hyperphosphorylated tau which is found in the brains of Alzheimer's patients and patients with other tauopathies. Significant research is being done in Alzheimer's disease which may carry over to Sanfilippo Syndrome as well due to their similarities.
1. 4 different subtypes: Each Sanfilippo subtype is caused by the deficiency of each specific enzyme: heparin N-sulfatase for MPS-III A, N-acetyl-alpha-D-glucosaminidase for MPS-III B, acetyl-CoA: alpha-glucosaminide acetyltransferase for MPS-III C, and N-acetylglucosamine-G-sulfate sulfatase for MPS-III D. Among these four subtypes, Sanfilippo syndrome type A is the most prevalent (60%), followed by B (30%), D (5%), and C (6%). In total, 47% of all cases of mucopolysaccharidosis diagnosed is related with Sanfilippo disease.
2. Mortality/ Morbidity: Patients with Sanfilippo syndrome tend to develop Central Nervous System degeneration and usually end up at a vegetative state. They usually die before the age of 20 due to cardiopulmonary arrest because of airway obstruction or infection in the pulmonary pathway. Among these 4 subtypes, MPS-III A is the most severe one due to early death in patients (usually during their teenage years). Sanfilippo syndrome has an equal effect on both males and females as well as on different races since its main cause is the inheritance in an autosomal recessive pattern which has no relations with the sex chromosomes.
3. Diagnosis and History: In terms of diagnosis, these four subtypes are not indistinguishable clinically; therefore, the only determining factor to identify each specific subtype is the different genes that are responsible for that subtype. Usually, affected individuals show no symptoms and develop normally during the first two years of their lives. Onset usually takes place between the age of 2 and 6. Developmental delays in infancy may be shown in some of them. Growth might be slowed down at the age of 3 (e.g. short stature). Patients might also become hyperactive and behave aggressively and destructively. Besides disturbing the sleep pattern in patients, this syndrome also interferes severely into the mental development of affected patients – speech impairment, hearing loss, etc. At the same time, patients might show shortened attention spans and find it challenging to concentrate and to be able to perform academic tasks at schools. By the age of 10, patients’ daily activities and movements are severely limited. They often are in need of wheelchairs to accommodate them and might even have swallowing difficulties and seizures. Some other physical symptoms might also be shown such as carious teeth, enlarged liver and spleen, diarrhea (which is believed is due to lysosomal glycosaminoglycans (GAG) storage in the neurons of the myenteric plexus3.) Respiratory compromise can occur and is related to airway obstruction due to anatomical changes, excessive thick secretions and neurologic impairment. Upper respiratory tract infections and sinopulmonary disease are common.
4. Work-up: In order to diagnose patients with Sanfilippo Syndrome, specific enzymatic assays in cultured skin fibroblasts and in peripheral blood leukocytes are used (e.g. enzymatic cell analysis). One indicating sign for this syndrome is the increase in the level of heparan sulfate in the urinary secretion. Thus a total quantitative or a fractionation test are carried by performing either electrophoresis or chromatography with the purpose of measuring how much Glycosaminoglycans (GAGs) is in the urine. Due to the higher level of GAGs in newborns and infants, age-specific controls and fractionation must be included to accurately quantify the level of GAGs. Imaging studies can also be used to look for changes in brain structure since the spectrum of skeletal changes can be seen in patients with Sanfilippo syndrome.
5. Treatment: Currently, there is no available treatment for the real cause of Sanfilippo syndrome. Bone marrow transplantation and Enzyme replacement therapy only work for patients with mucopolysaccharidosis I, II, and VI (not III). However, some promising therapies are making their ways to be FDA-approved.
References
[edit | edit source]- Defendi, Germaine, [1]
- Neufeld, Elizabeth F, "From serendipity to therapy."
- [2]
- [3]