Biomedical Engineering Theory And Practice/Bioelectric phenomena(Application)
Electrocardiography - for the heart
[edit | edit source]
Electrocardiography (EKG or ECG[1] ) is a quick, simple, painless recording that checks for problems with the electrical activity of your heart. An ECG is for measuring the heart’s electrical conduction system.[2] It picks up electrical impulses generated by the polarization and depolarization of cardiac tissue and translates into a waveform. The waveform is then used to measure the rate and regularity of heartbeats, including the size and position of the chambers, the presence of any damage to the heart, and the effects of drugs or devices for controlling the heart, like a pacemaker.
Leads
[edit | edit source]An electrocardiogram also is called an EKG or ECG. Sometimes the test is called a 12-lead EKG or 12-lead ECG. This is as the heart's electrical activity is monitored from the leads of 12 different places on the body at the same time[3].
Usually, an EKG machine consists of electrode wires with gel patches, a computer which converts the signal into a waveform and adjusts for electrical artifact, a screen to view the cardiac rhythm in real time (many incorporate a 6 second delay), a printer to produce a hard copy of the waveform. The data is collected from the patient using a total of 10 electrodes[4].
Limb Leads (Bipolar)
[edit | edit source]Leads I, II, III together form the vectors of an equilateral triangle (0, 60, 120 degrees). This is called Einthoven's triangle. Einthoven found that the sum of current of Lead I + Lead III = Lead II[5]. The limb leads measure cardiac depolarization in the frontal (coronal) plane.
| Lead | Placement of electrode |
|---|---|
| Lead I | The negative electrode attaches to the right arm(RA). The positive electrode attaches to the left arm(LA).The axis is 0 degrees. |
| Lead II | The negative electrode attaches to the right arm(RA).The positive electrode attaches to the left leg(LL). The axis is +60 degrees. |
| Lead III | The negative electrode attaches to the left arm(LA).The positive electrode attaches to the left leg(LL). The axis is 120 degrees. |
Augmented Limb Leads (Unipolar)
[edit | edit source]There are 3 augmented limb leads. These leads provide additional vector views of cardiac depolarization in the frontal plane. Unlike leads I, II, III, the augmented leads need a central negative terminal. This virtual "electrode" is calculated by the electromyogram computer to measure vectors originating roughly at the center of the heart.
| Lead | Placement of electrode |
|---|---|
| avL | The negative electrode is the central termininal. The positive electrode attaches to the right arm(RA). The axis is -150 degrees. |
| avR | The negative electrode is the central termininal.The positive electrode attaches to the left arm(LA).The axis is -30 degrees. |
| avF | The negative electrode is the central termininal.The positive electrode is connected to the left leg(LL). The axis is +90 degrees. |
Chest Leads (Unipolar:Precordial lead)
[edit | edit source]Precordial leads consist of the other 6 leads and electrodes connected during an EKG. These leads measure depolarization in the axial plane using a central terminal. These provide essential information used in localizing ischemic or infarcted tissue during a cardiac event.
| Lead | Placement of electrode |
|---|---|
| V1 | +120 degrees |
| V2 | +90 degrees |
| V3 | +75 degrees |
| V4 | +60 degrees |
| V5 | +30 degrees |
| V6 | 0 degrees |

ECG waves and intervals
[edit | edit source]
ECG Pattern and Diseases
[edit | edit source]Most ECGs are used to monitor diseases or research purposes on human hearts. Some pathological patterns can be seen on electrocardiography as the following tables[6]:
Electroencephalography - for the brain
[edit | edit source]
Brain cells communicate with each other by producing tiny electrical signals, called impulses[7].
An EEG records the oscillations of brain electric potentials recorded from perhaps 20 to 256 electrodes attached to the human scalp.The recorded signals are transmitted to an EEG system composed of amplifiers, filters, and paper chart or computer monitor. The test is done for 20~40 mins by an EEG technologist in the doctor's office or at a hospital or laboratory[8].
The EEG is used to evaluate various brain disorders.In the case of epilepsy, seizure activity will appear as rapid spiking waves on the EEG.[9] Patients with lesions of the brain from tumors or stroke, may have unusually slow EEG waves, depending on the size and the location of the lesion.[10] but this use has decreased with the advent of high-resolution anatomical imaging techniques such as MRI and computed tomography. Despite limited spatial resolution, EEG is still valuable tool for research and diagnosis, especially in the case of millisecond-range temporal resolution (not possible with CT or MRI). The test can also be useful to diagnose other brain disorders like as Alzheimer's disease, certain psychoses, and a sleep disorder called narcolepsy. The EEG may also be good at testing the overall electrical activity of the brain, such as drug intoxication,trauma or extent of brain damage in comatose patients). The EEG may also be used to monitor blood flow in the brain during surgical procedures.
-
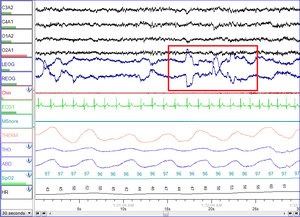
Placement of electrodes to determine EEG, EOG, and EMG
-
An EEG recording at Dalhousie University
EEG 10-20 Lead System
[edit | edit source]The 10/20 system or International 10/20 system is an internationally recognized method to describe the location of scalp electrodes.

This system is based on the relationship between the location of an electrode and the underlying area of cerebral cortex. The "10" and "20" refer to the fact that the actual distances between adjacent electrodes are either 10% or 20% of the total front–back or right–left distance of the skull.[11][12][13]
Each site has a letter to identify the lobe and a number to identify the hemisphere location.The letters F, T, C, P and O define frontal, temporal, central, parietal, and occipital lobes respectively.There are no central lobes. The "C" letter is only for identification purposes. A "z" (zero) refers to an electrode placed on the midline. Even numbers (2,4,6,8) means electrode positions on the right hemisphere respectively.On the other hand, odd numbers (1,3,5,7) means those on the left hemisphere. The letter codes A, Pg and Fp identify the earlobes, nasopharyngeal and frontal polar sites respectively.
Two anatomical landmarks are used for the essential positioning of the electrodes: First, the nasion is the point between the forehead and the nose. Second, the inion is the lowest point of the skull from the back of the head and is normally indicated by a prominent bump.
When recording a more detailed EEG with more electrodes, extra electrodes are added using the 10% division, which fills in intermediate sites halfway between those of the existing 10–20 system. These new electrodes named according to the Modified Combinatorial Nomenclature (MCN). This MCN system uses 1, 3, 5, 7, 9 for the left hemisphere which refers to 10%, 20%, 30%, 40%, 50% of the inion-to-nasion distance respectively. The introduction of extra letter codes helps the naming of intermediate electrode sites. In this case, These new letter codes do not refer to an area on the underlying cerebral cortex. The new letter codes for intermediate sites are: AF – intermediate between Fp and F, FC – between F and C, FT – between F and T, CP – between C and P, TP – between T and P, PO – between P and O. In addition, the MCN system renames four points of the 10–20 system — T3, T4, T5 and T6 — as T7, T8, P7 and P8 respectively.This higher-resolution nomenclature has been suggested and called the "5% system" or the "10–5 system".[14]
Different types of normal brain waves
[edit | edit source]An EEG measures patterns of brain activity. The basic waveforms are the alpha, beta, theta, and delta rhythms. During an EEG, generally about 100 pages or computer screens of activity are examined.The basic waveforms needs special attentions but brief bursts of energy and responses to stimuli, such as light, are also recorded.
Electrocorticography - from the cerebral cortex
[edit | edit source]Electrocorticography (ECoG), or intracranial EEG (iEEG), is invasive electroencephalography with the needle-like electrodes placed directly on the exposed surface of the brain to record electrical activity from the cerebral cortex[15]. ECoG may be performed in the operating room during surgery (intraoperative ECoG) or outside of surgery (extraoperative ECoG) as a craniotomy (a surgical incision into the skull) need to implant the electrode grid.
Electrophysiological Basis
[edit | edit source]Method
[edit | edit source]Application
[edit | edit source]
Electromyography - for the muscle
[edit | edit source]
Electromyography (EMG) is a diagnostic procedure for evaluating and recording the electrical activity produced by skeletal muscles and the nerve cells that control them (motor neurons).[16]The electrical source is the muscle membrane potential of about -90 mV.[17] Measured EMG potentials range between less than 50μV and up to 20 to 30 mV, up to the muscle under observation. Typical periodical rate of muscle motor unit firing is about 7–20 Hz, according to the size of the muscle (eye muscles versus seat (gluteal) muscles), previous axonal damage and other factors. Damage to motor units is about 450 ~ 780 mV[16].
Electrooculography - for the eyes
[edit | edit source]
An electro-oculogram (EOG) is often performed after the ERG. The EOG records the polarization potential or cornealretinal potential (CRP), which is the resting potentials between the front(cornea) and Bruch’s membrane at the back of the human eye. The potential makes a dipole field with the cornea about 5 millivolts positive in comparison to the back of the eye, in a normally illuminated room. Although the EOG is from the pigment epithelium of the retina, the light rise of the potential needs both a normal pigment epithelium and normal mid-retinal function.
EOG are performed with the same lateral canthus electrodes as for the ERG and with additional electrodes placed on the medial canthus of the eyes on the nose. The common/ground electrode remains on the forehead[18].
Electroretinography - for the retina
[edit | edit source]
Electroretinography(ERG) tests the electrical responses of various cells in the retina which is the lining at the back of the eye including the photoreceptors (rods and cones), inner retinal cells (bipolar and amacrine cells), and the ganglion cells[19]. ERG can be carried out alone or with the cortical visually evoked potential (VEP). VEPs are usually performed to measure the function of the optic nerve which is the vision part of the brain[20].
ERG response to fast bright flashes (50 or 100ms in duration) is recorded with an extracellular electrode positioned either on the cornea, in the vitreous or at different levels inside the retina. and processed using an digital system.
The recording conditions may be various in order to test the overall health of the retina and the function of specific light receptors (different retinal cells); ie the cones and rods are for day and night vision respectively.
Optimal responses are recorded through contact lens type electrodes. Other types of electrodes are proper for clinical recordings. These include filament, fibre and gold foil type electrodes. Useful results can also be done with surface electrodes on lower eye-lids. All except the latter need a local anaesthetic eye-drop to allow the electrodes comfortably. Dilation of the pupil is also needed to obtain standardized responses.

Bright flashes would bring ERGs including an a-wave (initial negative deflection) followed by a b-wave (positive deflection). The a-wave is produced by the photoreceptors, while A mixture of cells including photoreceptors, bipolar, amacrine, and Muller cells or Muller glia cause the other waves.[21]
Clinically used mainly by ophthalmologists and optometrists, the electroretinogram (ERG) is suitable for the diagnosis of diverse retinal diseases.[22].
- Arteriosclerosis with damage to the retina
- Achromatopsia
- Cone dystrophy
- Choroideremia
- Congenital night blindness
- Congenital retinoschisis (splitting of the retinal layers)
- Giant cell arteritis
- Medications (chloroquine, hydroxychloroquine)
- Mucopolysaccharidosis
- Retinal detachment
- Rod-cone dystrophy (retinitis pigmentosa)
- Trauma
- Vitamin A deficiency
Audiology - for the auditory system
[edit | edit source]Audiology is a field of science thatin identifies, diagnoses, treats and monitors disorders of the auditory and vestibular system parts of the ear. Audiologist are the health professional who treat those with hearing loss and proactively prevent related damage. According to the Audiology and Speech-Language Pathology Act, 1991 (ASLPA),the scope of audiology in Ontario,Canada is as follows: "The practice of audiology is the assessment of auditory function and the treatment and prevention of auditory dysfunction to develop, maintain, rehabilitate or augment auditory and communicative functions. Audiologists are concerned with the prevention, identification, assessment, treatment and (re)habilitation of hearing difficulties in children and adults. Audiologists also provide education and counseling services for people experiencing hearing difficulties and vestibular problems, such as dizziness and tinnitus[23]. Audiologist works in hospitals,public health units,community Health Centres,schools,private practice,hearing aid manufacturers and so on[24]. An Audiologist usually graduates with one of the qualifications among MSc(Audiology), Au.D., STI, PhD, or ScD up to the program, and country standard.
Further Leading
[edit | edit source]International Society for Clinical Electrophysiology of Vision
Practise
[edit | edit source]1. Understand placement of electrode in each application.
2. Understand wave patterns in each applications
Reference
[edit | edit source]- ↑ Abbreviated from the German word Elektro-Kardiographie
- ↑ Walraven, G. (2011). Basic arrhythmias (7th ed.), pp. 1–11
- ↑ National heart, lung and blood institute, other names for electrocardiogram
- ↑ Cardiovascular physiology concept, Richarde E.Klabundle
- ↑ "Electrocardiogram explanation image". Retrieved 28 February 2014.
- ↑ http://www.ecglibrary.com/ecghome.html
- ↑ MedlinePlus,EEG
- ↑ Niedermeyer E. and da Silva F.L. (2004). Electroencephalography: Basic Principles, Clinical Applications, and Related Fields. Lippincot Williams & Wilkins. ISBN 0-7817-5126-8.
- ↑ Atlas of EEG & Seizure Semiology. B. Abou-Khalil; Musilus, K.E.; Elsevier, 2006.
- ↑ "EEG".
- ↑ system manual
- ↑ system manual
- ↑ American Electroencephalographic Society. Guidelines for standard electrode position nomenclature. J Clin Neurophysiol, 8:200-202, 1991.
- ↑ Robert Oostenveld and Peter Praamstra (2001). "The five percent electrode system for high-resolution EEG and ERP measurements". Clinical Neurophysiology. 112: 713–719. doi:10.1016/S1388-2457(00)00527-7.
{{cite journal}}: CS1 maint: uses authors parameter (link) - ↑ free dictionary,Electrocorticography
- ↑ a b Kamen, Gary. Electromyographic Kinesiology. In Robertson, DGE et al. Research Methods in Biomechanics. Champaign, IL: Human Kinetics Publ., 2004.
- ↑ Nigg B.M., & Herzog W., 1999. Biomechanics of the Musculo-Skeletal system. Wiley. Page:349.
- ↑ Michael F. Marmoret al,ISCEV standard for clinical electro-oculography Ophthalmol (2011) 122:1–7
- ↑ Michael Bach et al. ISCEV standard for clinical pattern electroretinography(PERG): 2012 update;Doc Ophthalmol (2013) 126:1–7
- ↑ Great Ormond Street hospital for children, Visual evoked potential (VEP) and electroretinogram (ERG) tests
- ↑ waves Webvision at University of Utah
- ↑ Electroretinography, U.S. National Library of Medicine, 11 April 2005 (accessed 19 January 2007)
- ↑ http://www.e-laws.gov.on.ca/html/statutes/english/elaws_statutes_91a19_e.htm
- ↑ http://www.caslpo.com/AboutTheProfessions/Audiologists/tabid/64/Default.aspx







