Metabolomics/Hormones/Corticosteroids
Back to Previous Chapter: Metabolites
Next chapter: Analytical Methods
Go to: Mineralocorticoids
Go back to: Somatostatin
Introduction
[edit | edit source]Corticosteroids, or Corticoids are hormones that are produced in the adrenal cortex. This family can be broken down into two main groups; mineralocorticoids and glucocorticoids. Included in these groups are hormones such as Cortisol and Prednisone. The male and female sex hormones, testosterone and estrogen are also produced in small amounts in the adrenal gland. A reduced ability to produce these steroids can lead to disorders such as Addison’s disease.
The adrenal gland can be broken down into three layers. The outermost layer is the zona glomerulosa, which produces mineralocorticoids. The middle layer is the zona fasciculate which produces the glucocorticoids and the innermost layer is the zona reticularis which produces weak androgens (precursors to testosterone and estrogen).
Corticosteroid drugs are usually administered through inhalers for asthma related problems, and topologically for skin related irritations.
Table of corticosteroid medications
[edit | edit source]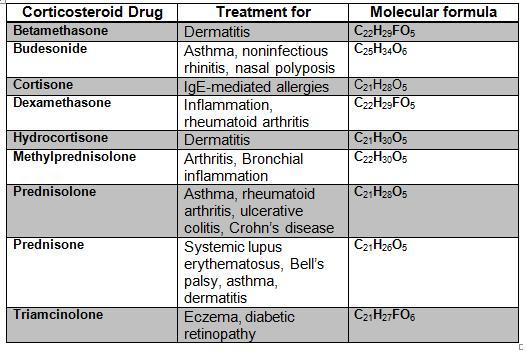
Formation of Corticosteroids
[edit | edit source]All steroids originate from the same starting molecule, cholesterol. In the case of the formation of the corticosteroid Aldosterone, cholesterol is first converted into Pregnenolone by way of a side chain cleavage. Pregnenolone is then converted into Progesterone which in turn in converted into 11-deoxycorticosterone. The remaining reactions take place in the outer layer of the adrenal gland.

11-deoxycorticosterone is converted into Corticosterone which is converted into 18-hydroxy-corticosterone which is oxidized, turning it into the final product, Aldosterone. The human body will synthesize this steroid to conserve sodium and secrete potassium in the kidneys, which causes retention of water and increase blood pressure. This is a key molecule in the regulation of ion re-absorption and blood pressure.
Disorders related to Corticosteroids
[edit | edit source]There are a few disorders related to the adrenal gland and the production of corticosteroids. One of these diseases is called Addison’s disease, also known as chronic adrenal disorder. People who suffer from this cannot produce sufficient steroid hormones form their adrenal gland and must take supplement hormones orally. Some symptoms of Addison’s disease are; sweating, change in mood and personality, joint and muscle pain. Signs that someone may have the disorder are puffiness and darkening of the skin, most noticeable on scars, lips and pressure points. This occurs because the hormone that causes increased melanin production, melanocyte stimulating hormone (MSH) shares the same precursor molecule as adrenocorticotropic hormone (ACTH). When ACTH levels are increased due to medication MSH levels increase as well. A prominent figure in American history that had Addison’s disease was John F. Kennedy, it is thought to have caused some of his appearance and mood issues late in his presidency.
Inhaled Corticosteroids in Asthma Management
[edit | edit source]This article stated that all available inhalable corticosteroids have the ability to work as advertised at an equipotent dose. Inhalers are currently the most effective treatment to asthma on the market, most of them only requiring low (80μl-1200μL) doses a day. Inhalers can range from once daily doses to multiple doses daily. This article when into detail about the obstacles that drug developers have to overcome to produce an effective treatment, such as taking advantage of corticosteroids that are only activated once they reach the lower respiratory tract (Ciclesonide). This ensures that the maximum amount of the drug is deposited in the lungs where it is needed, and not lost in the mouth and throat. The article also included adverse effects that may occur while taking the steroids, such as Adrenocortical suppression, bone degradation and glaucoma. As with most drugs being overweight and smoking increase adverse effects. Long acting beta agonists have been found to make the medications more effective and have been suggested for patients to use in tandem.
The article can be found at; http://www.rcjournal.com/contents/05.08/05.08.0625.pdf
Addison’s Disease
[edit | edit source]This article, entitled Addison’s Disease focuses on the corticosteroid treatment of the adrenal gland insufficiency. The article reviews the clinical presentation and common manifestations of the disease, followed by the diagnostic criteria and management. The management portion of the paper was the most revealing in terms of corticosteroids. This portion of the paper focused on biochemical testing used to diagnose the illness, including plasma cortisol, morning serum cortisol, and cortisol response to ACTH; to rule out the illness, potassium and plasma renin activity are taken. Normal treatment of this disease includes replacing hormones, specifically corticosteroids that the adrenal insufficiency has not provided. These corticosteroids include intravenous or oral hydrocortisone, or prednisone for a longer half-life. The hydrocortisone is a much safer option, not adversely affecting the immune system like prednisone, although the prednisone is a more effective treatment it can only be used for emergency situations, not for long term treatment. The only other option for replacement of these corticosteroids is oral fludrocortisone which is quite potent requiring a dose of only 0.05 to 0.3 mg/day this hormone replaces the mineralocorticoids whereas the other two medicines replace glucocorticoids.
The article can be found at: http://www.sciencedirect.com/science?_ob=ArticleURL&_udi=B6T5G-4KBG8HY7&_user=47004&_coverDate=082F312F2006&_rdoc=1&_fmt=&_orig=search&_sort=d&view=c&_acct=C000005018&_version=1&_urlVersion=0&_userid=47004&md5=cf2542b40a4bdd827b755b543fb46aa9
What are topical Corticosteroids?
[edit | edit source]As its name suggests, the website provided below pertains to information about topical corticosteroids. This site gives a general overview of the science behind corticosteroids and their uses. Topical corticosteroids are used to suppress inflammation of the skin and come in ointments and creams like the widely known Hydrocortisone. In many cases, commercial topical corticosteroids include antiseptics and antibiotics to combat potential microbial threats as well as heal inflammation. The site divides topical corticosteroids into four strengths: mild, moderate, potent and very potent. When seeing a doctor about issues with skin irritation, the lowest strength is usually prescribed first and is increased until the problem is solved. This is to avoid any potential side effects that may occur with the stronger varieties.
This website can be found at: http://www.netdoctor.co.uk/skin_hair/eczema_corticosteroids_003762.htm
Glucocorticoids
[edit | edit source]Carbenoxolone (CBX) has been discovered to inhibit cortisol and prednisolone production via 11ß-hydroxysteroid dehydrogenase (11ß-HSD)1 inhibition. Decreasing glucocorticoid (GC) levels has been determined to be a requirement for GC-induced lipolysis.
Previous studies have concluded that CBX increases levels of urinary free cortisol (UFF) and decreases levels of urinary free cortisone (UFE). This is reflects upon the inhibition of renal 11ß-HSD2. A decrease in tetrahydrometabolites of cortisol (THF + 5 THF) and an increase in tetrahydrocortisone (THE) levels were also discovered to occur.
11ß-HSD1 and -2 are capable of interconverting cortisol and cortisone, as well as prednisone and prednisolone. The activities of these enzymes were also able to be inhibited by glycyrrhetinic acid (GE), because of their similar enzyme kinetics. Dexamethasone has been established as an 11ß-HSD1 substrate, and could act as a competitive inhibitor with cortisone.
Experimental GC induction might be counteracted by decreased mRNA expression from CBX action. There have been observed decreases in cortisol production after CBX treatment, which supports the assumption that 11ß-HSD2 inhibition increases the half-lives of cortisol and prednisolone. Increasing these half-lives would result in an increase in overall production of cortisol and prednisolone.
During interstitial fluid experiments, single doses of CBX were proven to have the same impact as a 72hr treatment as the limited availability of cortisol. Activity inhibition had been marked in microdialysate samples. Single doses of CBX were discovered to inhibit the production of cortisol in the microdialysate. This is in agreement with the local inhibition in adipose, and is further supported by the capability of measuring CBX within adipose tissue and interstitial fluid. CBX concentrations were much higher in serum than in adipose and were in excess of interstitial fluid GC concentrations. As a result, competitive inhibition seems entirely possible.
11ß-HSD1 has been proven to regulate GC promoted lipolysis. Adipose tissue microdialysis data revealed that peak glycerol release was reduced by CBX, which indicated an inhibition of GC-mediated lipolysis. Overall, useful biomarkers of 11ß-HSD1 inhibition include urinary GC/MS, prednisolone, and interstitial adipose cortisol production. In addition, limited GC availability to human adipose tissue via 11ß-HSD1 inhibition also results in lipolysis attenuation.
Link to article:
http://jcem.endojournals.org/cgi/content/full/92/3/857
Corticosteroids
[edit | edit source]This website is dedicated to corticosteroids, their application, background, various types, and side effects. The site is based around about.com so it is based on a certain topic, in this case arthritis. Corticosteroids are a well known very effective treatment for rheumatoid arthritis and this site is based on information focused around that fact. This page starts with describing what they are, some examples of corticosteroids, information about cortisol, how corticosteroids work, what conditions do they treat, and how they are given. For just some basic background and applications of corticosteroids this is an excellent resource, for a more in-depth look at the hormones, where they are formed and what they do in the human body a more scholarly article should be sought. Most websites readily available online are geared more to the layman but journal articles are where the real information is.
The website can be found at: http://arthritis.about.com/cs/steroids/a/corticosteroids.htm
Glossary of terms
[edit | edit source]Pharmacodynamic: study of the biochemical and physiological effects of drugs on the body or on microorganisms or parasites within or on the body and the mechanisms of drug action and the relationship between drug concentration and effect.
Pharmacokinetic: The study of absorption, distribution, biotransformation and excretion of medicines, including the timelines of these processes.
Equitherapeutic: Administration of medication at equal therapeutic value .
DPI: dry-powder inhaler.
ICS: inhaled corticosteroids.
Dysphonia: the medical term for hoarseness or other phonation disorders.
MDI: metered-dose inhaler
Comorbidities: The presence of one or more disorders (or diseases) in addition to a primary disease or disorder
LABA: long acting β agonists
Neutrophilic inflammation: Inflammation of granulocyte containing cells, in this case contained in the lungs.
Languor: lack of energy or vitality; sluggishness.
Monograph: a highly detailed and thoroughly documented study or paper written about a limited area of a subject or field of inquiry.
Melanocyte: a cell producing and containing melanin.
Orthostatic: pertaining to an upright standing posture; "orthostatic hypotension".
Azotemia: the accumulation of abnormally large amounts of nitrogenous waste products in the blood, as in uremic poisoning.
Mucocutaneous: of or relating to the mucous membranes and skin.
Vitiligo: a skin disorder characterized by smooth, white patches on various parts of the body, caused by the loss of the natural pigment.
Supraphysiologic: Indicating a dose that is larger or more potent than would occur naturally, as of a chemical agent that mimics a hormone.
Diurnal: chiefly active during the daytime.
Cushingoid: resembling Cushing’s disease especially in the face.
Hirsutism: excessive hairiness, esp. in women.