Medical Physiology/Gastrointestinal Physiology/Motility
Motility
[edit | edit source]Ingestion of food is controlled by hunger and appetite. In health the body controls the rate at which ingested food moves through the GI system, so that digestion and absorption are optimised. The first residue from a meal will pass through the GI system in 7–10 hours, but some may take up to 5 or six days to pass through.
Smooth muscle Characteristics
[edit | edit source]Smooth, also called involuntary or un-striated muscle is usually found in the walls of hollow organs, and have many unique characteristics. Contraction of these cells is dependent on the influx of Ca++ ions. In the gut three types of contraction are seen:
- Tonic sustained contractions, such as occur in sphincters
- Peristaltic contractions
- Segmental contractions
By a variety of these contractions, food and chyme is moved through the bowel.
Mechanics of contraction
[edit | edit source]Smooth or un-striated muscle cells contract by altering their shape. They contain numerous actin-myosin bundles. Some of the actin Strands attach to the cell, they are all anchored to dense bodies in the cytoplasm of the cell. On activation the actin strands slide over the myosin causing shortening of the actin-myosin bundle:
This causes overall bulging and shortening of the cell:
Physiology of contraction
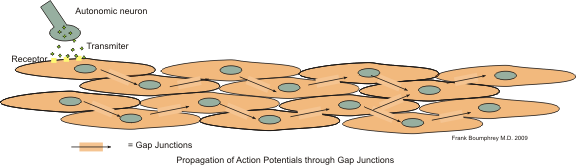
[edit | edit source]Muscle cells in the intestine communicate with each other through gap junctions, causing a series of function syncitial units. Thus an action potential in one cell will spread to other cells in the unit.
Contraction can be initiated by action potentials or by chemicals and hormones. Contraction caused by the former are known as myogenic potentials, the later is known as pharmacomechanical coupling. Some of the smooth muscle cells have a spontaneous cycle of depolarization, and these are known as pacemaker cells. They are said to have slow wave depolarization. When the level of depolarization reaches a certain threshold, an action potential is triggered. The strength of contraction depends on the number of action potential triggered.
Some pace maker cells will trigger an action potential with every slow wave, others with only occasional slow waves. The following illustration shows the electrical pattern of slow waves with occasional action potentials and 'pacemaker' potentials where every wave generates action potentials. Each slow cycle lasts 7–12 seconds.
The following illustration demonstrates the effect on two agents, A & B on Muscle Tension in pharmacomechanical coupling. Note that there is no change in the membrane potential.
Action Potentials cause an influx of Ca++ ions which release more Ca++ from the sarcoplasmic reticulum. Because the supply of Calcium in the sarcoplasmic reticulum is limited it must be replaced by Calium ions from outside the cell. The membrane potential is restored by an efflux of Na+ ions.
Tonic sustained contractions
[edit | edit source]One characteristic of smooth muscle cells is their ability to maintained tonic sustained contractions. Muscle that has this is said to have or maintain tone. This allows sphincters to maintain their tonicity, and to open by 'relaxing' their tone. As an example of the tone in the gut, the length of the small intestine is about 24 ft. in death, but is only half this length in life due to the tone in the longitudinal muscle bundles.
Peristalsis & Segmental Contractions
[edit | edit source]Segmental contractions are used for mixing food or chyme. The circular muscles in adjacent segments of the intestine undergo alternate contraction and relaxation. The effect of this is not to move food along the lumen, but to churn it and mix it, especially with the digestive juices. Segmental contractions also bring the chyme into contact with the epithelial cells for absorption.
Peristaltic contractions move food and chyme down the lumen of the bowel. Circular muscles contract behind a bolus of food, the muscles in front of the bolus relax and this wave of contraction proceeds down the bowel propelling the bolus of food forward.
Motility through out the GI System
[edit | edit source]The passage of food through the gut, its conversion to chyme, and finally feces is all under involuntary control. Only the first part - ingestion and swallowing, and the last part - defecation are under voluntary control.
Mastication
[edit | edit source]Chewing is extremely important part of the digestive process especially for fruits and vegetables as these have indigestible cellulose coats which must be physically broken down. Also digestive enzymes only work on the surfaces of food particles, so the smaller the particle, the mre efficient the digestive process.
Swallowing
[edit | edit source]Swallowing is coordinated by the swallowing or deglutition center located in the upper medullar and lower pons. Impulses are carried by the Trigeminal, Glossopharangeal, and Vagus nerves.
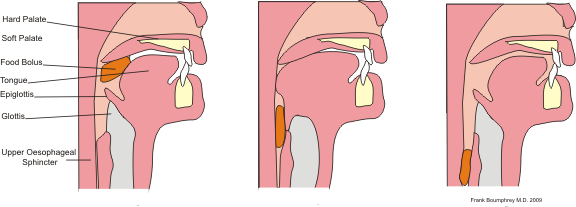
- The tongue pushes a bolus of food against the soft palate triggering the swallowing reflex.
- The soft palate is pulled upwards preventing reflux of food into the nasal cavities
- The vocal cords are strongly approximated
- The larynx is pulled upwards, closing the epiglottis, preventing food entering into the trachea. The esophageal sphincter relaxes.
- The muscular wall of the pharynx contracts beginning superiorly, pushing the food into the esophagus
- Peristaltic waves assisted by gravity push the food down the esophagus.
Esophagus
[edit | edit source]Food is carried down the esaphagus by peristaltic contractions. If these are insufficient to move all the food, stronger secondary peristaltic waves develop. These are initiated by both the myenteric plexus and centrally.
The muscle at the lower end of the esophagus thickens and is called the lower esophageal sphincter. This is usually tonically contracted, but relaxes when the peristaltic wave reaches it, allowing passage of food into the stomach.
Stomach
[edit | edit source]Food entering the stomach passes into the fundus of the stomach where it is stored. Weak peristaltic waves, known as mixing waves originate in the upper stomach and pass down to the antrum. These waves become stronger as they approach the antrum, and as they push the food against a closed pylorus they also act as mixing waves. Food in the antrum of the stomach is also thoroughly mixed with segmental contractions. The mixed fluid contents are called chyme, and small amounts of this are pushed through the pylorus into the duodenum with the stronger peristaltic contractions.
Control of Stomach Emptying
[edit | edit source]The rate of emptying of the stomach is controlled by various factors originating in the duodenum and stomach, of which the duodenal factors are the most important.
Gastric factors include increased volume of food in the stomach and stretching of the stomach wall. The hormone Gastrin also appears to promote stomach emptying.
Duodenal factors serve mainly to inhibit entering, thereby ensuring that the small intestine is not overwhelmed by a sudden influx of acidic chyme. They include nervous reflexes and hormones. The nerve reflexes are transmitted both by the enteric nervous system and through extrinsic nerves via the pre-vertebral sympathetic ganglia.
Factors that inhibit emptying include:
- Distension of the duodenum
- The degree of acidity of the duodenal chyme
- The osmolarity of the chyme
- Irritation of the duodenum
The reflexes are particularly sensitive to acidity and irritation which case rapid inhibition of stomach entering.
Hormones that inhibit emptying include cholecystokinin, secretin, and Gastric Inhibitory Peptide (GIP). Secretin is secreted in response to acidity in the duodenum, Cholecystokinin and GIP in response to the presence of fats in the chyme.
All these factors ensure that the rate of stomach emptying is limited to what the small intestine can process.
Small bowel
[edit | edit source]In the small intestine mixing with segmental contractions continues and the food is slowly passed through the intestine, finally passing through the ileocaecal sphincter to the large intestine. to a large extent the separation of segmental contractions from peristaltic contractions is artificial as both serve to move chyme forward, and both add to mixing. Chyme moves down the small intestine at the rate of about 1 cm/min, so will reach the ileocaecal junction in 3–5 hours. It often stays there til the next meal the gastroileal reflex intensifies peristalsis in the distal ileum forcing chyme through the ileocaecal valve.
Intensity of peristalsis is controlled by both neuronal reflexes and hormones. Neuronal factors include distension of the intestine wall, but also distension of the stomach will also cause increased small intestine peristalsis. Both of these reflexes are mediated by the myenteric plexus.
Hormonal factors increasing peristalsis include gastrin, CCK, insulin, motulin and seretonin. Glucagon and secretin inhibit peristalsis
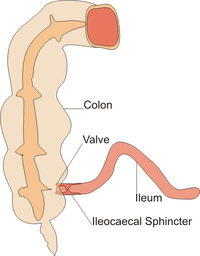
Ileocaecal valve
[edit | edit source]The prime function of the ileocaecal valve is to prevent reflux of fecal contents into the small intestine. As can be seen from the illustration, the valve protrudes into the caecum, thus increased caecal pressure will cause occlusion. Furthermore, the muscle is thickened for a few centimeters from the distal end of the ileum, and this acts as a functional sphincter.
Increased pressure or irritation in the distal ileum will cause relaxation of this sphincter; increased caecal preasure or irritation will cause constriction.
Large Bowel and Defecation
[edit | edit source]The principal function of the large intestine is to remove water and electrolytes from the chyme, and to store the resultant faeces until it can be eliminated.
In the colon the longitudinal muscle coat is condensed into three narrow bands called the taenia coli. Thus mixing movements of the circular muscle coat, so called haustrations predominate in the Large intestine. These will also slowly move the contents towards the rectum.
Much of the forward movement comes from these 'haustrations, but there is a third type of contraction called the mass movement which sends substantial amounts of material forward. These typically occur 2-3 times a day, usually after a meal - the so-called gastrocolic reflex, and last for about 20 minutes. They are responsible for the final formation of the faeces and the filling of the rectum.
Filling of the rectum is a signal for the relaxation of the Internal anal sphincter. However the External anal sphincter is under voluntary control.
Although the myenteric defecation signal only weakly relaxes the Internal anal sphincter, the stronger signal comes from parasympathetic reflexes synapsing in the sacral cord. These can be inhibited centrally, and when time to defecate is convenient, the inhibition is released, and the external anal sphincter, under voluntary control is relaxed.
The sequence of defecation is often initiated voluntarily; the epiglottis is closed a deep breath, and contraction of the abdominal muscles increase intra-abdominal pressure.
Coordination of motility
[edit | edit source]All these actions are coordinated, and are under control of hormones, and the autonomic nervous system as well as the enteric nervous system, the result is that in health food products and chyme are moved forward at the optimal rate to allow for efficient digestion and absorption.