Exercise as it relates to Disease/The role of strength training in managing Ehlers Danlos

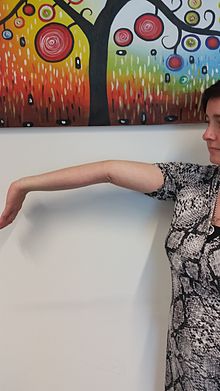


People who have a high degree of flexibility are often referred to as being 'double jointed'[1] which suggests two joints at one site however, is actually just having a joint that can extend beyond a normal range of movement. Being able to move a joint in a range greater than normal is not uncommon and not in itself a disease.[2] Where it can become an issue though is where this joint hypermobility is a result of a connective tissue disorder such as Marfan Syndrome, Benign Joint Hypermobility Syndrome (BJHS) or Ehlers Danlos Syndrome (EDS).
Ehlers Danlos Syndrome is a collection of connective tissue disorders that are hereditary and cause a mutation to genes that encode collagen or collagen-modifying enzymes. It has been described as an invisible musculoskeletal disease that is chronic, painful, debilitating and is early in onset.[3] Some clinical suggestions on treatment include palliative care which can be distressing to those newly diagnosed and so it is not uncommon for EDS patients who experience chronic pain and discomfort to seek the assistance of medical and allied health professionals.
While this condition was first named in 1949,[4] research and information is still scarce.[3][5] Australia has just hosted its' first EDS conference in July 2014 which was open to medical professionals, allied health professionals but perhaps more importantly, those suffering from EDS and their families. http://www.edsconference.com.au/2014/
Pathophysiology
[edit | edit source]Clinically it can be difficult to differentiate between EDS and BJHS and they can often be considered to be the same. A revised instrument for classification of BJHS, the Brighton Criteria was presented in 1998 and published in The Journal in 2000[6] which helped to create a separation between the two conditions.
The key diagnostic variation in assessment is that for BJHS, a score of four out of nine in the Beighton test is required whereas for EDS a score of five or more out of nine is indicative of the disease. Both conditions have a range of other associated major and minor indicators.[4]
The scoring criteria for the Beighton score[7] is shown in the table below and pictures demonstrating some of the tests are shown on the right.[8] The Beighton score can be categorised into three groups:
• 0-2 points not hypermobile
• 3-4 points moderately hypermobile
• 5-9 points distinctly hypermobile
| Criteria | Right | Left |
|---|---|---|
| Passive dorsiflexion of the little fingers beyond 90 degrees | 1 | 1 |
| Hyperextension of the elbows beyond 10 degrees | 1 | 1 |
| Passive apposition of the thumbs to the flexor aspect of the forearm | 1 | 1 |
| Hyperextension of the knees beyond 10 degrees | 1 | 1 |
| Forward flexion of the trunk with knees fully extended so that the palms of the hand rest flat* on the floor | 1 point if successful | - |
There are six categories of EDS each with similar core features however, some have potentially fatal variations such as the vascular type. These are:
• Classical Type
• Hypermobility Type
• Vascular Type
• Kyphoscoliosis Type
• Arthrochalasia Type
• Dermatosparaxis Type
• Tenascin-X Deficient Type [4][8][9]
The Hypermobility type is the most common form of EDS. Combined with the Classic type, these two forms account for around 90% of reported EDS cases.[3]
The Brighton Criteria for EDS expands on the Beighton score to include a set of major and minor criteria and helps to differentiate between the six types of EDS. To see all the variations of the criteria, visit the US based Ehlers-Danlos Syndrome Network at http://www.ehlersdanlosnetwork.org/typesofehlersdanlos.html. The criteria for the Hypermobility Type is shown below as an example of the improvement of diagnostic criteria beyond the Beighton score:
Major Diagnostic Criteria for the Hypermobility Type or EDS
• Joint hypermobility, which usually is confirmed by a score of five or more on the nine-point Beighton scale.
• Soft or velvety skin with normal or slightly increased extensibility.
• Absence of skin or soft tissue fragility, which is suggestive of other types of EDS.
• Molluscoid pseudotumors.
• Surgical complications, such as incisional hernia, wound dehiscence, or sutures tearing through tissues and failing to hold.
Minor Diagnostic Criteria for the Hypermobility Type of EDS
• Family history of similar features without significant skin or soft tissue fragility in a pattern consistent with autosomal dominant inheritance
• Recurrent joint dislocations or subluxations
• Chronic joint or limb pain
• Easy bruising
• Functional bowel disorders (functional gastritis, irritable bowel syndrome)
• Neurally mediated hypotension or postural orthostatic tachycardia
• High, narrow palate
• Dental crowding
Strength Training for EDS
[edit | edit source]Joint instability in those with EDS can occur anywhere and everywhere across the body with jaw, shoulders, wrists and fingers common in the upper body and hips, knees and ankles in the lower body.[5] This instability is commonly met with chronic musculoskeletal pain that most frequently involves the shoulders, hands, hips and knees.[3] As such, the primary role for strength training for people with EDS is to aid in joint stability and secondary to this is to improve proprioception throughout the body.[5]
A combination of the strength and endurance forms of strength training will help with stability and balance of those with EDS. It is important to note that those with EDS often suffer from poor sleep quality and experience a chronic level of fatigue in varying degrees of magnitude from day to day.[3] Accordingly, it is important to commence each session with a survey of the general health and wellbeing of the person to assess for daily pain level and locations as well as fatigue.
Studies have found that resistance training using unstable platforms, rubber tubing, modified body weight functional movement and hydrotherapy resistance work helps to improve joint stability, balance and emotional wellbeing of those challenged with EDS.[3][5][10] Low repetitions and a low number of sets will help to ensure that fatigue doesn’t interfere with correct performance of the exercises. Training a person to one repetition max or to failure is strongly discouraged as it presents a high risk of injury in those without stable joints.
Considerations for strength training
[edit | edit source]Due to the ease of full or partial dislocations of joints, heavy loading of the musculoskeletal structure and isometric exercises should be avoided.[11] Often those suffering with EDS will not even realise they have hyperextended a joint because the lax nature of their connective tissue and poor proprioception will fail to signal to their body that a dislocation has occurred.[5] There also may be little to no swelling and little or no discomfort. As a result, people with EDS should work one on one with an experienced professional who can guide them in steady and controlled movements and identify for them that a the range of motion has been exceeded.
The Vascular type of EDS presents an increased risk with strength work as it effects the connective tissue in blood vessels and internal organs.[4][8] This type of EDS is the most serious with diagnosis requiring genetic studies of the patient. Often patients can be misdiagnosed with another form of EDS. The most serious complication of the Vascular type of EDS is unpredictable ruptures of arteries and organs which can lead to death. Straining to lift weights for people with this type of EDS can prove fatal.
Contraindications for exercise
[edit | edit source]Those diagnosed with or who have a suspected diagnosis of EDS should not be prevented from exercise. Being active can not only aid in the reduction of risk of an injury but also help to improve general health and wellbeing.[4][12] If the person finds that certain exercise movements or sporting activities cause pain in any aspect of their body that is not related to fitness, then they should stop these activities and seek advice on mitigating, where possible, the onset of pain for future involvement.
It is important is to avoid overstretching joints. Swimming and aquatic based activities can help as the weight of their body is supported by water however, breaststroke can irritate the knees and hips and should be avoided.[13][14]
Further information
[edit | edit source]Support Groups and information in Australia
[edit | edit source]EDSAUS - Ehlers Danlos Syndrome Support in Australia
Joint Pain Relief
Ehlers-Danlos and Joint Hypermobility Syndrome Australia Facebook Group
Support Groups and information overseas
[edit | edit source]Mayo Clinic
The Ehlers-Danlos National Foundation
U.S. National Library of Medicine - PubMed Health
Ehlers-Danlos Support UK
Ehlers-Danlos Foundation of New Zealand
References
[edit | edit source]- ↑ Cashin-Garbutt, A; 2014 'Double-Jointed - Joint Hyperlaxity/Hypermobility'; http://www.news-medical.net/health/What-is-Double-Jointed.aspx
- ↑ Zweers, M.C. et al (2005) 'Tenascin-X: a candidate gene for benign joint hypermobility syndrome and hypermobility type Ehlers-Danlos syndrome?' Annals of the Rheumatic Diseases. 2005;64(3):504 –505
- ↑ a b c d e f Voermans, Nicol C., et al.; 2010 'Pain in Ehlers-Danlos syndrome is common, severe, and associated with functional impairment' Journal of pain and symptom management 40.3: 370-378.
- ↑ a b c d e Schroeder, Erik L., and Mark E. Lavallee.; 2006, 'Ehlers-Danlos syndrome in athletes', Current sports medicine reports 5.6: 327-334.
- ↑ a b c d e Rombaut, Lies, et al.; 2011 'Medication, surgery, and physiotherapy among patients with the hypermobility type of Ehlers-Danlos syndrome', Archives of physical medicine and rehabilitation 92.7: 1106-1112.
- ↑ Rheumatol, J.; 2007 'The need to take a fresh look at criteria for hypermobility.' The Journal of Rheumatology; vol34no.4;664-665
- ↑ Smits-Engelsman, B; 2011 'Beighton Score: A Valid Measure for Generalized Hypermobility in Children', The Journal of Pediatrics, 158.1: 119-123.
- ↑ a b c Paepe, Anne De, and Fransiska Malfait.; 2004,'Bleeding and bruising in patients with Ehlers–Danlos syndrome and other collagen vascular disorders.' British journal of haematology 127.5: 491-500.
- ↑ Ehlers-Danlos Syndrome Network http://www.ehlersdanlosnetwork.org/typesofehlersdanlos.html
- ↑ Anderson, K. and Behm, DG; 2005, 'The impact of instability resistance training on balance and stability.' Sports Medicine 35.1: 43-53.
- ↑ Ehlers Danlos Support UK: http://www.ehlers-danlos.org/what-is-eds/types-of-eds
- ↑ Whitelaw, Sara E.; 2002, 'Ehlers-Danlos Syndrome, classical type: case management' Pediatric nursing 29.6: 423-426.
- ↑ Panni, Alfredo Schiavone, et al.; 2006, 'Patellofemoral problems' Football Traumatology. Springer Milan. 263-274.
- ↑ Beighton, P; et al.; 2012, 'Hypermobility in the performing arts and sport' Hypermobility of Joints. Springer London, 125-149.