Exercise as it relates to Disease/Testosterone supplementation: improving mortality in men with chronic obstructive pulmonary disease through resistance training
What is the background to this research?
[edit | edit source]COPD is a progressive disease which makes it harder and harder to breathe. the term progressive is used as it gets worse over time if left untreated.[1] with the rising death rates associated with COPD (11% from 1999-2009[2]), some interventions need to be found to cure or at least help to slow the progression of this disease and improve quality of life of those suffering. Patients with Chronic Obstructive Pulmonary Disease (COPD) have said that exercise intolerance is their number one complaint,[3] dysfunction in the muscles is what contributes mostly to this complaint.[4] Dysfunction of the muscles is very easy to cure or at least improve function through rehabilitative exercise training programs. The choice of a resistance training intervention was to improve muscle mass and muscle strength in functional movements for men with COPD to help improve exercise tolerance.
Where is the research from?
[edit | edit source]This research was conducted by Richard Casaburi et al, at various colleges and institutions throughout the United States including Los Angeles and California.
What kind of research was this?
[edit | edit source]The research was a random control trial. It involved participants being in 4 different groups to test the effects of each intervention.
What did the research involve?
[edit | edit source]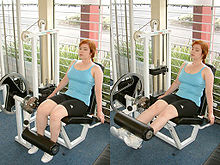
The research involved 53 male patients with stable COPD within the age of 55-80 taking part in 4 different interventions. Groups: 1. Placebo injections and no resistance training 2. Testosterone injections and no resistance training 3. Placebo injections and resistance training 4. Testosterone injections and resistance training Subjects received injections 100 mg/week of either testosterone enanthate in sesame oil or the placebo (sesame oil). The resistance training consisted of 3 supervised sessions per week with training consisting of seated leg press, seated leg curl, seated leg extension, standing calf raise, and seated ankle dorsiflexion. Training sets for each exercise remained at 3 while rep range was anywhere between 8-12, progressing throughout the program. This resistance training focused on muscles of ambulation. Outcome measures included Body composition analysis, Muscle strength and local muscle fatigability, Whole-body exercise endurance & Pulmonary function testing/arterial blood gas analysis
What were the basic results?
[edit | edit source]Group 4 yielded superior muscle mass and strength gains than the other 3 groups. This shows that the combined intervention worked. Leg extensor strength was improved which is crucial for everyday activities e.g standing from a chair. Although all groups, except the placebo + no training group, experienced strength gains, the whole body endurance measure was only significantly higher for group 4. Given that low muscle mass is a predictor of mortality in men with COPD, these muscle hypertrophy interventions should be implemented into a rehabilitation programs.
How did the researchers interpret the results?
[edit | edit source]The researchers involved concluded that there are positive benefits to resistance training and testosterone supplementation for men with COPD in terms of mortality. They also suggested more research should be directed towards this method in conjunction with endurance training to see the effects of both.
What conclusions should be taken away from this research?
[edit | edit source]Given that low muscle mass is a predictor of mortality in men with COPD,[6][7] these muscle hypertrophy interventions should be implemented into a rehabilitation programs. Over the 10 week intervention period, no adverse affects were seen by the men subjected to testosterone supplementation which indicates it may be safe to use. Given that group 2 experienced slightly higher strength gains then group 3, this supplementation method could be useful for future rehabilitation programs with patients that cannot exercise at the beginning of treatment. ==
What are the implications of this research?
[edit | edit source]Resistance training could also be another way of helping patients with COPD improves quality of life. Although many studies have been conducted to suggest endurance training is the best method,[8] these researchers have shown that there may be other ways to rehabilitate these patients safely with low risk.
References (including the primary reference that this fact sheet relates to)
[edit | edit source]References
[edit | edit source]- ↑ What Is COPD? National Heart, Lung and blood institute July 31, 2013 access here: http://www.nhlbi.nih.gov/health/health-topics/topics/copd
- ↑ Trends in COPD (Chronic Bronchitis and Emphysema): Morbidity and Mortality, Epidemiology and Statistics Unit, Research and Health Education Division, March 2013.
- ↑ Casaburi R et al. (1993) Exercise training in chronic obstructive lung disease. In: Casaburi R, Petty TL, editors. Principles and practice of pulmonary rehabilitation. Philadelphia: Saunders; p. 204–224.
- ↑ Maltais F et al. (2014)An official American Thoracic Society/European Respiratory Society statement: update on limb muscle dysfunction in chronic obstructive pulmonary disease. Am J Respir Crit Care Med;189(9):e15-62.
- ↑ Emily,15 January 2005 (original upload date)
- ↑ Casaburi, R et al. (2004) Effects of Testosterone and Resistance Training in Men with Chronic Obstructive Pulmonary Disease, ATS Journals, Pp 870- 877
- ↑ Marquis K et al., (2002) Midthigh muscle cross-sectional area is a better predictor of mortality than body mass index in patients with chronic obstructive pulmonary disease. Am J Respir Crit Care Med;166:809–813.
- ↑ Ortega F, et al. (2002) Comparison of effects of strength and endurance training in patients with chronic obstructive pulmonary disease. . Am J Respir Crit Care Med 2002;166:669–674.