Exercise as it relates to Disease/Osteoarthritis and Resistance Training as an Intervention Strategy

This fact sheet has been written for those people suffering or affected by osteoarthritis. It provides background information of osteoarthritis and the current treatment and prevention strategies, more specifically resistance training for treatment and prevention. This fact sheet also provides details on where to find further information on osteoarthritis.
What is osteoarthritis (OA)?
[edit | edit source]Osteoarthritis (OA) is the most common form of arthritis. It is a chronic joint disorder that is the most common cause of joint pain and joint disability. It is characterised by the break down of joint cartilage that usually protects the bones joints allowing it to move freely. The joints that are more commonly affected are the spine, hands, hips and knees. In OA, the breakdown of joint cartilage leaves the bones exposed and unprotected resulting in damage that decreases the joints ability to move freely. Accompanying the loss of movement is a decreased ability to carry out daily tasks and normal living, resulting in a decreased quality of life for the individual.[1]
What are the symptoms of OA?
[edit | edit source]The symptoms of OA can vary between sufferers. The symptoms that you experience will sometimes depend on which joints are causing you discomfort. The development of OA is a progressive disease, usually over several months or several years. Joint pain and stiffness are the most common complaints from sufferers of OA. You may experience over symptoms such as a reduction in range of movement (ROM), decrease muscle mass (muscle atrophy), joint swelling and physical disability. These symptoms may become worse when you are inactive for extended periods of time, such as driving for long periods of time.[2][3][4]
What are the risk factors of OA?
[edit | edit source]The cause of OA is not yet clear, but research shows that there are certain factors that increase the risk of developing OA in certain joints, these include:
- knees: previous injuries, occupation e.g. carpet layers, being overweight, repeated overuse, muscle weakness due to minimal physical activity, genetics and aging.
- hips: previous injuries, occupation e.g. removalist, being overweight and aging.
- hands: previous injuries, heredity, repeated overuse and aging.
What are the chances I develop OA?
[edit | edit source]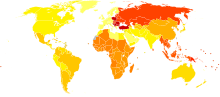
The chances of you developing OA increases with age. Research shows 5% of the entire population below 40 are affected by OA, this increases dramatically to 10% of males and 20% of females aged 45–65 years, and then further to affect more than 50% of women aged 85 years and over. OA can not only affect you via the cost of medicines and surgery but may affect you indirectly, such as loss of income, lost productivity, pain, disability, emotional impairment, impaired social function and other health-related quality of life issues.[5][6][7]
What are the treatment and prevention for OA?
[edit | edit source]The overall goal, since there is no cure, is to reduce pain, improve overall function of the joints that are affected and more importantly eliminate the risks of you developing OA. You can meet these goals through the following methods of intervention:
- Pharmacological - drug therapy, such as non-steroidal anti-inflammatory drugs (NSAIDs), glucosamine, chondroitin sulfate and paracetamol for pain relief.
- Non-Pharmacological – exercise therapy, such as resistance training for muscle strengthening, aerobic training for weight loss.
- Surgical - joint replacement surgery, usually the last option if the symptoms can no longer be controlled by pharmacological and non-pharmacological preventions and treatments.
What is resistance training and how does it help?
[edit | edit source]Resistance training is any exercise that causes your muscles to contract against a resistance. The expectation is an increase in strength, tone, mass, and/or endurance for muscle and bone. It has been reported that exercise, predominantly dynamic strengthening exercises, provides benefits for pain and function of patients suffering from knee and hip OA. Activities that are likely to be good for your fitness include walking, swimming, water exercise, low-impact aerobics, and riding a bike or exercise bike. Your physiotherapist can also suggest specific exercises and stretches that are appropriate for your situation.[8][9]
What resistance exercises can I do to help?
[edit | edit source]Below you will find a list of exercises you can complete at home on a regular basis that will help you prevent and manage the onset of OA. These exercises are targeted at strengthening the muscles surrounding the hip and knee joints which are common sites affected by OA. They will help in reducing pain, increasing movement of the joint and increasing your ability in the gait cycle (walking).
What else can I do?
[edit | edit source]- For more exercises to help reduce pain and improve mobility consult your doctor/physician as they will help you get the right treatment to manage your symptoms.
- Play an active role and learn about the treatments and preventions of OA.
- Eat healthy as this will help you with weight loss if your weight is a problem.
- Lead an active lifesyle as exercise is highly recommended for people with OA.
Where can I get further information on OA?
[edit | edit source]For further information on prevention and treatment for OA, more specifically resistance training and its effectiveness, refer to the following resources:
| - The Arthritis Foundation (US) www.arthritis.org | - Arthritis Queensland www.arthritis.org.au |
| - Taking control of your Osteoarthritis | - Information on Osteoarthritis www.healthinsite.gov.au |
| - Healthy eating and further exercises www.healthyactive.gov.au | - World Health Organisation (WHO) www.who.int |
| - For your local Arthritis Office: 1800 011 041 OR www.arthritisaustralia.com.au |
References
[edit | edit source]- ↑ Jamtvedt, G, Dahm, KT, Christie, A, Moe, RH, Haavardsholm, E, Holm, & Hagen KB 2008 ‘Physical Therapy Interventions for Patients With Osteoarthritis of the Knee: An Overview of Systematic Reviews’, Physical Therapy, vol. 88, pp. 123-136. http://www.ncbi.nlm.nih.gov/pubmed/17986496
- ↑ http://www.arthritisaustralia.com.au/images/stories/documents/info_sheets/english/colour/template_Osteoarthritis.pdf
- ↑ http://www.arthritis.org/media/newsroom/media-kits/Osteoarthritis_fact_sheet.pdf
- ↑ http://www.arthritis.org/media/newsroom/media-kits/Osteoarthritis%20fact%20sheet%20from%20AF-Final%2012_10_09.pdf
- ↑ http://www.abs.gov.au/ausstats/abs@.nsf/mf/4823.0.55.001
- ↑ http://web.archive.org/web/20080729084239/http://www.health.gov.au/internet/main/publishing.nsf/content/AD383BF1A9E16D5BCA25711A007AF405/$File/evid4.pdf
- ↑ http://www.mja.com.au/public/issues/180_05_010304/mar10381_fm.html
- ↑ Maura Daly Iversen, Therapeutic Advances in Musculoskeletal Disease 2010 2: 279
- ↑ Taking Control of your Osteoarthritis, Arthritis Australia, http://www.arthritisaustralia.com.au/images/stories/documents/booklets/2011_updates/Taking_control_of_your_Ostoarthritis_booklet.pdf
- ↑ Silva, LE, Valim, V, Pessanha, APC, Oliveira, LM, Myamoto, S, Jones, A & Natour J 2008 ‘Hydrotherapy Versus Conventional Land-Based Exercise for the Management of Patients With Osteoarthritis of the Knee: A Randomized Clinical Trial’, Physical Therapy, vol. 88, pp. 12-21. http://www.ncbi.nlm.nih.gov/pubmed/17986497